Impact of off-pump coronary artery bypass grafting on survival: current best available evidence
Introduction
For decades, cardiac surgeons have performed coronary surgery with cardiopulmonary bypass (CPB) and cardioplegia-induced cardiac arrest, the on-pump technique (ONCAB), which provides a motionless and bloodless surgical field, this at the expense of potentially negative sequelae including blood trauma, activation of systemic inflammatory responses, non-pulsatile flow, aortic cannulation and clamping with possible embolization of air or atherosclerotic debris and systemic hemodilution (1).
Because of these detrimental aspects, ONCAB has been challenged in recent years by off-pump coronary artery bypass surgery (OPCAB), which avoids the use of CPB. This has triggered a large number of randomized clinical trials (RCTs) and retrospective analyses addressing the clinical outcomes of the two techniques. There seems to be convincing evidence that OPCAB reduces the risk of early postoperative morbidity such as myocardial infarction, pulmonary dysfunction, abnormal renal function, atrial fibrillation, blood product transfusion, intensive care unit and hospital stay (2-14). However, concerns persist with respect to the impact of OPCAB on long-term mortality and freedom from re-intervention (15-18) with some studies reporting a higher risk of incomplete revascularization and graft failure (19,20). Despite the potential benefits of OPCAB, recent data shows that only a minority of CABG operations worldwide (about 15% to 20%) are carried out with this technique (21).
Surgeons might be reluctant to commit to OPCAB because of concerns that the technique requires distal anastomoses to be performed on the beating heart, potentially compromising long-term graft patency. These concerns seem not to apply in large-volume centers and for surgeons who have crossed their learning curve (22,23).
Methods
We conducted a literature search through PubMed, EMBASE, the Web of Science, the Cochrane Library and Google Scholar. No language, publication date or publication status was imposed. Suitable papers were individually analyzed and results were tabulated in a spreadsheet to categorize and organize the information. The main articles were presented as well in a table (Table 1).
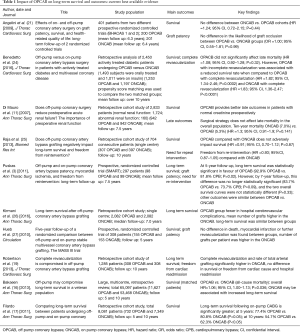
Full table
Results
A general view of recent randomized controlled trials
The largest trials until now are the Randomized On/Off Bypass (ROOBY) trial (28) and the CABG Off or On Pump Revascularization Study (CORONARY) (29).
The ROOBY trial enrolled 2,203 patients from the Veterans Affairs (VA) system scheduled for urgent or elective CABG to either OPCAB or ONCAB. The primary long-term end point was a composite of death from any cause, a repeat revascularization procedure, or a nonfatal myocardial infarction within 1 year after surgery. The results showed a significantly higher rate of the composite long-term outcome with OPCAB when compared with ONCAB (9.9% vs. 7.4%; RR =1.33; 95% CI, 1.01–1.76; P=0.04). The 1-year patency rate of arterial grafts was lower in OPCAB (92.9%) than ONCAB (94.8%) although this difference was not statistically significant (P=0.13).
Recently, the results of the CORONARY trial at 1 year have been published (29): authors compared OPCAB with ONCAB in 4,752 patients from 19 countries on 5 continents. They found no significant differences between groups at 1 year in the rate of the first co-primary outcome of death, nonfatal stroke, nonfatal myocardial infarction, or nonfatal new renal failure requiring dialysis (HR =0.91; 95% CI, 0.77–1.07; P=0.24). The rate of repeat coronary revascularization at 1 year was 1.4% in the OPCAB group and 0.8% in the ONCAB group (HR =1.66; 95% CI, 0.95–2.89; P=0.07).
