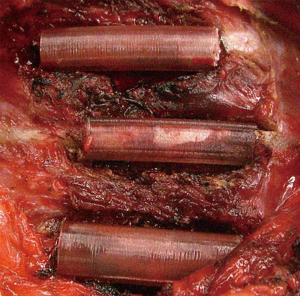
Development of a socket-type rib coaptation device made of poly-L-lactide fibers: feasibility study in a canine model
Introduction
Surgical stabilization of fractured ribs in cases of uncontrolled pain or respiratory failure has been studied and accepted as an effective therapy, which results in shorter mechanical ventilation periods, lower medical costs, and quicker resumption of work (1-3). Recent reports on the treatment of flail chest recommend surgical fixation of fractured ribs (4-8). Surgical costal fixation is performed either with external fixation (outer cortical placement of plates) or with intramedullary stabilization. MatrixRib (DePuy Synthes, West Chester, PA, USA), RibLoc (Acute Innovations, Hillsboro, OR, USA), and Stratos [Strasbourg Thoracic Osteosyntheses System (STRATOS™); MedXpert GmbH, Heitersheim, Germany] are commercially available examples of external stabilization system (9-11). Other reports are in favor of the plate system rib stabilization (12,13). Intramedullar fixation is performed by inserting costal pins or rods. Poly-L-lactide (PLA) bone coaptation pins or rods have been reported to be effective for the treatment of fractured bones (14-16). Their usefulness is also appreciated in rib fixation in general thoracic surgery (17-20). However, not all reports are in favor of their clinical results of rib fixation, as reflected by two conflicting reports (19,21). Our clinical experience with costal sockets since 2000 at Kyoto University Hospital includes implantation of approximately 120 sockets in thoracotomy cases. Our criterion regarding rib fixation failure is complete radiographical displacement of the costal pin-inserted ribs. The failure rate is approximately 30%. This is considered to be clinically unfavorable.
When inventing a surgical stabilizing device for bone fractures, less invasive materials should be used for bone fixation (22-24). A feature of less invasive materials is biodegradability, seen with PLA.
To develop a more reliable rib coaptation device with innovative structure for external fixation, we developed costal coaptation sockets made of PLA fibers. We investigated the mechanical properties of the newly developed costal sockets and their effectiveness in costal fixation in adult beagle dogs.
Methods
Three-dimensional (3D)-printed socket preparation
A commercially available 3D printing machine (Bits from Bytes 3D Touch Printer, 3D Systems, SC, USA) was used in this study. Using thermoplastic PLA material, the 3D printer heats the material through the extruder (printer head). The extruder then pushes out a very fine plastic thread, which is arranged layer-by-layer according to the x- and y-coordinates, resulting in a solid 3D object. The maximum print speed in terms of extruded volume is 15 mm3 per second. Print tolerance is the possible deviation from the provided x- and y-coordinates, which was specified as ±1%, and on the z-axis, it was specified as ± half the processed z resolution for this printer. In the present study, the model used was the 3D TouchTM 3D printer (double head) to print the sockets (Figure 1A).

PLA fiber knitted socket preparation
Our newly proposed rib coaptation sockets (Marui Textile Machinery Co., Ltd., Osaka, Japan) were fabricated using PLA fiber knitting and heat processing. Two kinds of PLA fibers with melting points of 170 and 210 °C were separately knitted to form a hollow curved socket of 4-cm length, with a curvature radius of 12 cm; then, they were heat processed at 180 °C for 20 to 60 min (Figure 1B). Each PLA fiber, with a melting point of 170 °C, is composed of 36 filaments, with a weight of 110 g per 10,000 m (110T36f). Each fiber with a melting point of 210 °C is composed of 48 filaments, with a weight of 167 g per 10,000 m (167T48f). The letter “T” indicates the unit “decitex” for fibers. The most commonly used unit for linear mass density of fibers is the decitex, which is the mass in grams per 10,000 meters. The letter “f” indicates the number of filaments. The ratio of the above-mentioned PLA fibers and the heat processing time were optimized, resulting in successful development of PLA fiber knitted sockets with three levels of incremental elasticity and strength.
