Pyrexia in patients with uncontrolled systemic hypertension: could they have an aortic dissection?
Introduction
Aortic dissection is a potentially life threatening disease, consequently, obtaining a diagnosis quickly is vital and can affect the patients mortality and morbidity. The exact cause of aortic dissection is unknown but uncontrolled hypertension is among one of the most common risk factors (1). It classically presents with severe chest pain, which radiates to the back but there has been a diverse set of clinical features documented and can present painlessly (2). There have been some reports of fever being a feature of an acute aortic dissection but it is rarely the main presenting complaint (3).
We describe two cases of delayed diagnosis of type B aortic dissection where fever was the presenting feature in patients who had uncontrolled hypertension. In both cases there was also an incidental finding of a small, left sided pleural effusion.
Case reports
Case 1
Case 1 is of a 42-year-old female, 6 months post-partum, with a past medical history of hypertension. This patient was taking a once daily dose of amlodipine (10 mg) at the time of presentation, however, her hypertension remained uncontrolled with a systolic blood pressure of more than 170 mmHg. She presented to a general hospital with symptoms of epigastric pain, vomiting and pyrexia, and was admitted to a medical ward. Investigations included abdominal ultrasound, echocardiogram, upper gastro-intestinal (GI) endoscopy, urine and blood cultures; no abnormalities were detected. Inflammatory markers were raised [white cell count (WCC) 12.5×109 g/dL, C-reactive protein (CRP) 126 mg/L and erythrocyte sedimentation rate (ESR) 36 units] and she had persistent pyrexia of around 38.5 °C. The coagulation function was also normal [platelets (PLT) 255000, international normalized ratio (INR) 1.18, activated partial thromboplastin time (APTT) 34 s, prothrombin time (Pt) 12 s, Fibrinogen 240 mg/dL). After 12 days with persistent symptoms, not changing from presentation, a CT of the chest, abdomen and pelvis was done. This demonstrated a type B aortic dissection extending from the origin of the left subclavian artery to the left iliac artery, there was no evidence of mal-perfusion. Additionally, there was a small left sided pleural effusion (Figure 1). The patient was then transferred to a cardiothoracic unit on the same day; her hypertension was treated with intravenous glyceryl trinitrate and esmolol. Raised inflammatory markers were thought to be due to an inflammatory process originating from the aortic haematoma. The next day a stent graft was inserted through the right femoral artery and was placed between the origin of the left subclavian artery and the aorta at the level of the seventh thoracic vertebra. Angiogram immediately after insertion showed correct position with no endo-leak (Figure 2).
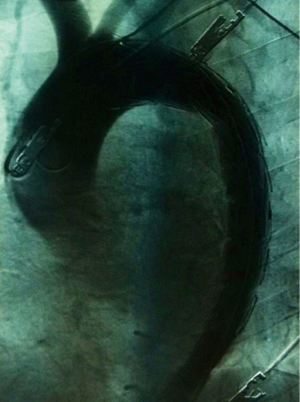
Post procedure she remained haemodynamically stable (blood pressure around 110/80 mmHg). Hypertension postoperatively was treated with Exforge® (a combination drug of amlodipine and valsartan). Follow up CT scan at day 4 and 3 months post procedure both showed good placement of the stent without any endo-leaks. The 3-month scan showed minimal haematoma.
Case 2
Case 2 is of a 48-year-old male, overweight, smoker with uncontrolled hypertension (not medicated). He presented to the A&E department with a 5-day history of epigastric pain, vomiting and pyrexia. At presentation his systolic blood pressure was more than 170 mmHg. He was admitted to a medical ward and underwent blood and urine cultures, abdominal ultrasound scan which showed no abnormalities. Upper GI endoscopy demonstrated an area of mild gastritis in the pyloric antrum which was biopsied at the time but this was not thought to be contributing to the on-going symptoms. Similarly to the first case, the patient remained pyrexic throughout admission and WCC and CRP were raised (13.2×109 and 126 respectively). The coagulation function was normal (PLT 315,000, INR 1.25, APTT 33 s, Pt 13 s, Fibrinogen 270 mg/dL), too. After 12 days, a CT scan of the abdomen demonstrated dissection at the level of the diaphragm, and therefore the radiologist progressed to scan the remaining thorax which demonstrated a type B aortic dissection with the presence of haematoma, a small left sided pleural effusion and small pericardial collection. This patient underwent the same procedure and follow up as case 1, his hypertension was also controlled with intravenous GTN and esmolol preoperatively and Exforge®, post operatively. The fever resolved in the post-operative period and the inflammatory makers normalised. CT scan at day 4 and 3 months showed reducing size of haematoma and no leaks.