It is quite evident that there are notable differences between the two trials; CORONARY included more than twice as many participants than the ROOBY; furthermore, the participants in the CORONARY represented altogether a more heterogeneous group, whereas the ROOBY trial recruited patients exclusively from the VA system. The CORONARY specified a higher level of surgical ability at the beginning of the trial than was required in the ROOBY; each operation was performed by a surgeon who had more than 2 years of experience and had completed more than 100 cases of the specific technique (either OPCAB or ONCAB). In CORONARY, trainees were not allowed to be the primary surgeon. The rate of conversion from OPCAB to ONCAB was lower in CORONARY than in the ROOBY (7.9% vs. 12.4%), and the rate of repeat revascularization between 31 days and 1 year was also lower in CORONARY (0.7% in the OPCAB and 0.6% in the ONCAB vs. 4.6% and 3.4%, respectively). Interestingly, in CORONARY, the rate of the primary end point was lower in the OPCAB group than in the ONCAB group (11.5% and 13.2%, respectively; P=0.08), whereas in the ROOBY, the rate was lower in the ONCAB group (9.4% in the OPCAB group vs. 7.1% in the ONCAB group; P=0.08).
The most recent Cochrane Review on OPCAB versus ONCAB (30), which did not include the CORONARY trial, was strongly influenced by the results from the ROOBY trial and concluded that OPCAB did not confer any significant benefit compared with ONCAB in relation to mortality, stroke or myocardial infarction. The authors observed better long-term survival in the group of patients undergoing ONCAB. Based on the current evidence, they suggested ONCAB to continue to be the standard surgical treatment, and OPCAB to be acceptable when there are contraindications for cannulation of the aorta and CPB.
A previous meta-analysis of propensity score analyses published by Kuss et al. (12) showed results contrasting the Cochrane Review conclusions: a total of 35 out of 58 initially retrieved propensity score analyses were included, accounting for a total of 123,137 patients. The ROOBY trial was not enrolled in this meta-analysis. The estimated overall OR was less than 1 for all outcomes, favouring OPCAB. This benefit was statistically significant for mortality (OR =0.69; 95% CI, 0.60–0.75), stroke, renal failure, red blood cell transfusion (P<0.0001), wound infection (P<0.001), prolonged ventilation (P<0.01), inotropic support (P=0.02), and intra-aortic balloon pump support (P=0.05). The odds ratios for myocardial infarction, atrial fibrillation, and reoperation for bleeding were not significant. These results agree with previous systematic reviews of randomized and nonrandomized trials (4).
Best available evidence for long-term survival
The increasing availability of longer-term data now requires follow up analysis; recent studies and meta-analysis have focused on long-term survival and major secondary outcomes in OPCAB vs. ONCAB within the general population (31).
Our group has previously reported the results from two prospective, randomized, controlled trials the Beating Heart Against Cardioplegic Arrest Study (BHACAS) 1 and 2 trials (23): 401 participants were recruited overall, of whom 200 patients had OPCAB and 201 patients underwent ONCAB surgery. The patients were followed up for 6 to 8 years after surgical intervention to assess graft patency, major adverse cardiac-related events (MACEs), and health-related quality of life (HRQoL). Patency was assessed using multidetector computed tomographic coronary angiographic analysis with a 16-slice scanner. Two blinded observers classified the proximal, the body and the distal segments of each graft as occluded or patent. MACEs and HRQoL were obtained from questionnaires given to participants and family practitioners. The mean follow-up period for OPCAB and ONCAB survival was 6.3 and 6.4 years, respectively, and survival-free from MACEs or death was 5.4 and 5.2 years, respectively. The key findings (6 to 8 years after surgical intervention) are that there were no differences between the OPCAB and ONCAB groups in the hazard of death (HR =1.24; 95% CI, 0.72–2.15; P=0.44) or survival free from MACEs or death (HR =0.77; 95% CI, 0.58–1.24; P=0.39). Patency was studied in 199 out of 349 and HRQoL was studied in 299 out of 349 survivors. There was no evidence of attrition bias. The likelihood of graft occlusion was no different between OPCAB (10.6%) and ONCAB (11.0%) groups (OR =1.00; 95% CI, 0.55–1.81; P>0.99). Graft occlusion was more likely at the distal than the proximal anastomosis (OR =1.11; 95% CI, 1.02–1.20).