Testing configuration for mechanical properties of PLA fiber sockets
To compare the mechanical strength of each type of socket, including the 3D-printed ones, we used a three-point bending apparatus, as was done for mechanical testing of the ribs by Kemper et al. and Stitzel et al. (25,26), attached to a handy force gauge (Digital Force Gage, Model RZ Series; Aikoh Engineering Co., Ltd., Osaka, Japan). The setup of the apparatus was designed so that one end of the socket was held tightly and the other end was supported. Sockets were oriented so that they were bent out to inside, exterior to interior, by an impactor blade. Impactor displacement was applied at a rate of 20 mm/s downward until it lost its curvature radius, and then upward until its original curvature radius was restored (Figures 2,3). The loading (downward direction of the impactor blade) and unloading data (upward direction) were recorded and plotted continuously from the available data by a computer connected to the three-point bending apparatus. The internal sampling time of measured values was set to 50 ms. The unit of each measurement of mechanical strength was expressed kilogram-force (Kgf). The maximum load values were measured as mechanical strength during the test.


This apparatus enabled us to quantify the ductility by measuring the force at which the sockets lost their curvature and the stiffness by measuring the point of failure. For each type of socket, mechanical testing was performed twice. The mean difference between two sets of observations was not significant (paired sample t-test; P=0.68). Therefore, the first value of each mechanical test was considered the mechanical strength of the respective socket.
Operative procedure
Care, housing, and surgeries were performed with the approval of the Committee for Animal Research of Kyoto University, Japan, which ensures humane treatment of laboratory animal subjects in compliance with the guidelines established by the Ministry of Education, Culture, Sports, Science and Technology, Japan. The canine model was chosen for testing this device as our institution has a well-organized canine experimental facility. A total of 15 adult beagle dogs (age <2 years; body weight 8.0–11.0 kg) were used. Each dog was sedated with an intramuscular injection of 0.05 mg/kg atropine sulfate, followed by 15 mg/kg ketamine hydrochloride and 3 mg/kg xylazine hydrochloride. Each dog was then intubated with 8.0–8.5 I.D. endotracheal tube. Respiration was maintained by a mechanical ventilator with sevoflurane and oxygen. Monitoring of electrocardiogram and percutaneous oxygen saturation was conducted throughout the surgical procedures. To reduce the risk of postoperative infections, each dog was administered an antibiotic (ampicillin sodium) immediately after intubation.
Each dog was placed on the left lateral decubitus position. The skin was shaved and sterilized with an iodine solution. The lateral side of the right chest wall was exposed to visualize the 7th to 9th ribs. After the ribs that were planned to be divided were exposed, the superior and inferior aspects of the ribs were dissected with electrocautery and freed from the intercostal muscles. Care was taken not to injure the intercostal pedicles. Lateral-midlines of the three ribs were divided with a rib cutter. The sockets were sterilized with gaseous ethylene oxide before implantation. Subsequently, the rib sockets were implanted to stabilize the divided ribs (Figure 4). A steel wire was placed at both ends of the sockets as a marker because the sockets are radiolucent. 3D-printed sockets were implanted in 15 ribs of five dogs to stabilize the divided ribs, and PLA fiber knitted sockets (four dogs for type A, three dogs for types B and C each) in 30 ribs of 10 dogs (Figure 5).

We observed the degree of fixation of the divided ribs with computed tomography (30) scan and its 3D reconstruction using the Open Source OsiriX software (OsiriX®) immediately after the operation and after 1, 2, 3, and 6 months. We employed the rib displacement categorization described by Kawachi and colleagues; it includes no displacement, lateral, vertical, and combined lateral with vertical displacements (21).
Measured and calculated data (mechanical strength of sockets and scale of ribs) are expressed as mean (SD). Mann-Whitney U test was used to compare the difference of the costal size and mechanical strength of the PLA fiber sockets. A P value of <0.05 (two-tailed) was considered significant. Statistical analysis was performed with StatMate IV (ATMS Co., Ltd., Tokyo, Japan).
