Uniportal video-assisted thoracoscopic surgery right upper lobectomy with systematic lymphadenectomy in a semiprone position
Introduction
With the development of thoracoscopic instruments and techniques, video-assisted thoracoscopic surgery (VATS) lobectomy has become the first choice for early stage non-small-cell lung carcinoma. Most surgeons prefer three-port or four-port VATS lobectomy, because multiple ports provide different angles facilitating better dissection and division of the bronchus and vessels. We performed our first uniportal VATS lobectomy in November 2013, and both the surgeon and the assistant felt very fatigued after the operation. In an effort to achieve better ergonomics, we performed our first uniportal VATS lobectomy in a semiprone position in May 2014.
Clinical data
A 53-year-old male smoker was referred to our hospital due to an enlarged lesion in his right upper lung. Computed tomography (CT) showed a 1.5 cm solid lesion with pleural indentation in the right upper lobe adjacent to the oblique fissure. No metastases or contraindications were found in the preoperative evaluation. The clinical diagnosis was stage I primary lung cancer. Uniportal VATS right upper lobectomy in a semiprone position was performed (Figure 1). Intraoperative frozen section examination confirmed lung adenocarcinoma, and systematic lymphadenectomy was then performed.

Operative techniques
The patient was placed in a semiprone position under general anaesthesia, with single-lung ventilation provided by a double-lumen endotracheal tube. Thoracic paravertebral block was used. The surgeon and the sole assistant participating in the operation both stood on the ventral side of the patient. A single incision was employed, which was 3.5 cm long and positioned at the fifth intercostal space on the anterior axillary line. A plastic wound protector was used to prevent the lung from expanding when suction was applied. A high definition 30° 10 mm thoracoscope was placed at the posterior part of the incision.
The instruments used were a harmonic scalpel, curved suction device, endoscopic grasper, double-jointed forceps and endoscopic linear cutter. An endoscopic grasper containing a small gauze was used to push the lung to promote exposure.
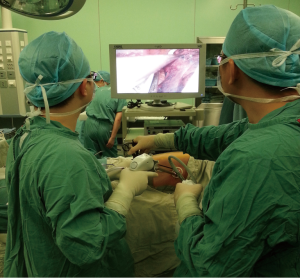
The surgeon stood caudally, while the assistant stood cranially. The surgeon held the suction in the left hand, and the harmonic scalpel (or sometimes the double-jointed forceps or the endoscopic linear cutter) in the right hand. The assistant held the thoracoscope in one hand and the endoscopic grasper in the other hand (Figure 2).
We began the procedure with exploration to find the lesion, locating it in the right upper lobe with pleural indentation, no metastases in the pleurae, complete oblique fissure and poor horizontal fissure. The oblique fissure was divided with a harmonic scalpel, and the ascending A2 pulmonary artery was exposed. The ascending A2 was closed proximally with two 5-mm vascular clips and then cut with a harmonic scalpel. The posterior mediastinal pleura was opened until the upper edge of the right upper bronchus was visible. The 12th group lymph nodes were dissected to the distal lung.
The right upper lobe was pushed down to expose the apico-anterior pulmonary arterial trunk. The apical artery and anterior artery branched from the right pulmonary arterial trunk separately in this case. The apical artery was mobilised, and cut with an endoscopic linear stapler, whereas the anterior artery was hard to expose at this angle. The 12th group lymph nodes between the upper right bronchus and apical artery were dissected to the distal lung at this angle. The right upper bronchus was mobilised with double-jointed forceps from the dorsal aspect, then transected with an endoscopic linear stapler. The anterior artery was then exposed dorsally, and cut with an endoscopic linear stapler.
The right upper lobe was pushed backwards. The right upper pulmonary vein was mobilised, and then cut with an endoscopic linear stapler. The 11th group lymph nodes were dissected before the horizontal fissure was cut with an endoscopic linear stapler. The specimen was put into a protected bag, and removed for frozen section examination. Lung adenocarcinoma was confirmed, and systematic lymphadenectomy was performed.
