Prof. Yi Hu: a doctor of acute insight and action
Introduction
The ancient Greek aphorism “know thyself” engraved on the forecourt of the Temple of Apollo epitomizes the human desire for the exploration into the unknown. In fact, never has mankind dragged their feet in understanding themselves, as in the achievements scientists have made all these years in the studies of disease and pathology.
Ere the 2017 WCLC journey, AME Editors were sent across China to conduct in-depth interviews with an army of distinguished experts in the field of lung cancer. Together we learned how these soldiers fought for the nation that has the largest number of patients, and how they dedicated their lives to inventing the most-advanced weapons and probing into the enemy camp. From the past, they reflect and learn from mistakes; at present, they work hard and make changes; for the future, they make plans and improvements.
May this issue take you to the innermost world of these Chinese scholars, where you can delve into their wealth of knowledge and be inspired.
Prologue
Several months ago, Prof. Yi Hu and his team were working on a clinical research project to find the best strategy to postpone the drug resistance in the targeted therapy for lung cancer. The team has designed several clinical trials and developed a new medicine that could reverse the drug resistance at the early stage of study. Prof. Hu said: “There is no need to design more trials, because we have a preferential medicine. We don’t need multidrug therapy anymore!”
Later, Prof. Hu replace ARMS test which was designed at the early stage of trial with the newest technique, next generation sequencing (NGS). “With the progress of detection technology, we have to speed up our research” he said, “after the invention of the intelligent robot Watson, tons of data can be processed by the robot, and the human brain will be good at a flash of insight or genius. To do a good research, we need to be forward-looking and adaptive.” It is not worthy if you need to spend too much time on the research.
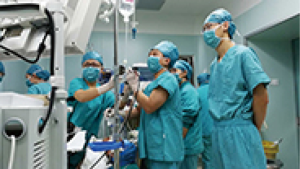
This is Prof. Yi Hu (Figure 1), the Director of the first Oncology Division at the Chinese PLA General Hospital.
Solid foundation and creative thinking
When Prof. Hu studied his PhD under the direction of his tutor Prof. Shu-Jun Cheng, the only treatment for tumors was chemotherapy. There were no such detailed and clear pathological classifications of lung cancer as they are now and there was no individualized treatment focused on a specific target. When designing the study protocols, he found that based on the current clinical data, they can not figure out whether the chemotherapy works for a specific kind of patients. So, we were not sure how to choose the patients in clinical research or what kinds of patients will develop chemoresistance?
To figure out the intrinsic problem in chemoresistance, Prof. Hu came out an idea of analyzing the status of DNA. At that time, DNA sequencing technology wasn’t as advanced as it is now. The chromosome was observed under the microscope, and the software for alignment of DNA sequences was very simple and stupid. “I stared at the chromosome pictures every day and night. At first, I couldn’t tell the differences among chromosomes, they were all fragments to me. After one or two mouths, I had a sudden insight that helped me to distinguish which individual chromosomes they are”, Prof. Hu said. It demands excellent squash techniques, great experiences of chromosome karyotype analysis and lots of patience to identify the individual chromosome under high-power microscopes with biological micro movie-making technology.
Prof. Yi Hu eventually achieved some good results in his researches. He believes the reason why this technique was not available for many researchers is that the researchers were not familiar with chromosomes. While he began his postdoctoral work with Prof. You-Ning Liu, the microRNA high-throughput screening technique has been well developed. He decided to continue his PhD research project on the mechanism of chemoresistance, and successfully got the fund from the National Natural Science Foundation, which was his first funding. “looking back, I found all the work of those years has built a solid foundation for the researchers afterwards.” said Prof. Hu.
During the interview, Prof. Yi Hu mentioned about “inspiration” several times, so we asked him how he could come up with some new ideas. Prof. Hu had been immersing himself in brisk memories, but suddenly became serious and replied “Probably because I am always thinking and pondering”.
