
The impact of immune-inflammation-nutritional parameters on the prognosis of non-small cell lung cancer patients treated with atezolizumab
Introduction
Lung cancer is the leading cause of cancer-related deaths worldwide, and non-small cell lung cancer (NSCLC) accounts for approximately 85% of all lung cancers (1). Although in some cases the genetic pathogenesis associated with the development and progression of NSCLC, such as epidermal growth factor (EGFR) mutations or anaplastic lymphoma kinase (ALK) rearrangements, has been elucidated, the prognosis of metastatic or recurrent disease after surgical resection remains very poor.
Over the past decade, the therapeutic strategies for advanced NSCLC have dramatically changed. Immune checkpoint inhibitors (ICIs) targeting programmed death-1 (PD-1) and programmed death-ligand 1 (PD-L1) have shown favorable clinical outcomes compared with standard chemotherapy in several clinical studies (2-4). Atezolizumab, a monoclonal antibody against PD-L1 protein, was approved for the treatment of patients with metastatic NSCLC who were identified with disease progression during or following platinum-based chemotherapy based on the OAK study (4). Moreover, combining Atezolizumab and cytotoxic chemotherapy has emerged as the novel first line strategy for advanced NSCLC patients (5,6). Notably, this single agent statistically improved overall patient survival regardless of PD-L1 expression. However, its efficacy for patients with PD-L1-negative expression was less significant. There are several reports of biomarkers that show prognostic response to ICIs, including PD-L1 expression by immunohistochemistry and tumor mutational burden by next-generation sequencing (7-9). However, a predictive biomarker for response to atezolizumab is unclear.
Recently, several studies supported evidence that patient prognosis is determined not only by tumor characteristics but also by patient factors. Among these factors, host inflammation or immune-nutritional index have attracted attention as prognostic factors and biomarkers to predict response to anti-cancer drugs. We hypothesized that the host’s immunonutrition status is associated with a therapeutic effect of atezolizumab. Thus, we retrospectively investigated the relationship between several patient immune-inflammation-nutritional parameters and the clinical outcome of atezolizumab at a single institution.
Methods
Patients
From January 2018 to March 2019, we retrospectively enrolled 24 consecutive NSCLC patients treated with atezolizumab (Tecentriq, Genentech, approved January 2018 in Japan) at the Department of Thoracic Oncology, National Hospital Organization Kyushu Cancer Center. These patients were diagnosed with unresectable advanced-stage NSCLC or recurrent disease after pulmonary resection and had received at least one regimen of cytotoxic chemotherapy before being administered atezolizumab. Pathological stage was defined according to the criteria of the eighth edition of the TNM classification by the International Association for the Study of Lung Cancer (10). In addition, the following clinicopathological characteristics were investigated: age at atezolizumab therapy, sex, performance status (PS), smoking status, histological type, EGFR, ALK mutational status, and PD-L1 expression by immunohistochemistry (monoclonal antibody, 22C3, Dako, Carpinteria, CA, USA).
Atezolizumab was administered to the patients on day 1 every 3–4 weeks, which was continued until disease progression, discontinuation by treatment-related adverse events, or death. All patients were carefully assessed for treatment response based on the Response Evaluation Criteria in Solid Tumors (RECIST) version 1.1 every 6–10 weeks (11).
Written informed consent was obtained from each patient before inclusion in this study. This study was approved by the Institutional Review Board of National Hospital Organization Kyushu Cancer Center.
Immune-inflammation-nutritional parameters
We evaluated pretreatment immune-inflammation-nutritional parameters that had accumulated within the 10 days preceding atezolizumab treatment. The prognostic nutritional index (PNI) was calculated as follows: 10 × serum albumin (g/dL) + 0.005 × total lymphocyte count (/mm3). Neutrophil/lymphocyte ratio (NLR) and platelet/lymphocyte ratio (PLR) were defined as whole neutrophils or the total number of platelets divided by whole lymphocytes. Modified Glasgow prognostic score (mGPS) was evaluated as described previously (12).