Result
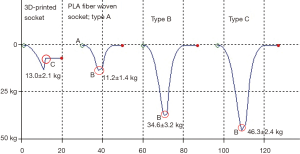
The ratios of PLA fibers, heat-processing time, and mechanical properties of the sockets, including the 3D-printed sockets, are shown in Table 1 and Figure 6. The 3D-printed sockets had less durability with poor elasticity, showing failure at a force of 13.0±2.1 kg. Not all the 3D-printed sockets could restore to their original curvature radii. Three types of PLA fiber knitted sockets with incremental mechanical strengths were successfully manufactured by adjusting the ratios of low-melting PLA fibers to high-melting ones with different heat processing time. The amount of low-melting PLA fiber and the length of heat-processing time were positively correlated with the rigidity of the sockets.

Full table
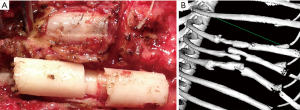
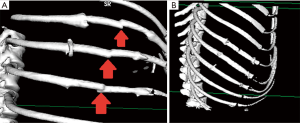
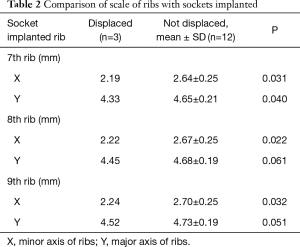
All 3D-printed sockets (15 sockets in 5 beagles) failed 1 month after the implantation, exhibiting combined lateral and vertical displacement of the divided ribs (Figure 7A,B). Further follow-up was not performed because they were sacrificed for evaluation. All 10 beagle dogs [type A socket for 4 dogs (12 sockets), types B and C for 3 dogs each (9 sockets for each)] whose ribs were fixed with PLA fiber knitted sockets were examined for 6 months with CT scans. Displacement occurred 1 month after the operation in the three ribs of the dog in which type C costal sockets were implanted. The degree of displacement in those ribs did not change during the further follow-up period (Figure 8A). The remaining 27 implanted sockets in nine dogs stabilized the divided ribs well (Figures 8B,9). The animal in which all ribs displaced radiographically had small physique. Its ribs were significantly small in size (Table 2).

Full table
Discussion
Costal pins made of PLA have been used for rib fixation in thoracic surgery (17-20). However, not all reports are in favor of their effectiveness (21). The incidence of rib displacement following costal approximation with PLA pins ranges from 1.3% to 31% (19-21). Tsunezuka and colleagues suggested that costal pins could be ineffective in cases of brittle bone marrow because costal pins can move within the bone marrow space (20). At Kyoto University Hospital, from 2000 to 2015, 116 costal pins were implanted in lung cancer operations and lung transplant recipients/donors to approximate the ribs divided during posterolateral thoracotomy. The failure rate has been found to be 30%. Considering the nature of thoracotomy, even if without any costal fixation failure, patients were prone to have postoperative pain. However, in most cases, the pain was likely to be controlled gradually. Post-operative patients with costal fixation failure were highly likely to suffer from intractable pain or uncomfortable sensations. Unfortunately, the exact data regarding the relation between post-thoracotomy pain and costal fixation failure could not be retrieved or be cited. Therefore, empirically, it could be hypothesized that fixation failure can intervene in pain control. Considering these drawbacks, invention of a new device for costal fixation is encouraged. The development of our socket system originated from the idea that all circumferential stabilization, which is circumferential external fixation, of fractured points should be superior to internal fixation.
Mechanical strength/elasticity
Several studies have reported the mechanical properties of the ribs. Stitzel et al. reported that the lateral portion of the ribs has more stiffness and ultimate stress than the anterior and posterior portions and the costal stiffness and stress generally increases as the ribs go inferiorly (26). Kemper et al. described that the lateral parts of the human ribs are likely to have a significantly higher peak bending moment, peak strain, modulus, and stiffness than the anterior specimens, which means that the lateral side of the thorax should have more ductility (31). Considering their report regarding the material properties of ribs, costal fixation devices should be sufficiently strong to endure the stress of the lateral sides of inferior ribs. In our current study, rib coaptation sockets were applied to the lateral sides of inferior ribs. The result was quite satisfactory. Therefore, our PLA fiber knitted sockets were validated to have enough strength with ductility to hold the divided sections of the ribs. In contrast, the results of the 3D-printed sockets were quite unsatisfactory, which should reinforce the importance of ductile properties of rib coaptation devices.