In recent years, Prof. Yi Hu has led his team to work on some prospective research and made some achievements. Mentioned about these results, Prof. Hu said, “We could not have achieved these results without the predecessors of Chinese PLA General Hospital who have devoted great efforts to the tumor immunotherapy for a long time.” Shun-Chang Jiao, Director of Department of Oncology has worked on tumor immunotherapy since 2004. When the other hospitals were using the PD-1 monoclonal antibody for only one or two patients, the PLA General Hospital already had over one hundred cases using the drug. Therefore, on the whole, the PLA General Hospital was easier to accept the latest immunotherapy treatments concepts.
In 2016, the latest international research results showed that patients with higher TMB are more likely to benefit from immunotherapy. However, in 2015 Prof. Hu had already proved this correlation on dozens of patients.
Prof. Hu found some literature mentioned that patients with higher TMB are less likely to benefit from drugs targeting a single driver gene and he also noticed that Prof. Yi-Long Wu has mentioned several times in conferences: some tumors are simple and some are complicated. Simple tumors (also called benign tumors) are more likely to be affected by targeted medicines; but for complicated tumors with multiple mutations, it is more difficult to find the real driver genes. And he found lung cancer patients have higher TMB. “With all these thinking and finding, we decided to try immunotherapy on patients with higher TMB, which was used as one of the evidences in making our treatment plans.” Obviously, these patients finally benefited from our practical results of immunotherapy.
“It is necessary to think about the problems to understand and acquire knowledge. Certainly, it is impossible to understand things without thinking.” Prof. Hu said.
Forward-looking and sensitive
It is one of the most important schedules for Prof. Yi Hu to read the latest articles and pay attention to the new techniques despite of busy daily routines. Prof. Hu said, “It is more convenient to acquire information nowadays. As long as you are willing to learn, you can continuously acquire new knowledge. Furthermore, some researches will cause a chain reaction, which means once a new finding comes out, there will be a series of related research articles published. All you need to do is to read these articles, and it will inspire your thinking.”
As for the basic and clinical research on tumor immunotherapy, Prof. Hu led his team and followed the published literature at the beginning of their research. Right now, they have the ability to design innovative trials and conduct the research on their own, and as a result, contribute to scientific development. One of the current research projects in his team is the predictor for the effectiveness of immune targeted drug, in other words, the relationship between the detection of screened cytokines on the T-cell surface and the clinical effectiveness of the therapy, which is a groundbreaking research around the world.
Prof. Hu’s team will work on the basic research related to clinical practice, the translational research to quickly transfer the research results into clinical application and benefit the patients. Even, some conclusions from early stage researches can be applied to clinical medicine now, providing guidelines to avoid risk in time and solve patients’ problems.
“Everyone is very busy in their clinical work but still working on the researches to solve practical problems and benefit patients. It not just about finishing their papers.” Prof. Hu said. “It is to provide patients with better treatments, and also test the effectiveness of therapy strategies. Furthermore, it will not only build up the confidence in treating next patient, but make the next following research deeper and more thorough.”
“How can you treat the disease without following the latest research literature and evidence?” Prof. Hu believes that as the doctors from national research hospitals, they should bear in mind the idea to provide every patient the best treatment and apply the latest methods and concepts to clinical practice.
In 2007, anti-tumor angiogenesis medicine was used for the first time in China. At that time, a patient with early stage stomach cancer at the Chinese PLA General Hospital received postoperative adjuvant therapy. The patient was financially well-off and asked to try the latest anti-tumor angiogenesis medicine. The medicine was used for two circles. The patient suffered from hemoptysis and soon got worse with gastrointestinal bleeding after two days he left the hospital. Finally, he died of the disease. There was no such a case of fatality related to that medicine at that time in China. Prof. Hu’s first thought was, “It must be related to that medicine which would influence the vascular endothelium.” During the interview, Prof. Hu told us he was more sensitive towards this medicine, after all he had made deep research on the medicine when he first came across this medicine.
At that time, Prof. Hu had done some systematic researches on new medicine and read the latest articles, from the medicine mechanism, drug metabolism to the possible adverse effects. How exactly does medicine benefit patients? What are the potentials of the medicine? He did thorough research on the mechanisms of medicine effectiveness, not just reading the medicine’s instructions. Prof. Hu believes, “It is important for doctors to have scientific thinking and systematic training. They need to have the habits of tracking down the sources of the problem and exploring for the answer. Try your best to think deeper within your understanding.”
