Cardiac arrest due to coronary embolism from a metastatic sarcoma recovered through aspiration thrombectomy
Introduction
Coronary embolism in patients with metastatic cancer is an uncommon cause of acute myocardial infarction (1,2). Aspiration thrombectomy becomes necessary in specific conditions, especially in cases of large thrombus or coronary embolism. Some cases of cancer embolism, with restoration of coronary flow through percutaneous coronary intervention (PCI) using aspiration thrombectomy were reported in the literature (3,4). We report on a rare and lethal case of cardiac arrest due to acute myocardial infarction owing to coronary embolism. Coronary flow was restored and histologic confirmation was made after removal of emboli via aspiration thrombectomy.
Case presentation
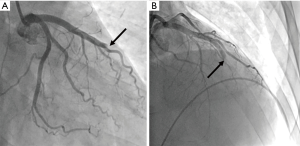
A 45-year-old male patient suffering from abrupt chest pain following cardiac arrest was transferred to our emergency department. During transport via ambulance, the patient recovered spontaneous circulation after cardiopulmonary resuscitation for 10 minutes. Initial electrocardiogram showed ST segment elevation in extensive anterior leads with reciprocal changes in inferior leads. The patient was immediately referred for primary PCI. Coronary angiography revealed that the middle left anterior descending artery (LAD) was completely occluded and the other epicardial coronary arteries had no atherosclerotic stenosis (Figure 1). Angiographic finding suggested complete occlusion by a thrombus. Aspiration thrombectomy was performed using an aspiration catheter (5.9 Fr, inner lumen 2.03 mm, ELIMINATE; Terumo, Tokyo, Japan). After five aspiration thrombectomy procedures, filling defects were observed in the guiding catheter via fluoroscopy, and arterial pressure was unchecked (Figure 2A). We gently removed the guiding catheter under negative pressure and the aspirated materials from the guiding catheter. Fibrous tissues with thrombus different from atherosclerotic thrombi were detected (Figure 2B). Arterial pressure through the femoral sheath was still undetermined. We removed the femoral sheath and large materials were drawn from it. The patient achieved vital stability after aspiration thrombectomy and we decided to discontinue the primary PCI owing to the high risk of procedure-related fatal systemic embolization.

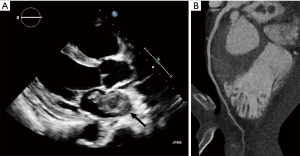
The past medical history of the patient revealed that he had been diagnosed with sarcoma at the axillary lymph node for which he underwent surgical resection following adjuvant chemotherapy and radiotherapy 6 months earlier. Transthoracic echocardiography revealed a large mass (60 mm × 30 mm size) in the left atrium (Figure 3A). Computed tomography (CT) showed that the LAD was patent without remnant embolus (Figure 3B). CT showed cancer invasion to the right pulmonary vein and left atrium from the metastatic lung cancer. The histopathological finding of the specimens through aspiration thrombectomy included anaplasia and pleomorphism of the nucleus that indicating high-grade metastatic sarcoma. The patient fully recovered from cardiac arrest and received the palliative chemotherapy.
Discussion
We report on a rare case of a 45-year-old male patient with cardiac arrest caused by a coronary embolism, who had already been treated for metastatic sarcoma. Current guidelines for ST segment elevation myocardial infarction dose not recommended routine aspiration thrombectomy before primary PCI (5), however, aspiration thrombectomy have roles in specific conditions, especially in cases of suspicious large thrombus burden or coronary embolism. We experienced coronary emboli from metastatic sarcoma and restoration of coronary flow and documented histologic diagnosis after primary PCI using aspiration thrombectomy.
Coronary embolism occurs less frequently than cerebral or renal embolization. Cheng (1) suggested the following potential explanations: (I) the discrepancy between the caliber of the aorta and that of the coronary artery; (II) the state of the coronary arteries at the root of the aorta immediately beyond the aortic valve; (III) the right-angle takeoff of the coronary arteries from the aorta; (IV) the bulk and swiftness of the blood flow in this portion of the aorta; and (V) the fact that coronary filling mainly occurs during diastole. Moreover, coronary embolism was classified into three types: direct coronary embolism, paradoxical embolism, and iatrogenic embolism (1). Causes of embolism included thrombus embolization from atrial fibrillation (73%), cardiomyopathy (25%), valvular heart disease (15%), cancer embolism (10%), septic embolism from infective endocarditis (4%), and paradoxical embolism (4%) (1,2).