The type A PLA fiber knitted socket showed the same ductility as and lower stiffness than the 3D-printed ones (Figure 5). Moreover, rib fixation with type A socket was successful, unlike that with 3D-printed ones. Furthermore, the displacement occurred in the dog with type C sockets implanted. Type C sockets are of highest stiffness. These findings suggest that costal fixation needs ductility rather than stiffness or strength. Another important suggestion in costal stabilization, as mentioned by Marasco and colleagues, is that the ductile properties could reduce the stress at the points of contact between the bone and fixation device, leading to reduced excessive stress with no likelihood of fixation failure (2). A metal plate or a device with more stiffness is inferior to PLA fiber knitted sockets not only in reducing stress with ductility but also in rotational stability.
Our method of knitting PLA fibers sheds new light on developing costal fixation devices. The mechanical strength of the sockets can be adjusted by changing the ratio of low-melting/high-melting point fibers and heat-processing time. Moreover, the knitting technique enables the device to possess more durability, while maintaining its ductility. For optimal strength of rib sockets for costal fixation, further analyses regarding PLA are encouraged.
Biocompatibility
In clinical settings, PLA prosthetics for chest wall reconstruction were reported to lose mass, following strength loss, in about 12 months with minimal inflammatory response (13,32). Our study period (maximal follow-up period of 7 months and minimum of 6 months) was not sufficiently long to observe absorption of the PLA-sockets. However, no infectious complications related to socket implantation were observed and inflammatory changes around the implanted sockets were radiologically minimal. Therefore, in terms of biocompatibility, our new socket system for costal approximation is satisfactory, but further investigation regarding biocompatibility is warranted.
Advantages over costal pins
We did not compare the rib fixation between costal pins and rib sockets. However, the PLA fiber knitted rib socket system is expected to have two advantages for costal fixation over costal pins. First, external fixation with costal sockets must be superior to internal fixation with rib pins. Although costal pins with different sizes are available commercially, in cases of loose cortical bone, costal pins cannot hold the divided sections of the ribs well, which can result in costal displacement. Second, contrary to the costal pins, the lengths of the PLA fiber knitted sockets can be adjusted easily by cutting with surgical scissors. Therefore, we could use optimal lengths of sockets to secure and hold the fractured ribs in a clinical setting.
3D-printed sockets were shown to be brittle and less ductile than types B and C sockets, as measured by the three-point bending apparatus. Although 3D-printed sockets were designed easily with the 3D-printer software for a variety of configurations and made by creating successive layers of PLA material extruded from the printer, layer adhesion might be loosened by hydrolysis, which eventually could be the cause of failure in our study. This is a serious consideration in 3D-printing apparatus.
In our study, three ribs in one dog with type C PLA fiber sockets were displaced radiologically 1 month after the operation. The grade of displacement remained the same throughout the follow-up period. We consider this costal displacement to be due to the smaller size of the ribs in this animal than in dogs in the other groups (Table 2), and that the socket size was not appropriate for this animal. This failure could have been prevented by using the optimal sizes of sockets. Therefore, for more reliable rib fixation, preparation of sockets of different sizes is important.
The promising next step for PLA fiber knitted sockets
First, we should develop PLA fiber knitted sockets of different sizes, to allow for size matching, because the rib displacement encountered in our study was due to a size mismatch. Second, if greater durability and ductility of the costal sockets could be achieved, the sockets could possibly be used in chest wall reconstruction, during which multiple rib resections are often performed, because these sockets could bridge the gaps between the resected segments of multiple ribs. Filling these gaps with bone regeneration material, which is a collagen scaffold, to enhance the costal regeneration for segmental bone loss could be promising.
Setbacks of PLA fiber knitted socket system
Our PLA fiber knitted socket system has two setbacks. First, our socket system was designed to stabilize the lateral and anterior ribs. Therefore, for the fixation of posterior ribs, which have thicker cortical bones and rounder cross sections with tighter radius of curvature, some modifications in the designs of the sockets should be carried out. Marasco and colleagues also raised this concern in their study regarding intramedullary rib fixation; they mentioned that no fixation devices are currently available for posterior rib stabilization (2). Second, periosteal elevation should be done for the entire circumference of the fractured ribs to insert our sockets. This periosteal dissection carries a risk of injuring the intercostal vessels.