In fact, combined drugs are usually applied in in the clinical treatments of tumors. Using the “combination blow (therapy)” can extend the timeline of drug resistance and enhance the effectiveness of treatment. “We don’t use single therapy in current tumor treatments. It is not enough and feasible to only provide the patients with only one chemotherapy or targeted drugs”, Prof. Hu said.
So, what is the mechanism behind the “combination blow (therapy)” to improve the effectiveness of treatment?
In clinical lung cancer treatments, it is often to use combined therapy of targeted drug and the PD-1 or the CTLA-4 monoclonal antibody and the PD-1 monoclonal antibody. To fully realize the targeting effects in the treatment and explain the intrinsic reason of the increasing effectiveness of “combination blow(therapy)”, Prof. Yi Hu and his team are now working on designing new types of antibody combinations, and increasing the identifiability of immunocyte—adding the EGFR antibody to the PD-1 antibody, which is dual resistance; as well as adding the EGFR and VEGF antibodies to the CTLA-4 and the PD-1 monoclonal antibody, which is quadruple resistance.
The antibody platform was set up by Prof. Yajun Guo in early years, and right now Prof. Hu has developed it into a new type of research platform. Many of his ideas are put into practice on this platform, developing researches on “novel multi-targeted antibodies and their anti-tumor activity”, with high hopes to generate enduring antibodies for tumor treatments in the future.
At the 2017 World Conference on Lung Cancer (WCLC), Prof. Hu and his team will present three posters about lung cancer immunotherapy (Figure 2).
Execution
Within two years from 2015–2017, Prof. Hu has led his team to get the first National Key Clinical Speciality Project of Army Construction, and built up an endoscopic operating room and a tumor intensive care unit. He has also led his team to focus on the technique of endoscopic surgery and related operations; the team have made rapid and astonishing progress under Prof. Hu’s lead.
When Prof. Hu became the Chief of the First Oncology Division at the Chinese PLA General Hospital, he realized that the department had made many achievements and published a series of articles under the leadership of predecessors. But the department of oncology was a new division with a team of young doctors or researchers, it had not yet been included in the National Key Clinical Specialities. The research ability of the team was rapidly increasing. “I think we should have the ability to apply for being a National Key Clinical Speciality. At that time, our division tried our best in the application and we finally made it!” It seemed to be widely recognized, Prof. Hu looked up and said straightforwardly: “We came in first place out of all units, with the efforts of our own division. The units of the second and third place had gathered 10 divisions’ efforts to be included in the specialties. We did feel so proud after finally being one of the key specialties, and we were honored.” Prof. Hu then said.
“Since the division became one of the National Key Clinical Specialities, we have received full support from the nation, which has built up the foundation for the establishment of endoscopic operating room afterwards.”
In Prof. Hu’s opinion, for those patients of lung cancer with tumors in their main airway, if you don’t solve the problem, the patients may die of suffocation soon before they could receive the systemic treatments. Only by helping patients go through the current crises, we then have a chance to design systemic treatments for them. But the traditional ideology is that the lifespans of tumor patients are short and endoscopic treatments are unnecessary. If transferring patients to other hospitals to receive operations, there are too many unpredictable factors during the transfer process for critical patients. The patients may miss the timing to receive the best treatments and lose confidence in the treatments.
“It is not the work style to always ask for other people’s helps in the Chinese PLA General Hospital”, said Prof. Hu. He wanted to set up their own endoscopic operating room; however, nobody supported them in the beginning. Prof. Hu recalled his memory at that time, “Maybe some people won’t understand the differences between tumors and respiratory diseases. The key of management of tumors is to focus on treatments and of respiratory diseases is to focus on diagnosis.”
With the fund of National Key Clinical Speciality project, Prof. Hu led his team to set up the endoscopic operating room (Figure 3). Afterwards, the hospital devoted some funds into this operating room when they saw the effectiveness this operating room had brought.