Because of the relatively small number of patients, the optimal cut-off value was not determined by a receiver operative curve. Thus, the cut-off value of each parameter was determined by previous reports. The cut-off values of NLR and PLR were set by Kunizaki et al. (13), and that of PNI was set by Okada et al. (14): NLR =5, PLR =150, and PNI =48. A mGPS score of 2 was regarded as the high mGPS group.
Statistical analysis
We performed statistical evaluations using JMP software version 14 (SAS Institute Inc., Cary, NC, USA). Continuous variables are expressed as the mean and standard deviation, and categorical variables are expressed as numbers and were analyzed using a two-sided Fisher’s exact test. Univariate analysis of the associations between the immune-nutritional parameters and clinicopathological factors was performed using logistic regression analysis. Overall survival (OS) was defined as the interval between the date of atezolizumab initiation and the date of the last follow-up or death. Time to treatment failure (TTF) was defined as the time between the date of atezolizumab initiation and the date of the last follow-up or discontinuation of atezolizumab. OS and TTF rates were analyzed using the Kaplan-Meier method with the log-rank test. We performed univariate and multivariate analyses to estimate the hazard ratios (HRs) for independent prognostic values via Cox proportional hazards regression models with the backward elimination method including following variables: age, sex, smoking history, performance status, treatment line, PD-L1 expression, and immune-inflammation-nutritional parameters (PNI, NLR, PLR, and mGPS status). A P value of <0.05 was regarded as significant.
Results
Patient characteristics and immune-inflammation-nutritional parameters
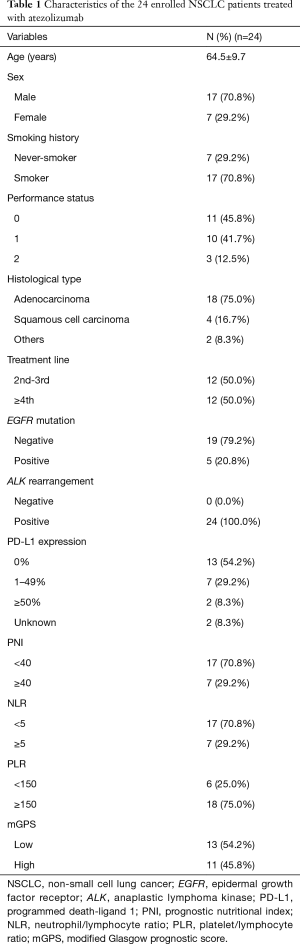
Table 1 shows the baseline of the 24 enrolled patients. Overall, the median age was 64.5 years (range, 49–82 years), while 70.8% of patients were male and smokers. Approximately half showed a good performance status (n=11, 45.8%), and the major histological type was adenocarcinoma (n=18, 75.0%). EGFR mutations were identified in five patients, but none had ALK rearrangements. Regarding PD-L1 expression in tumor tissues, over half of the cases showed no expression (n=13, 54.2%), seven patients showed moderate expression (1–49%), and two patients showed high expression (over 50%). The PD-L1 data of two patients were not available.
Full table
We calculated each immune-inflammation-nutritional parameter. Seventeen patients (70.8%) showed low pretreatment PNI levels (<40), and a minority of patients showed a high NLR (29.2%) and a low PLR (25.0%). High mGPS score was identified in 11 patients (45.8%).
Association between immune-inflammation-nutritional parameters and tumor response
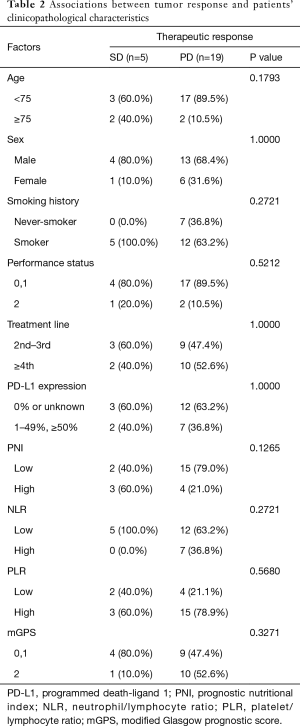
Next, we investigated the relationship between tumor response and clinicopathological characteristics including immune-inflammation-nutritional parameters. There were no patients with partial response or complete response to atezolizumab. As shown in Table 2, the disease control rate of atezolizumab was 20.8% (5/24), and there were no significant associations between tumor response and clinical characteristics. However, pretreatment PNI was higher and NLR levels was lower in patients with SD than in those with PD (P=0.1265 and P=0.2721, respectively). In addition, disease control tended to be experienced if atezolizumab was started within four treatment lines (P=0.0530).