Limitations
The present study has four limitations. First, the optimal ductility for rib coaptation could not be concluded because of the small sample size. Therefore, superiority of the PLA fiber woven sockets (types A, B, and C) could not be verified. Second, we could not confirm the bio-absorbability of PLA sockets, which requires a longer follow-up period. Third, the clinical costs of our PLA fiber costal sockets cannot be currently clarified, as these experiments were performed in animal models. However, our sockets are made of PLA fibers, and thus the cost should not be exorbitant. Last, we cannot exclude the possibility that the 3D printed sockets failed due to the choice of the animal model because of the lack of reported comparison between animals.
Conclusions
PLA fiber knitted rib coaptation sockets have been proven to be ductile and durable enough to stabilize the divided ribs in a canine model with easy handling. Further investigation on more reliable stabilization and biocompatibility is warranted for application in a clinical setting.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study was approved by the Committee for Animal Research of Kyoto University, Japan (ME232013).
References
- Granetzny A, Abd El-Aal M, Emam E, et al. Surgical versus conservative treatment of flail chest. Evaluation of the pulmonary status. Interact Cardiovasc Thorac Surg 2005;4:583-7. [Crossref] [PubMed]
- Marasco S, Quayle M, Summerhayes R, et al. An assessment of outcomes with intramedullary fixation of fractured ribs. J Cardiothorac Surg 2016;11:126. [Crossref] [PubMed]
- Marasco SF, Davies AR, Cooper J, et al. Prospective randomized controlled trial of operative rib fixation in traumatic flail chest. J Am Coll Surg 2013;216:924-32. [Crossref] [PubMed]
- Fagevik Olsen M, Slobo M, Klarin L, et al. Physical function and pain after surgical or conservative management of multiple rib fractures - a follow-up study. Scand J Trauma Resusc Emerg Med 2016;24:128. [Crossref] [PubMed]
- Kasotakis G, Hasenboehler EA, Streib EW, et al. Operative fixation of rib fractures after blunt trauma: A practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 2017;82:618-26. [Crossref] [PubMed]
- Majak P, Naess PA. Rib fractures in trauma patients: does operative fixation improve outcome? Curr Opin Crit Care 2016;22:572-7. [Crossref] [PubMed]
- Schulte K, Whitaker D, Attia R. In patients with acute flail chest does surgical rib fixation improve outcomes in terms of morbidity and mortality? Interact Cardiovasc Thorac Surg 2016;23:314-9. [Crossref] [PubMed]
- Kaplan DJ, Begly J, Tejwani N. Multiple Rib Nonunion: Open Reduction and Internal Fixation and Iliac Crest Bone Graft Aspirate. J Orthop Trauma 2017;31 Suppl 3:S34-5. [Crossref] [PubMed]
- Marasco SF, Liovic P, Sutalo ID. Structural integrity of intramedullary rib fixation using a single bioresorbable screw. J Trauma Acute Care Surg 2012;73:668-73. [Crossref] [PubMed]
- Moreno De La Santa Barajas P, Polo Otero MD, Delgado Sanchez-Gracian C, et al. Surgical fixation of rib fractures with clips and titanium bars (STRATOS System). Preliminary experience. Cir Esp 2010;88:180-6. [Crossref] [PubMed]
- Sales JR, Ellis TJ, Gillard J, et al. Biomechanical testing of a novel, minimally invasive rib fracture plating system. J Trauma 2008;64:1270-4. [Crossref] [PubMed]
- Huang KN, Xu ZF, Sun JX, et al. Stabilization of multiple rib fractures in a canine model. J Surg Res 2014;192:621-7. [Crossref] [PubMed]
- Makarawo TP, Reynolds RA, Cullen ML. Polylactide bioabsorbable struts for chest wall reconstruction in a pediatric patient. Ann Thorac Surg 2015;99:689-91. [Crossref] [PubMed]