“We developed rapidly. Now, we can perform all kinds of airway (respiratory tract) surgeries which can save people near death.” Prof. Hu said.
However, after having local treatments like endoscopic surgery, patients would have mucosal edema without the help of a ventilator, which would cause a huge impact on their respiratory functions. If there is no intensive care unit to let critical patients survive through the difficulties, then there is no need for the follow-up systemic treatments. For example, for some lung cancer patients, tumors are stuck in their small airway, so doctors need to open their airway and insert a child-sized trachea to ensure the ventilation; otherwise, patients will suffocate to death. These surgeries need mechanical ventilation, which cannot be performed in normal ward. For these patients, they are possible to receive the follow-up treatment of chemotherapy and get better.
“This is the reason why we set up the Tumor Intensive Care Unit—exactly for the rescue of this kind of patients!” Prof. Hu said with confidence.
“With the care received in the tumor intensive care unit, and followed by nursing and supportive therapy, our patients have the opportunities to receive follow-up systemic treatment. Because the tumor intensive care unit is the first one in China, many people thought we were not serious about it when we just set up.” he laughed. To gain more supports besides national funding, they needed to apply for hospital funds and find sponsors everywhere.
Love beyond borders
The reason why Prof. Hu set up tumor intensive care unit is that he hopes once critical patients make through the difficulties, they can have the opportunity to be benefited from new therapies and treatments.
“Life is a step-by-step process. If you have the chance to receive treatments at the beginning, and extend your lifespan, you will probably have the chance to benefit from the latest therapy and extend your lifespan in the future. Step by step, you might have the opportunity to live longer. However, this kind of opportunity comes from the willingness of patients to receive the treatments; otherwise, they miss the opportunity at the very beginning.” Prof. Hu said. “If oncologists don’t have these ideologies and don’t encourage the patients to receive treatments so that they try the newest therapy, then there will be definitely no further extension of their lifespan.”
Among Prof. Hu’s patients, some of them received chemotherapy in the beginning, and then received the first to third generation targeted therapy when they came out. Their lifespan can be extended for 8 more years. For these kinds of patients, if they gave up chemotherapy at the time, they would lose the chance to survive longer. In the clinical treatment, Prof. Hu not only encourages his patients to receive the treatments but also encourages them to accept the adverse drug reactions resulting from the treatment.
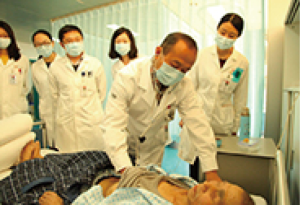
When talking about how Prof. Hu treated his patients, the young doctors in Oncology Division said “Chief Yi Hu treats every patient with patience and gives them detailed explanations. He has very clear thinking and decisive judgment. The treatments he made for his patients are all customized and individualized and with international and advanced perspectives”
In past few decades, as a tumorist, Prof. Hu has witnessed that tumor therapy has kept progressing. “Twenty years ago, the only tumor medicine was chemotherapy. In the hospital corridors, there were scenes showing the painfulness of patients after chemotherapy. We could only apply the available basic treatments for our patients. Ten years ago, the third-generation chemotherapy and medicine that was effective at lowering the adverse drug reaction came out. It led to a huge progress in tumor therapy, and doctors suddenly felt chemotherapy was more acceptable. Since then, we started to tell our patients: without the treatment, you only have one result, but taking the treatment, there might be two possible outcomes.” (Figure 4).
When meeting with patients, Prof. Hu would pay special attention to the patients’ psychological issues. He thinks most of the patients with tumors have some psychological problems, because tumors and long-term depression are related. He suggests, “Patients should know the truth of their disease.” If patients don’t know the truth, they might feel they are “in critical condition” and therefore refuse the treatment. Instead, by telling them their true condition and informing them there is a possibility to be fully cured, they will have a hope. “Cancer isn’t hopeless itself, but if doctors can not guide patients correctly, they might die in a short period of time.”