Full table
Prognostic significance of immune-nutritional parameters
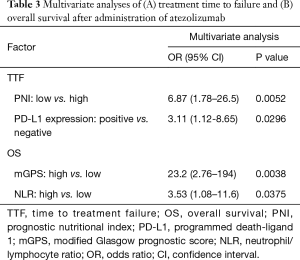
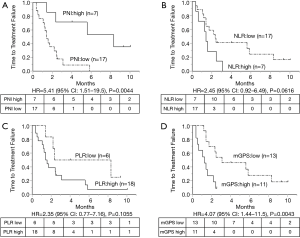
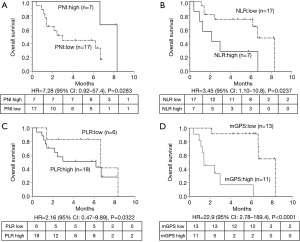
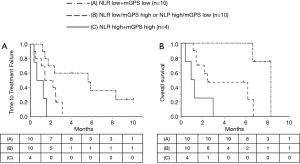
Finally, we analyzed TTF and OS after atezolizumab according to age, sex, performance status, treatment line, PD-L1 expression, and each immune-nutritional parameter. Older age, sex, treatment line, and PD-L1 expression were not significantly associated with TTF and OS after atezolizumab initiation. Figures 1 and 2 show the Kaplan-Meier analyses of TTF and OS stratified by each immune-inflammation-nutritional parameter. These analyses showed that the low PNI group had significantly shorter TTF and OS after atezolizumab than the high PNI group [(Figure 1A) TTF: HR =5.41, P=0.0044; (Figure 2A) OS: HR =7.28, P=0.0283)], while the high NLR group had shorter TTF and OS than the low NLR group [(Figure 1B) TTF: HR =2.45, P=0.0616; (Figure 2B) OS: HR =3.45, P=0.0237], and patients with high mGPS experienced significantly shorter TTF and OS than those with low mGPS [(Figure 1D) TTF: HR =4.07, P=0.0043; (Figure 2D) OS: HR =22.9, P<0.0001)]. In addition, multivariate analyses showed that low PNI was an independent predictor of short TTF (HR =6.87, P=0.0052, Table 3), and high NLR and high mGPS were independent prognostic factors for OS after atezolizumab (NLR: HR =3.53, P=0.0375; mGPS: HR =23.2, P=0.0038, Table 3). Based on the survival results, we analyzed the survival risk according to patients’ NLR and mGPS status. As shown in Figure 3, survival analyses revealed a much worse prognosis in patients with NLR high/mGPS high [NLR high/mGPS high vs. NLR low/mGPS low: TTF, HR =10.8, 95% confidence interval (CI): 2.32–50.2, P=0.0024; OS, HR =58.1, 95% CI: 5.48–616, P=0.0007].

Full table
Discussion
ICIs have emerged as novel therapeutic strategies in NSCLC patients. Several clinical factors were reported as predictive biomarkers of response to ICIs (8,9,15). However, biomarkers for predicting response to atezolizumab have yet to be elucidated. In the present study, we showed that host immune-nutritional parameters were associated with treatment time and survival in patients treated with atezolizumab for second- or further-line treatment. These results are novel findings for thoracic oncologists.