More recently, our group reported a retrospective analysis of long term survival in actively treated diabetic patients undergoing OPCAB versus ONCAB (24). The final population consisted of 2,450 patients; of those, 1,493 subjects were orally treated and 1,011 were on insulin. OPCAB and ONCAB were performed in 1,253 and 1,197 patients respectively. Propensity score matching was used to compare the two groups. The results showed that OPACB did not significantly affect late mortality (HR =1.08; 95% CI, 0.92–1.28; P=0.32). However, OPCAB with incomplete revascularization was associated with a reduced survival rate when compared to OPCAB with complete revascularization (HR =1.82; 95% CI, 1.34–2.46; P=0.0002) and ONCAB with complete revascularization (HR =1.83; 95% CI, 1.36–2.47; P<0.0001). Di Mauro et al. (11) conducted a retrospective cohort study of 2,833 patients with multivessel coronary disease. Two analyses comparing OPCAB and ONCAB were created with respect to preoperative normal and abnormal renal function: one analysis included 1,724 (862 each group) out of 2,618 patients with normal preoperative creatinine (<1.5 mg/dL), and the second analysis included 160 (80 each group) out of 215 patients with preoperative abnormal renal function; in both analyses matched groups were selected applying propensity score. Mean follow up was 7.5 years. Ten-year mortality did not show any significant difference between ONCAB (7.0%) vs. OPCAB (5.3%) (HR =1.3; 95% CI, 0.91–1.9; P=0.141). The authors concluded that OPCAB provides better late outcomes in patients with normal creatinine preoperatively, but similar outcomes for those with abnormal creatinine levels. The occurrence of acute renal failure significantly impairs early and long-term mortality and the surgical strategy does not influence late mortality in the overall population.
Raja et al. (25) reported the results of a retrospective cohort study of 704 consecutive patients with multivessel disease; 307 patients had OPCAB and 397 underwent ONCAB. The 307 OPCAB patients were propensity score matched to 307 ONCAB patients. The follow-up at 10 years was 100%. Survival was similar for the two cohorts. After adjusting for clinical covariates, OPCAB did not emerge as a significant independent predictor of long-term mortality (HR =0.91; 95% CI, 0.70–1.12), readmission to hospital for cardiac cause (HR =0.96; 95% CI, 0.78–1.10), or the need for re-intervention (HR =0.93; 95% CI, 0.87–1.05). OPCAB compared with ONCAB did not adversely impact on survival or freedom from re-intervention at 10-year follow-up.
Puskas et al. (3) reported the results of their prospective, randomized controlled trial [The Surgical Management of Arterial Revascularization Therapies (SMART) trial], enrolling 297 unselected patients with multivessel CAD. Of 140 survivors, 87 volunteered to return after a minimum of 6.8 years (maximum, 8.4 years; mean, 7.5 years) for assessment of graft patency and myocardial ischemia. Age at follow-up ranged from 38 to 90 years (mean, 68 years). There were 26 deaths from all causes among OPCAB patients and 31 among ONCAB patients. Graft patency was similar between groups among 622 grafts assessed by angiography before hospital discharge (99% OPCAB vs. 97.7% ONCAB; P=0.22), among 511 grafts assessed by angiography at 1 year (93.6% OPCAB vs. 95.8% ONCAB; P=0.33), and among 190 grafts assessed by computed tomographic angiography at late follow-up (76% OPCAB versus 83.5% ONCAB; P=0.44). Twelve out of 34 OPCAB (35.3%) and 16 out of 39 ONCAB patients (41.0%) had any ischemia on positron emission tomography scanning (P=0.62). Four OPCAB patients (11.8%) and 9 ONCAB patients (23.1%) had an ischemic region in excess of 10% of myocardium (P=0.21). At late follow-up, recurrent angina had occurred in 11 of 43 (25.6%) OPCAB patients and 5 of 44 (11.4%) ONCAB patients (P=0.09). Percutaneous re-intervention had been performed at the discretion of blinded local cardiologists in 1 of 43 (2.3%) OPCAB patients and 1 of 44 (2.3%) ONCAB patients (P=1.0). No patient in either group has undergone repeat CABG. The authors concluded that OPCAB and ONCAB were associated with similar early and late graft patency, incidence of recurrent or residual myocardial ischemia, need for re-intervention, and long-term survival.