- Pihlajamaki H, Bostman O, Hirvensalo E, et al. Absorbable pins of self-reinforced poly-L-lactic acid for fixation of fractures and osteotomies. J Bone Joint Surg Br 1992;74:853-7. [Crossref] [PubMed]
- Bostman O, Vainionpaa S, Hirvensalo E, et al. Biodegradable internal fixation for malleolar fractures. A prospective randomised trial. J Bone Joint Surg Br 1987;69:615-9. [Crossref] [PubMed]
- Hara Y, Tagawa M, Ejima H, et al. Clinical evaluation of uniaxially oriented poly-L-lactide rod for fixation of experimental femoral diaphyseal fracture in immature cats. J Vet Med Sci 1994;56:1041-5. [Crossref] [PubMed]
- Hirata T, Fukuse T, Mizuno H, et al. Clinical application of biodegradable rib connecting pins in thoracotomy. Thorac Cardiovasc Surg 1999;47:183-7. [Crossref] [PubMed]
- Iwasaki A, Hamatake D, Shirakusa T. Biosorbable poly-L-lactide rib-connecting pins may reduce acute pain after thoracotomy. Thorac Cardiovasc Surg 2004;52:49-53. [Crossref] [PubMed]
- Tatsumi A, Kanemitsu N, Nakamura T, et al. Bioabsorbable poly-L-lactide costal coaptation pins and their clinical application in thoracotomy. Ann Thorac Surg 1999;67:765-8. [Crossref] [PubMed]
- Tsunezuka Y, Iseki T, Sato H, et al. A new technique of fixing a costal coaptation pin after resection of rib segment. Asian Cardiovasc Thorac Ann 2004;12:224-6. [Crossref] [PubMed]
- Kawachi R, Watanabe S, Suzuki K, et al. Clinical application of costal coaptation pins made of hydroxyapatite and poly-L-lactide composite for posterolateral thoracotomy. Eur J Cardiothorac Surg 2008;34:510-3. [Crossref] [PubMed]
- Bemelman M, van Baal M, Yuan JZ, et al. The Role of Minimally Invasive Plate Osteosynthesis in Rib Fixation: A Review. Korean J Thorac Cardiovasc Surg 2016;49:1-8. [Crossref] [PubMed]
- Nolasco-de la Rosa AL, Mosinoz-Montes R, Matehuala-Garcia J, et al. Thoracic inestability fixed with bioabsorbable screws and plates. Acta Ortop Mex 2016;30:311-5. [PubMed]
- Yu YH, Fan CL, Hsu YH, et al. A Novel Biodegradable Polycaprolactone Fixator for Osteosynthesis Surgery of Rib Fracture: In Vitro and in Vivo Study. Materials (Basel) 2015;8:7714-22. [Crossref] [PubMed]
- Kemper AR, McNally C, Kennedy EA, et al. Material properties of human rib cortical bone from dynamic tension coupon testing. Stapp Car Crash J 2005;49:199-230. [PubMed]
- Stitzel JD, Cormier JM, Barretta JT, et al. Defining regional variation in the material properties of human rib cortical bone and its effect on fracture prediction. Stapp Car Crash J 2003;47:243-65. [PubMed]
- Komatsu T, Sato T, Sakaguchi Y, et al. The 3D-printed socket could not tolerate the bending test, resulting in snapping before being completely straightened (point of failure). Asvide 2018;5:429. Available online: http://www.asvide.com/article/view/24489
- Komatsu T, Sato T, Sakaguchi Y, et al. The PLA fiber socket showed ductile characteristics, restoring to its original curvature radius. Asvide 2018;5:430. Available online: http://www.asvide.com/article/view/24490
- Komatsu T, Sato T, Sakaguchi Y, et al. Operative video of socket implantation. Asvide 2018;5:431. Available online: http://www.asvide.com/article/view/24491
- Kyle UG, Spoede ET, Mallory GB, et al. Changes in body composition after lung transplantation in children. J Heart Lung Transplant 2013;32:800-6. [Crossref] [PubMed]
- Kemper AR, McNally C, Pullins CA, et al. The biomechanics of human ribs: material and structural properties from dynamic tension and bending tests. Stapp Car Crash J 2007;51:235-73. [PubMed]
- Tuggle DW, Mantor PC, Foley DS, et al. Using a bioabsorbable copolymer plate for chest wall reconstruction. J Pediatr Surg 2004;39:626-8. [Crossref] [PubMed]