Coronary embolism originating from tumors were mostly neoplasm in the left side of the heart. In benign cardiac neoplasm, coronary embolisms from left atrial myxoma and papillary fibroelastoma were reported, and fragility of neoplasm contributed to the development of coronary embolism (6). Cardiac metastases were reported to have a comparatively higher incidence compared with primary cardiac malignancy (7). In reported cases confirmed by autopsy, the main route of metastatic cancer causing coronary embolism were through the pulmonary veins from lung metastases and direct invasion to the left atrium (3,8). Earlier two cases of coronary embolism were diagnosed by histologic examination through aspiration thrombectomy (3,4). Šteiner and Vojáček (3) reported a case of coronary embolism from colonic adenocarcinoma, in which they focused on pathologic diagnosis. Noguchi et al. (4) reported a case of multiple coronary embolism from metastatic myxofibrosarcoma. In the present case, we successfully removed the large emboli from metastatic sarcoma by using aspiration catheter.
It is not easy to consider coronary embolism from cancer during primary PCI. The recently proposed scoring system from the Japan National Cardiovascular Center criteria for coronary embolism will be helpful in differentiating coronary embolism from atherosclerotic thrombi in clinical practice and research (2). The medical history of the patient, coronary angiographic findings, and additive imaging studies including echocardiography and CT are essential for the application of the criteria. Evaluation of clinical context from past medial history, cardiovascular risk factors, image work-up including chest X-ray and echocardiography may provide insight into the etiology of the acute myocardial infarction. Aspiration thrombectomy can be a helpful method for diagnosis and treatment when coronary embolism is considered. Operators should aim to select the most effective method and devices for revascularization of coronary vessels in case of suspicious coronary embolism. Moreover, each step of the procedure needs great caution to prevent the complication of procedure-related systemic embolism. Characteristics of the aspirated material should be considered according to clinical context.
We report on a rare and lethal case of cardiac arrest due to a coronary embolism from a metastatic sarcoma. Histopathologic diagnosis and restoration of coronary flow were ensured via aspiration thrombectomy without systemic complication.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written consent was obtained from the patient for publication of this manuscript and any accompanying images.
References
- Cheng TO. Coronary embolism. Int J Cardiol 2009;136:1-3. [Crossref] [PubMed]
- Shibata T, Kawakami S, Noguchi T, et al. Prevalence, Clinical Features, and Prognosis of Acute Myocardial Infarction Attributable to Coronary Artery Embolism. Circulation 2015;132:241-50. [Crossref] [PubMed]
- Steiner I, Vojáček J. Carcinoma embolization in coronary artery causing myocardial infarction: diagnosis from coronary thromboaspirate. Pathol Res Pract 2014;210:198-200. [Crossref] [PubMed]
- Noguchi M, Yamada Y, Sakakura K, et al. Coronary thrombus aspiration revealed tumorous embolism of myxofibrosarcoma from the left atrium. Cardiovasc Interv Ther 2016;31:75-8. [Crossref] [PubMed]
- Windecker S, Kolh P, Alfonso F, et al. 2014 ESC/EACTS guidelines on myocardial revascularization. EuroIntervention 2015;10:1024-94. [Crossref] [PubMed]
- Chiba N, Matsuzaki M, Furuya S, et al. Complete occlusion of the left main trunk coronary artery by a cardiac papillary fibroelastoma in a hemodynamically unstable patient. J Cardiol Cases 2016;13:97-100. [Crossref]
- Bussani R, De-Giorgio F, Abbate A, et al. Cardiac metastases. J Clin Pathol 2007;60:27-34. [Crossref] [PubMed]
- Kumagai N, Miura SI, Toyoshima H, et al. Acute myocardial infarction due to malignant neoplastic coronary embolus. J Cardiol Cases 2010;2:e123-7. [Crossref]