Kirmani et al. (26) recently presented the results of a retrospective cohort study of patients undergoing isolated CABG at a single centre. A total of 8,055 patients were identified, with a median follow-up of 7.0 years. Propensity score matching was performed on the basis of on demographic variables and two groups of 2,082 patients for both OPCAB and ONCAB were obtained. The results showed that in the OPCAB group, there were significantly fewer in hospital cerebrovascular complications (0.5% vs. 1.1%; P=0.017), and mean length of stay was shorter (7.6 vs. 8.1 days; P<0.0001). The mean number of grafts was higher in the ONCAB group (3.28±0.94 vs. 3.10±1.10; P<0.0001). The authors concluded that despite a lower mean number of grafts, long-term survival after OPCAB was not inferior to long-term survival after ONCAB (P=0.167).
Hueb et al. (27) reported the results of a prospective, randomized controlled trial (MASS III) of 308 patients undergoing CABG. Of those patients, 155 underwent OPCAB and 153 had ONCAB. The follow-up was at 5 years. Primary composite end points were death, myocardial infarction, further revascularization (surgery or angioplasty), or stroke. After 5-year follow-up, the primary composite end point was not different between groups (HR =0.71; 95% CI, 0.41–1.22; P=0.21). The number of grafts per patient was higher in the ONCAB than the OPCAB group (2.97 vs. 2.49 grafts/patient; P=0.001). The authors concluded that no difference was found between groups in the primary composite end point at 5-year follow-up. Although OPCAB surgery was related to a lower number of grafts and higher episodes of atrial fibrillation, it had no significant implications related to long-term outcomes.
Similar results were demonstrated by Robertson et al. (19) in a retrospective cohort study of 1,285 patients. Following propensity-score matching for baseline characteristics, they reviewed the results of 308 patients undergoing OPCAB compared with 308 patients who had ONCAB. Survival and readmission for cardiac causes were monitored for up to 10 years postoperatively, with a median follow-up period of 5.9 years. The frequency of complete revascularization was significantly different between the 2 groups (OPCAB, 79.2% vs. ONCAB 88.3%; P=0.002). The OPCAB group had a significantly higher rate of total arterial grafting (OPCAB, 66.6% vs. ONCAB, 49.7%; P=0001). No difference was seen in 8-year survival or freedom from cardiac cause and hospital readmission between the 2 groups.
Bakaeen et al. (16) recently published the results of their large multicentre retrospective review of all primary isolated CABG procedures performed at VA hospitals during a 13.5-year period. Their objective was to compare risk-adjusted long-term survival between patients who underwent ONCAB vs. OPCAB. Using VA Continuous Improvement in Cardiac Surgery Program, they identified all VA patients (n=65,097) who underwent primary isolated CABG from October 1997 to April 2011. The primary outcome measure was all-cause mortality. A greedy-match algorithm using the propensity scores matched 8,911 OPCAB with 26,733 ONCAB patients.
For the matched cohort, the median follow-up was 6.7 years (interquartile range, 3.72–9.35 years). Risk-adjusted mortality did not differ significantly between the OPCAB and ONCAB groups at 1 year (4.67% vs. 4.78%; RR =0.98; 95% CI, 0.88–1.09) or 3 years (9.21% vs. 8.89%; RR =1.04; 95% CI, 0.96–1.12). However, risk-adjusted mortality was higher in the OPCAB group at 5 years (14.47% vs. 13.45%; RR =1.08; 95% CI, 1.02–1.15) and 10 years (25.18% vs. 23.57%; RR =1.07; 95% CI, 1.03–1.12). Overall, the hazard ratio for OPCAB vs. ONCAB was 1.06 (95% CI, 1.00–1.13; P=0.04).