Like a mentor, like a friend
“Prof. Hu always pays attention to each student’s research progress. He spends a lot of time with students and he will be at the division building almost every weekend. He creates some opportunities for us to broaden our horizon in our expertise, through taking us to participate in academic conferences”, Dr. Fan Zhang the Director of Doctors in the hospital said.
Young doctors from the department always joke about the time working with Prof. Hu, “it reminds us of our junior high school experiences, in a group that is highly committed and with a strict and kind chief.” Young doctor Hai-Tao Tao said, “Prof. Hu is really nice and full of charisma. He enjoys sports activities and organizes ball games to improve our physical fitness and group cohesion. We always talk about the difficulties we face in life with him and listen to his advice.”
Prof. Hu said with a sigh, “When I was just a young doctor, I learned a lot from my teachers about how to be a good doctor and researcher. I can not make all the improvements and achievements in life and work without my teachers’ cultivation.” In his forties, he said: “We were all young before, and now as senior doctors, we hope we can do better, letting more young doctors to stand out. We now have stricter standards toward our young doctors, and I know the most desirable thing for these young doctors is to get better development of their expertise and career. I hope I can build a better and fair platform for them, so they can have a better environment to grow and develop.”
Prof. Hu emphasises on developing young doctors’ willingness to pursue knowledge. Meanwhile, he believes that a functioning operation and management system can magnify the role of people and make the training process more standardized, which is very critical to managing and training young doctors.
“It is a very tough training process to study medicine. Now it is not easy for the young man to finish their study and develop their career, so we call for a better environment for them on a national level,” he said. “The progress of medicine can benefit our society, and the trained and talented medicine practitioners can contribute to the society. I believe we should have this kind of mindset.” (Figure 5).
In the end of our interview, we ask Prof. Hu how did he make a balance between all his responsibilities. “Oh, right! Actually, I don’t know the answer too. Maybe it is because I am willing to do all these things and have a healthy body.”
“His nickname is superman.” the young doctor said. Prof. Hu will do some exercise when he has some free time in his office. “It’s really tired as the Chief of a big division, you have heavy workloads, including teaching, doing research and even nursing. But I’m happy.” he said.
Conversation with Prof. Yi Hu
AME: What were the precision lung cancer treatments before “Precision Medicine”? What about the latest treatments? What are the current difficulties of this therapy?
Prof. Hu: The current lung cancer treatments have been able to determine different therapies for patients according to the phenotype and molecular typing. The detection scope includes detecting the types of genes and performing tests on the whole exon. Besides of deciding on the targeted drug depending on gene mutations, we can consider choosing immunotherapy with TMB testing.
Using the drug resistance management of EGFR-TKI drugs for non-small cell lung cancer as an example, in the past, we conduct precision medicine treatment according to clinical phenomenon. Based on local symptoms, we classified the disease progress into local progress, slow progress and overall progress. For local progress, we continue using EFGR-TKI combined with local treatments, like chemotherapy and surgery; for slow progress, we observed the symptoms and the drug resistance conditions first, and then changed the treatment strategies; for overall progress, it may involve medication adjustment depending on the cases. At that time, this was a consensus but the fact was that precision medicine was about to come out at that time.
Today, based on the current conditions of precision medical technique, it is still difficult to apply precision medicine on every patient. The main reason is that: the second biopsy or multiple biopsies are traumatic and are not acceptable in all circumstances; it was also a challenge on skills of the doctors. The specimens of liquid biopsy and tissue biopsy are not 100 percent matched; In China, the precision testing is not standardized yet and the repeatability is relatively low, so it is a challenge on the ability of technicians and doctors to analyze the data.
But as time progresses, the developments are continuous. The techniques definitely become better and better year-by-year. Like the ultrasonic-guided puncture technique, CT-guided biopsy technique and endoscopic biopsy technique, these are the all advanced supplementary methods.
AME: What is the future direction of lung cancer precision medicine?
Prof. Hu: Now precision medicine has developed beyond the original scope mentioned previously, and is in the direction of high-precision on fighting tumors—high effectiveness rate, while protecting the normal tissues from attacks. All types of treatments are based on this concept. There are high hopes that the medicine only works on tumor cell, and reduces the potential influence or harm on normal cells. We also hope the reaction on tumor cells can be precise to the cell signal pathways, finding the exact molecular part that causes the continuous deterioration of tumor cells.
