Effects of early administration of acetazolamide on the duration of mechanical ventilation in patients with chronic obstructive pulmonary disease: still far from the truth?
In this study, Rialp Cervera et al. (1) have randomly assigned patients with chronic obstructive pulmonary disease (COPD) or obesity hypoventilation syndrome (OHS) with acute respiratory failure requiring mechanical ventilation (MV) <72 h to receive either acetazolamide 500 mg or placebo. All patients had initial bicarbonate >28 mmol/L and pH >7.35. Test-treatment, ACTZ 500 mg or placebo, was daily administered if pH >7.35 and bicarbonate >26 mmol/L. Clinical, respiratory and laboratory parameters were recorded on a daily basis.
This was a multicenter, randomized, placebo-controlled, phase III, double-blind study held in seven intensive care units in Spain. Patients with COPD or OHS, requiring invasive MV due to acute respiratory failure for less than 72 h and who showed metabolic alkalosis with pH >7.35 and with plasmatic bicarbonate >28 mmol/L, while being on invasive MV, were consecutively included from November 2011 to February 2014. Forty seven patients (36 men) were randomized as ACTZ (+) or placebo: 23 patients in placebo group, and 24 in ACTZ (+) group. There were no significant differences between groups in comorbidities, baseline characteristics or arterial blood gases at inclusion. At inclusion, SOFA score, proportion of patients with non-invasive ventilation (NIV) failure before inclusion, reason of invasive MV, laboratory serum tests, blood gas analysis and respiratory parameters did not show any significant differences between groups.
This study (1) showed no significant decreases in the duration of MV and weaning, or in the length of ICU and hospital stay with acetazolamide treatment compared with placebo in intubated patients with COPD or OHS and metabolic alkalosis. Moreover, patients treated with acetazolamide showed a significant reduction in bicarbonate concentration and PaCO2 values at discontinuation of MV, with 33% of them having recovered from their metabolic alkalosis, whereas no patient in the placebo group did so. Moreover, respiratory rate and minute volume did not show any significant differences throughout the MV period although minute volume tended to increase over time in the acetazolamide group [minute volume 9.7 (8.9–10.4) vs. 10.6 (9.2–12.0) L/min, P=0.26].
In conclusion, this study showed that in severe exacerbation of COPD or OHS requiring intensive care admission and invasive MV, despite the fact that acetazolamide is used to reverse metabolic alkalosis, this therapy does not help reduce the duration of MV and/or make the weaning process easier.
Nevertheless, this study—as mentioned by authors—suffers from many limitations. First, a sample size of 98 patients was estimated to have a power of 80% with an alpha error of 5% to detect a 3-day difference between groups in the duration of MV. However, the study was stopped prematurely due to slow patient recruitment. In fact, only 47 patients were included in the study, 23 patients in the placebo group and 24 in the acetazolamide one. Consequently, this study did not detect any significant statistical differences in the duration of MV because of a possible lack of power. The second limitation mentioned was the lack of measurement of a central drive performance due to the multicentre character of the study and the different equipment within hospitals. Another limitation which must be mentioned is the heterogeneity of the included population (with COPD and OHS).
In addition to these study limitations, we think that the inefficacy of ACTZ can be due to other factors. In fact, this inefficacy may be related to pharmacokinetic reasons. In fact, there are several isoforms of human carbonic anhydrase, therefore, some patients may be more inhibited than others by ACET, which may complicate the reversal of metabolic alkalosis (2-4). Moreover, several factors, such as co-administration of furosemide or systemic steroid, can interfere with ACET pharmacokinetics (5). In the study performed by Rialp Cervera et al. (1), co-treatments with diuretics (69% vs. 71%), steroids (4% vs. 13%), catecholamines (35% vs. 50%), were not used in the same proportion in the two groups (although the difference has no statistical significance), theses therapeutics can interfere with ACET pharmacokinetics and affect ACET’s effectiveness (5).