They concluded that OPCAB may be associated with decreased long-term survival.
Filardo et al. (17) published a retrospective cohort study of 8,081 consecutive patients; 732 patients had OPCAB, 7,349 underwent ONCAB. A propensity-adjusted model controlling for preoperative risk factors identified by the Society of Thoracic Surgeons (STS) and other preoperative clinical and nonclinical details was used to assess adjusted long-term mortality differences between OPCAB and ONCAB. Their results showed that ten-year unadjusted survival was 54.7% (95% CI, 47.2–61.6%) in OPCAB patients and 62.3% (95% CI, 60.9–63.8%) in ONCAB patients. The log-rank test (P=0.012) indicated a significantly higher risk of death in OPCAB patients. After adjustment, the risk of death remained significantly higher in the OPCAB patients (HR =1.18; 95% CI, 1.02–1.38). The authors concluded that for multivessel coronary disease, ONCAB might be preferable to OPCAB given that it may achieve a more complete and durable revascularization.
Takagi et al. (15) recently published the results of a meta-analysis including 5 randomized controlled trials and 17 observational studies, enrolling a total of 104,306 patients. A pooled analysis of all 22 studies demonstrated a statistically significant 7% increase in long-term all-cause mortality with OPCAB relative to ONCAB (HR =1.07; 95% CI, 1.03–1.11; P=0.0003). Although a pooled analysis of 5 randomized trials (1,486 patients) demonstrated a statistically nonsignificant 14% increase in mortality with OPCAB relative to ONCAB (HR =1.14; 95% CI, 0.84–1.56; P=0.39), another pooled analysis of 17 observational studies (102,820 patients) demonstrated a statistically significant 7% increase in mortality with OPCAB relative to ONCAB (HR =1.07; 95% CI, 1.03–1.11; P=0.0004). The authors concluded that OPCAB is likely associated with worse long-term (>5-year) survival compared with ONCAB.
The findings of this meta-analysis must be interpreted with caution as the results are strongly influenced by the ROOBY trial (28) which, as already mentioned, has received a lot of criticism and has several important limitations.
Discussion
There has been increasing interest in OPCAB over the last two decades on the basis of the clinical advantages attributed to avoiding CPB during CABG. The most notable merits, as suggested by several observational studies, included avoiding embolic stroke caused by invasive aortic manipulation and reducing coagulopathy and renal dysfunction (2-14). However, the expected benefit on long term survival is still debated. To date, results of the largest randomized trials are limited to within 1 year of surgery and the long term comparative data regarding clinical outcomes between the 2 strategies are currently unavailable (28,29).
Despite initial enthusiasm, concerns have been raised regarding the risk of incomplete revascularization and higher rate of graft failure with OPCAB. These potential drawbacks have been related to poorer long term survival after OPCAB reported in sporadic studies (16,17).
Incomplete revascularization of patients with multivessel coronary artery disease is an independent risk factor for increased long-term mortality after CABG (32) and has been related to inferior cardiac survival after 5 years of follow-up compared with complete revascularization (33). The criticism regarding completeness of revascularization with OPCAB seems no longer valid in the current era as technology to securely perform multivessel OPCAB has improved significantly; in fact, the majority of evidence from randomized trials suggests at least equivalent completeness of revascularization with OPCAB and ONCAB (3,8,29,30). It is interesting to note that in those trials where OPCAB was associated with incomplete revascularization it is impossible to determine myocardial viability in the territory left ungrafted, because myocardial viability studies were not used, so the significance of a reduced number of grafts in the OPCAB cohort is uncertain. Moreover, none of the trials or studies reporting incomplete revascularization provides an explanation for failure to completely revascularize the OPCAB group.