Discussion
The two cases described above demonstrate that pyrexia, in the absence of an obvious source with negative investigations, in a patient with a background of uncontrolled hypertension, could be a presenting feature of an aortic dissection. In both cases there was a considerable time delay between presentation and diagnosis which could have potentially been avoided had dissection been included in the original differential diagnosis and subsequent appropriate investigations been done in a timely manner.
A retrospective case series from Spain in 2010 also describes fever as a feature of aortic dissection, most frequently in type B dissections (3). Fever tended to be low grade and the patient was generally well when compared with a patient who has a fever caused by infection. This case series looked at patients with a diagnosis of aortic dissection and then identified those who had a fever as part of the acute episode. They determined the difference between a fever due to the inflammatory process as a result of a dissection and fever due to an intercurrent infection, they do not however suggest that fever can be the prominent presenting feature of an acute aortic dissection, as with two cases previously described.
In both cases described, the CT scan which diagnosed the aortic dissection also revealed a small left sided pleural effusion. Similar presentations have been described before, a retrospective review published in 2012 of 71 patients presenting with fever and a pleural effusion of unknown aetiology described three cases which had large thoracic vessel pathology. One of these patients had an aortic dissection (the two other patients had giant cell arteritis and Takayasu arteritis). In all three of these cases the pleural effusion was left sided, small-moderate in size and non-diagnostic on thoracocentesis. The effusions resolved following treatment (4). All patients presenting with fever would have a chest X-ray as part of a septic screen as an early investigation. Identification of a pleural effusion at this early stage in the absence of any other positive investigations could provide a clue that there may be aortic pathology and prompt appropriate investigation.
An inflammatory reaction to the aortic dissection can explain the pyrexia and raised inflammatory markers in these patients. As the left pleura are in contact with the aorta this may explain why the pleural effusions were always left sided. Inflammation of the aorta from a dissection could irritate the pleura leading to a reactionary effusion (5).
The right pleura is away from the aorta and in contact with the major veins in the thorax. Sato et al. analyzed 66 patients with aortic dissection, there were 16 pleural effusion cases found (3 type A and 13 type B classification). The result also suggested that transient rupture or leakage in descending aortic dissection was the possibly mechanism of pleural effusion (6).
Conclusions
Physicians should remember the association of pyrexia and left sided pleural effusion with aortic dissection when investigating patients with similar presentations, especially if they are known to have uncontrolled hypertension. Although it is a rare cause of these symptoms, it is important and missing the diagnosis could lead to catastrophic consequences to the patient.
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- Larson EW, Edwards WD. Risk factors for aortic dissection: a necropsy study of 161 cases. Am J Cardiol 1984;53:849-55. [PubMed]
- Yamada S, Tokumoto M, Ohkuma T, et al. Slowly progressive and painless thoracic aortic dissection presenting with a persistent Fever in an elderly patient: the usefulness of combined measurement of biochemical parameters. Case Rep Med 2013;2013:498129.
- García-Romo E, López-Medrano F, Llovet A, et al. Fever due to inflammation in acute aortic dissection: Description and proposals for diagnostic and therapeutic management. Rev Esp Cardiol 2010;63:602-6. [PubMed]
- Schattner A, Klepfish A. Left pleural effusion and fever of unknown origin--a clue to thoracic arterial pathology. J Gen Intern Med 2012;27:1084-7. [PubMed]
- Yamada S, Tokumoto M, Ohkuma T, et al. Slowly progressive and painless thoracic aortic dissection presenting with a persistent Fever in an elderly patient: the usefulness of combined measurement of biochemical parameters. Case Rep Med 2013;2013:498129.
- Sato F, Kitamura T, Kongo M, et al. Newly diagnosed acute aortic dissection: characteristics, treatment modifications, and outcomes. Int Heart J 2005;46:1083-98. [PubMed]