Moreover, the optimal dosage of acetazolamide to be administered to alkalotic COPD patients is unclear. The results of a study recently published (6) suggest that higher doses of acetazolamide (>1,000 mg daily) are necessary to induce a substantial increase in minute ventilation. This effect is obtained at the price of an increase in respiratory rate rather than tidal volume, whatsoever the ventilatory mode (6). Finally, it is necessary to precise that ACET induces a metabolic acidosis which stimulates the respiratory neural-driving leading to a hyperventilation with polypnea. This polypnea will significantly increase the workload of respiratory muscles in patients having poor mechanic capacities (in severely flow-limited COPD patients). As a consequence, a respiratory muscle dysfunction, which is frequently observed in COPD patients, will be increased by ACET prescription.
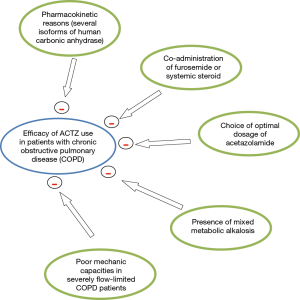
In summary, we found that this recent study (1), confirms the results of two retrospective, case-control studies (3,7) and one randomized clinical trial (8) published on the same subject. The conclusions of all these studies (1,3,7,8) were in severe exacerbation of COPD requiring intensive care admission and invasive MV, metabolic alkalosis occurs frequently in this group of patients who frequently receive therapies for cardiac and respiratory failures (steroids, diuretics, etc.). Moreover, these studies suggest that systemic ACET therapy in this specific condition is not helpful to reduce the duration of MV and to make the weaning process easier. As shown in Figure 1, due to multiple pharmacokinetic reasons and several factors—such as the co-administration of furosemide or systemic steroid that can interfere with ACET therapy, the high dose requested of ACET, and the significant increase of the workload of respiratory muscles—this therapy (ACET) seems to be ineffective to significantly decrease the duration of MV and weaning, or the length of ICU and hospital stay in patients COPD exacerbation requiring invasive MV.
In conclusion, there is limited evidence to recommend use of systemic ACET therapy in severe exacerbation of COPD requiring intensive care admission and invasive MV, to reduce the duration of mechanical. As consequence, ACET therapy in this specific condition is not helpful to reduce the duration of MV and to make the weaning process easier.
Acknowledgements
All authors thank Professor Chokri Khalaf for his help in the redaction of this manuscript.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Rialp Cervera G, Raurich Puigdevall JM, Morán Chorro I, et al. Effects of early administration of acetazolamide on the duration of mechanical ventilation in patients with chronic obstructive pulmonary disease or obesity-hypoventilation syndrome with metabolic alkalosis. A randomized trial. Pulm Pharmacol Ther 2017. [Epub ahead of print]. [Crossref] [PubMed]
- Alp C, Özsoy Ş, Alp NA, et al. Sulfapyridine-like benzenesulfonamide derivatives as inhibitors of carbonic anhydrase isoenzymes I, II and VI. J Enzyme Inhib Med Chem 2012;27:818-24. [Crossref] [PubMed]
- Bahloul M, Chaari A, Tounsi A, et al. Impact of acetazolamide use in severe exacerbation of chronic obstructive pulmonary disease requiring invasive mechanical ventilation. Int J Crit Illn Inj Sci 2015;5:3-8. [Crossref] [PubMed]
- Bahloul M, Chtara K, Chelly H, et al. Acetazolamide use in severe COPD exacerbations requiring invasive mechanical ventilation: impact on duration of mechanical ventilation. J Thorac Dis 2016;8:762-4. [Crossref] [PubMed]
- Heming N, Faisy C, Urien S. Population pharmacodynamic model of bicarbonate response to acetazolamide in mechanically ventilated chronic obstructive pulmonary disease patients. Crit Care 2011;15:R213. [Crossref] [PubMed]
- Heming N, Urien S, Fulda V, et al. Population pharmacodynamic modeling and simulation of the respiratory effect of acetazolamide in decompensated COPD patients. PLoS One 2014;9:e86313. [Crossref] [PubMed]
- Faisy C, Mokline A, Sanchez O, et al. Effectiveness of acetazolamide for reversal of metabolic alkalosis in weaning COPD patients from mechanical ventilation. Intensive Care Med 2010;36:859-63. [Crossref] [PubMed]
- Faisy C, Meziani F, Planquette B, et al. Effect of Acetazolamide vs Placebo on Duration of Invasive Mechanical Ventilation Among Patients With Chronic Obstructive Pulmonary Disease: A Randomized Clinical Trial. JAMA 2016;315:480-8. [Crossref] [PubMed]