In our review, most of the available comparisons found similar survival rates after OPCAB vs. ONCAB, especially when OPCAB is performed in high volume centres, thus supporting the view that OPCAB is as effective as ONCAB in terms of late survival. It should be underlined that substantial variability between the studies in terms of risk profile, selection criteria and expertise of surgeons limits the generalizability of any conclusions. The frequency of complete revascularization reported by different studies comparing OPCAB and ONCAB is strongly influenced by relative experience with each technique of the reporting centre and surgeon, highlighting once more the importance of a learning curve as well as case load. These differences can also have an impact on the final completeness of revascularization achieved by multicentre randomized trials.
Graft failure is one of the major determinants of clinical prognosis after CABG. There has been considerable concern among surgeons and cardiologists that the higher technical difficulty of OPCAB might translate into less precise anastomoses and subsequently reduced graft patency (34). A precipitous learning curve, distractions caused by cardiac motion or pulmonary insufflations, and performing the anastomoses on a moving target have been considered as factors accountable for poorer graft patency after OPCAB (35). Interestingly, the concerns about suboptimal graft patency over the last years have been largely influenced by the results of the ROOBY trial (28), whose findings have been strongly criticised since the 53 participating surgeons enrolled on average only eight patients per year during the study period and had unacceptably high conversion rates to on-pump surgery (12%) and incomplete revascularization (18%). Moreover, in 60% of the cases a junior resident was the primary surgeon. Another unrecognized confounder that contributed to poor graft patency in the ROOBY trial was the concomitant use of endoscopic vein harvesting (EVH) in 1,471 patients (ONCAB =907 and OPCAB =564). The incidence of a patient having 1 or more occluded saphenous vein grafts on follow-up angiography was 41.3% in the EVH group, compared with 28.0% in the open vein harvesting (OVH) group (P<0.0001). Since ROOBY trial was recruiting at a time when EVH was not being widely practiced, the poor vein graft patency secondary to EVH can be attributed to the learning curve and relative inexperience of the vein harvesters. Poor conduit quality, an unavoidable consequence of the learning curve for EVH, has been found to be a significant predictor of early graft failure (36).
Conclusions
In view of the increasing risk profile of patients currently referred to coronary artery bypass surgery and potential benefit from OPCAB in reducing operative morbidity, current evidence suggest that OPCAB should still be considered a valuable strategy. Undoubtedly, better results using the OPCAB technique are achieved by specialised groups completely committed to this surgical technique. OPCAB is more technically complex and completeness of revascularization is strongly influenced by surgeon and centre volume and expertise.
Acknowledgements
This study was supported by the British Heart Foundation and the NIHR Bristol Cardiovascular Biomedical Research Unit.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Birdi I, Caputo M, Underwood M, et al. The effects of cardiopulmonary bypass temperature on inflammatory response following cardiopulmonary bypass. Eur J Cardiothorac Surg 1999;16:540-5. [Crossref] [PubMed]
- Lemma MG, Coscioni E, Tritto FP, et al. On-pump versus off-pump coronary artery bypass surgery in high-risk patients: operative results of a prospective randomized trial (on-off study). J Thorac Cardiovasc Surg 2012;143:625-31. [Crossref] [PubMed]
- Puskas JD, Williams WH, O'Donnell R, et al. Off-pump and on-pump coronary artery bypass grafting are associated with similar graft patency, myocardial ischemia, and freedom from reintervention: long-term follow-up of a randomized trial. Ann Thorac Surg 2011;91:1836-42; discussion 1842-3.