The lung was pushed downwards by the assistant. The surgeon lifted the azygos vein via suction, and dissected the 4th group lymph nodes with a harmonic scalpel. After an approximately 1 cm length of the pericardium was exposed, the mediastinal pleura above the azygos vein was opened. The 2nd and 4th lymph nodes were dissected en bloc, with the right vagus nerve left untouched.
The lung was pushed forwards by the assistant. The posterior mediastinal pleura was opened in front of the right vagus nerve, from the right inferior pulmonary vein to the azygos vein. The oesophagus was separated from the 7th group lymph nodes, and the bilateral main bronchus was exposed. The 7th group lymph nodes were then dissected en bloc. The inferior pulmonary ligament was mobilised, and the 9th group lymph nodes were dissected. A chest tube was placed at the posterior part of the incision through the posterior thoracic cavity to the apex.
Comments
Uniportal VATS lobectomy was first reported by Gonzalez-Rivas et al. (2) in 2011. Gonzalez-Rivas et al. (2) proved the practical feasibility and safety of uniportal VATS lobectomy, and utilised the technique in more complex cases, including double sleeve lobectomy. The patient was placed in the lateral decubitus position in previous reports. Under such conditions, the cameraman is required to raise their arm to hold the thoracoscope, which easily leads to arm fatigue.
A prone position was utilised in thoracoscopic mobilisation of the oesophagus (3), and subsequently a semiprone position was investigated, due to the convenience of relatively uncomplicated conversion to thoracotomy, where required. A semiprone position is now widely utilised in thoracoscopic mobilisation of the oesophagus, because it reduces workload and facilitates better ergonomics (4). However, it is seldom utilised for VATS lobectomy (5).
We first performed uniportal VATS lobectomy in a semiprone position in May 2014, and achieved great success. Not only does a semiprone position relieve arm fatigue in the surgeon and assistant, but it also provides more angles for the surgeon. In this operation, only three instruments are inserted into the thoracic cavity at the same time, and they rarely interfere with each other because they are all slim. More than 20 patients have now successfully received uniportal VATS lobectomy in a semiprone position.
The most difficult manipulation during uniportal VATS right upper lobectomy is the division of the right upper pulmonary vein. Initial division of the anterior trunk can facilitate the insertion of a stapler to divide the right upper pulmonary vein. The anterior pulmonary artery could be divided apically or dorsally after cutting the right upper bronchus.
The oblique fissure is divided first, if the interlobar pulmonary is visible in the fissure. Otherwise, the oblique fissure is divided last. The horizontal fissure is divided last, unless it is completely developed. We did not grasp the lung or the lymph nodes throughout the operation, in order to reduce the possibility of trauma to the lung, and avoid crushing the lymph nodes. The lung was pushed to the appropriate angle using an endoscopic grasper containing a gauze, and a curved suction instrument. The lymph nodes were pushed to the appropriate angle via a curved suction instrument only. In uniportal VATS lobectomy, a semiprone position facilitates pushing of the lung, and facilitates more manipulation angles, less workload and better ergonomics for both the surgeon and the assistant.
Acknowledgements
Disclosure: The authors declare no conflicts of interest.
References
- Lin Z, Xu S, Wang Q. Uniportal video-assisted thoracoscopic surgery right upper lobectomy with systematic lymphadenectomy in a semiprone position. Asvide 2014;1:368. Available online: http://www.asvide.com/articles/402
- Gonzalez-Rivas D, Delgado M, Fieira E, et al. Double sleeve uniportal video-assisted thoracoscopic lobectomy for non-small cell lung cancer. Ann Cardiothorac Surg 2014;3:E2. [PubMed]
- Palanivelu C, Prakash A, Senthilkumar R, et al. Minimally invasive esophagectomy: thoracoscopic mobilization of the esophagus and mediastinal lymphadenectomy in prone position--experience of 130 patients. J Am Coll Surg 2006;203:7-16. [PubMed]
- Shen Y, Feng M, Tan L, et al. Thoracoscopic esophagectomy in prone versus decubitus position: ergonomic evaluation from a randomized and controlled study. Ann Thorac Surg 2014;98:1072-8. [PubMed]
- Agasthian T. Revisiting the prone position in video-assisted thoracoscopic surgery. Asian Cardiovasc Thorac Ann 2010;18:364-7. [PubMed]