Precision medicine is well applied in lung cancer. The most successfully research was the development of EGFR-TKI and ALK inhibitors. The first, second and third generation of EGFR-TKI are available, and the fourth and fifth-generation of EGFR-TKI are in the rapid process of research development. AZD9291 clearly works better than the first and second generation of EGFR-TKI, it solves more problems and extends the patients’ survival. We have the talents in every generation (the new is always replacing the old), and new medicine can provide more benefits to patients. This is the point of development and new medicine can only be used in the second line of treatment. In the future, it should be used in the first line of treatment. These new medicines will be taking a significant place in the future.
AME: Biomarkers are the bottleneck of tumor immunotherapy, so what is the future direction of these kinds of research?
Prof. Hu: Given the current techniques, immunotherapy has been able to achieve crushing control the tumor cells on the selected patients. But how to find the real immune target? We still haven’t found the answers yet.
PD-L1 can be an immune biomarker but it cannot cover all immunotherapy. TMB is a potential biomarker but patients with higher TMB do not necessarily benefit from immunotherapy, it is a probability event. Based on current knowledge, the only way to enhance the precision of immunotherapy is to find the real antigen—the new antigens that can stimulate the immune system. Of course, new antigen will be updated in the future development.
Currently, patients with higher TMB will have a higher possibility of generating new antigens, but it’s still a probability event. The biomarker of immunotherapy is like the polices and tumors are like the thieves. “Experienced polices” have a better ability in detection, so they are less possible to miss “thieves”. In a criminal environment, one experienced police can catch all the thieves. If new antigens appear and can be the biomarkers, then the corresponding immunotherapy could hit the tumors accurately.
AME: You have accumulated over 500 immunotherapy cases, what does this mean for clinical research? In the future, what are you going to do with these cases?
Prof. Hu: All the immunotherapy cases are very precious to us. We have had over 500 cases. This kind of achievement is very rare for a single medical center. In the US, a lot of patients participate in clinical trials, but it is almost impossible for a single medical center to have so many cases.
We conduct the relevant tests on these five hundred patients, and make sure we follow each case to track the immune system behavior. It is difficult to predict who will benefit from the immunotherapy and who will suffer from adverse reaction. Right now, the numbers of targets are not enough.
Especially, the most pressing issue we need to work on right now is how can we predict and prepare for the patients who might have the severe immunotoxicity response? In the clinical research, for those patients who have immunotoxicity, immunotherapy is also effective. But the patients might be dead before the tumor is shrunk; this is very dangerous. Therefore, the key is how to control—to save patients live with better quality of life and avoid the risks of immunotherapy in the meantime.
Some people think we are cutting corners, but that is not true. The main reason is that when the new medicine came out, we happened to have abundant case data to conduct the research and reach some conclusions. With regard to medical case resources, Chinese doctors have exceptional advantages.
AME: How do we fully utilize China’s advantages of a large number of cases?
Prof. Hu: Though we have rich medical case resources, we don’t have a well-developed database, all the records are not stored or transformed into data, which is related to our national development and the patients’ awareness.
Each hospital has its own database, but we haven’t formed a nationwide database. Many patients in China don’t realize that it is very important for medical development to help accumulate and complete the medical data. In other countries, patients think the cooperating with doctors’ following-up and collecting data is a service to the public, they think it can benefit more people. At Mayo Clinic in US, 92% of the gynecology cases are included in the clinical research in the department of gynaecology; and this number can also reach 87% in other divisions. Our levels are far behind compared to foreign countries in this aspect (Figure 6).
Acknowledgements
Special thanks to: Prof. Su-Jie Zhang, Prof. Hai-Tao Tao and Prof. Fan Zhang from the Department of Oncology at the Chinese PLA General Hospital provided supports for this interview. The authors also would like to thank Yuan Yu and Haichen Yang from AME Publishing Company for assisting in the interview.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
(Editors: Renfang Wang, Tanlun Yu, AME Publishing Company,