- Møller CH, Penninga L, Wetterslev J, et al. Clinical outcomes in randomized trials of off- vs. on-pump coronary artery bypass surgery: systematic review with meta-analyses and trial sequential analyses. Eur Heart J 2008;29:2601-16. [Crossref] [PubMed]
- Al-Ruzzeh S, George S, Bustami M, et al. Effect of off-pump coronary artery bypass surgery on clinical, angiographic, neurocognitive, and quality of life outcomes: randomised controlled trial. BMJ 2006;332:1365. [Crossref] [PubMed]
- Cheng DC, Bainbridge D, Martin JE, et al. Does off-pump coronary artery bypass reduce mortality, morbidity, and resource utilization when compared with conventional coronary artery bypass? A meta-analysis of randomized trials. Anesthesiology 2005;102:188-203. [Crossref] [PubMed]
- Reston JT, Tregear SJ, Turkelson CM. Meta-analysis of short-term and mid-term outcomes following off-pump coronary artery bypass grafting. Ann Thorac Surg 2003;76:1510-5. [Crossref] [PubMed]
- Angelini GD, Taylor FC, Reeves BC, et al. Early and midterm outcome after off-pump and on-pump surgery in Beating Heart Against Cardioplegic Arrest Studies (BHACAS 1 and 2): a pooled analysis of two randomised controlled trials. Lancet 2002;359:1194-9. [Crossref] [PubMed]
- Kowalewski M, Pawliszak W, Malvindi PG, et al. Off-pump coronary artery bypass grafting improves short-term outcomes in high-risk patients compared with on-pump coronary artery bypass grafting: Meta-analysis. J Thorac Cardiovasc Surg 2016;151:60-77.e1-58.
- Ascione R, Reeves BC, Taylor FC, et al. Beating heart against cardioplegic arrest studies (BHACAS 1 and 2): quality of life at mid-term follow-up in two randomised controlled trials. Eur Heart J 2004;25:765-70. [Crossref] [PubMed]
- Di Mauro M, Gagliardi M, Iacò AL, et al. Does off-pump coronary surgery reduce postoperative acute renal failure? The importance of preoperative renal function. Ann Thorac Surg 2007;84:1496-502. [Crossref] [PubMed]
- Kuss O, von Salviati B, Börgermann J. Off-pump versus on-pump coronary artery bypass grafting: a systematic review and meta-analysis of propensity score analyses. J Thorac Cardiovasc Surg 2010;140:829-35, 835.e1-13.
- Afilalo J, Rasti M, Ohayon SM, et al. Off-pump vs. on-pump coronary artery bypass surgery: an updated meta-analysis and meta-regression of randomized trials. Eur Heart J 2012;33:1257-67. [Crossref] [PubMed]
- Sedrakyan A, Wu AW, Parashar A, et al. Off-pump surgery is associated with reduced occurrence of stroke and other morbidity as compared with traditional coronary artery bypass grafting: a meta-analysis of systematically reviewed trials. Stroke 2006;37:2759-69. [Crossref] [PubMed]
- Takagi H, Matsui M, Umemoto T. Off-pump coronary artery bypass may increase late mortality: a meta-analysis of randomized trials. Ann Thorac Surg 2010;89:1881-8. [Crossref] [PubMed]
- Bakaeen FG, Chu D, Kelly RF, et al. Performing coronary artery bypass grafting off-pump may compromise long-term survival in a veteran population. Ann Thorac Surg 2013;95:1952-8; discussion 1959-60.
- Filardo G, Grayburn PA, Hamilton C, et al. Comparing long-term survival between patients undergoing off-pump and on-pump coronary artery bypass graft operations. Ann Thorac Surg 2011;92:571-7; discussion 577-8. [Crossref] [PubMed]
- Deppe AC, Arbash W, Kuhn EW, et al. Current evidence of coronary artery bypass grafting off-pump versus on-pump: a systematic review with meta-analysis of over 16,900 patients investigated in randomized controlled trials†. Eur J Cardiothorac Surg 2016;49:1031-41; discussion 1041. [Crossref] [PubMed]
- Robertson MW, Buth KJ, Stewart KM, et al. Complete revascularization is compromised in off-pump coronary artery bypass grafting. J Thorac Cardiovasc Surg 2013;145:992-8. [Crossref] [PubMed]
- Khan NE, De Souza A, Mister R, et al. A randomized comparison of off-pump and on-pump multivessel coronary-artery bypass surgery. N Engl J Med 2004;350:21-8. [Crossref] [PubMed]
- Angelini GD, Culliford L, Smith DK, et al. Effects of on- and off-pump coronary artery surgery on graft patency, survival, and health-related quality of life: long-term follow-up of 2 randomized controlled trials. J Thorac Cardiovasc Surg 2009;137:295-303. [Crossref] [PubMed]
- Murphy GJ, Rogers CA, Caputo M, et al. Acquiring proficiency in off-pump surgery: traversing the learning curve, reproducibility, and quality control. Ann Thorac Surg 2005;80:1965-70. [Crossref] [PubMed]
- Brown PP, Mack MJ, Simon AW, et al. Comparing clinical outcomes in high-volume and low-volume off-pump coronary bypass operation programs. Ann Thorac Surg 2001;72:S1009-15. [Crossref] [PubMed]
- Benedetto U, Caputo M, Vohra H, et al. Off-pump versus on-pump coronary artery bypass surgery in patients with actively treated diabetes and multivessel coronary disease. J Thorac Cardiovasc Surg 2016;152:1321-1330.e12. [Crossref] [PubMed]
- Raja SG, Husain M, Popescu FL, et al. Does off-pump coronary artery bypass grafting negatively impact long-term survival and freedom from reintervention? Biomed Res Int 2013;2013:602871.
- Kirmani BH, Brazier A, Sriskandarajah S, et al. Long-Term Survival After Off-Pump Coronary Artery Bypass Grafting. Ann Thorac Surg 2016;102:22-7. [Crossref] [PubMed]
- Hueb W, Lopes NH, Pereira AC, et al. Five-year follow-up of a randomized comparison between off-pump and on-pump stable multivessel coronary artery bypass grafting. The MASS III Trial. Circulation 2010;122:S48-52. [Crossref] [PubMed]
- Shroyer AL, Grover FL, Hattler B, et al. On-pump versus off-pump coronary-artery bypass surgery. N Engl J Med 2009;361:1827-37. [Crossref] [PubMed]
- Lamy A, Devereaux PJ, Prabhakaran D, et al. Effects of off-pump and on-pump coronary-artery bypass grafting at 1 year. N Engl J Med 2013;368:1179-88. [Crossref] [PubMed]
- Møller CH, Penninga L, Wetterslev J, et al. Off-pump versus on-pump coronary artery bypass grafting for ischaemic heart disease. Cochrane Database Syst Rev 2012.CD007224. [PubMed]
- Chaudhry UA, Rao C, Harling L, et al. Does off-pump coronary artery bypass graft surgery have a beneficial effect on long-term mortality and morbidity compared with on-pump coronary artery bypass graft surgery? Interact Cardiovasc Thorac Surg 2014;19:149-59. [Crossref] [PubMed]
- Synnergren MJ, Ekroth R, Odén A, et al. Incomplete revascularization reduces survival benefit of coronary artery bypass grafting: role of off-pump surgery. J Thorac Cardiovasc Surg 2008;136:29-36. [Crossref] [PubMed]
- Yi G, Youn YN, Joo HC, et al. Association of incomplete revascularization with long-term survival after off-pump coronary artery bypass grafting. J Surg Res 2013;185:166-73. [Crossref] [PubMed]
- Raja SG, Benedetto U. Off-pump coronary artery bypass grafting: Misperceptions and misconceptions. World J Methodol 2014;4:6-10. [Crossref] [PubMed]
- Cooley DA. Con: beating-heart surgery for coronary revascularization: is it the most important development since the introduction of the heart-lung machine? Ann Thorac Surg 2000;70:1779-81. [Crossref] [PubMed]
- Raja SG, Sarang Z. Endoscopic vein harvesting: technique, outcomes, concerns & controversies. J Thorac Dis 2013;5 Suppl 6:S630-7. [PubMed]