ICIs block inhibitory receptors such as PD-1 and its ligand, PD-L1, and thus tumor-specific T-cells are activated and exert effector functions on tumor cells. In this effector phase, activated T-cells infiltrate and attack tumor sites. Atezolizumab is such an ICI, targeting PD-L1 and inhibiting PD-1/PD-L1 function. It is well established that PD-L1 expression in tumor specimens is an important factor that predicts response to ICIs in NSCLC. However, some patients did not benefit from the inhibitors despite positive PD-L1 expression. Nonetheless, there were several patients with negative PD-L1 expression who responded favorably to these agents. Thus, there might be predictive biomarkers other than PD-L1 expression. Unfortunately, predictive factors for response to atezolizumab are unclear. Thus, we focused on host immune-nutritional and inflammation status for atezolizumab therapy in this study.
Inflammation is known to be an important factor in tumor progression, and has a role in epigenetic alterations in cancer (16). Previous studies elucidated that several hematological markers reflect patient inflammation or immune reaction, which are associated with poor survival in patients with various carcinomas including NSCLC (14,17,18). In addition, these markers have attracted attention and have been investigated as novel biomarkers to predict response to ICIs, giving information about patient immune status simply and inexpensively. Ogata et al. demonstrated that high NLR both before first nivolumab administration and two weeks after administration was associated with short progression-free survival (PFS) in advanced gastric cancer (19). The cut-off value of NLR in this previous report was the same as in the present study. In NSCLC patients, pretreatment PNI levels were associated with response to ICI therapy and were an independent prognostic factor for PFS and OS (PFS: HR =1.704, OS: HR =1.606) (20). Furthermore, we previously reported that pretreatment control the nutritional status score has a potential application as a predictor of therapeutic effect and prognosis of NSCLC patients treated with pembrolizumab (21). The present study showed that a low PNI level was an independent predictor of short TTF, and high NLR and mGPS were independent prognostic factors for OS in patients treated with atezolizumab. As can be seen from these results, pretreatment immune-nutritional and inflammation status seems to be strongly correlated with outcomes for ICI therapy including atezolizumab.
GPS and mGPS are classified into three stages according to serum albumin and C-reactive protein (CRP). This score reflects both host-related systemic inflammatory response and nutritional status. Several reports have elucidated that high GPS or mGPS is associated with poor survival in NSCLC. Leung et al. showed that increased mGPS was likely linked to poor PS and be independently associated with poor cancer-specific survival in 261 inoperable NSCLC patients (22). Likewise, Jiang et al. reported that GPS was positively correlated with serum tumor markers and was an independent prognostic factor for PFS and OS in advanced NSCLC patients (23). Focusing on the possibility of a therapeutic effect of GPS or mGPS, Fujio et al. reported that high GPS decreased the therapeutic efficacy of platinum combination therapy for advanced NSCLC patients (24). Kasahara et al. investigated the therapeutic significance of post-treatment GPS in advanced NSCLC patients treated with anti-PD1 treatment. They concluded that post-treatment GPS independently predicted the efficacy of anti-PD1 treatment for NSCLC. In Figure 2, we performed survival analyses on the groups classified by NLR and mGPS status. The group with high NLR and mGPS had significantly shorter TTF and OS than that with low NLR and mGPS. These results suggested that patients who have both inflammation and malnutrition are not likely to benefit from atezolizumab.
The present study has several potential limitations. First, it was a retrospective study performed at a single institution. Second, the number of enrolled patients was too small to establish the therapeutic significance of host immune-inflammation-nutritional parameters. Prospective studies or multicenter studies are needed to validate our results. Finally, the disease control rate of the present study was lower than OAK study (4). This result may be caused by the patient population half of which was administered atezolizumab in 4th line or later.
In conclusion, the therapeutic and prognostic benefit of atezolizumab may be subject to the host immune-inflammation-nutritional status. Future validation of these important results is needed.
Acknowledgments
We thank H. Nikki March, PhD, from Edanz Group (www.edanzediting.com/ac) for editing a draft of this manuscript.
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jtd.2020.02.27). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. This study was approved by the Institutional Review Board of National Hospital Organization Kyushu Cancer Center. Written informed consent was obtained from each patient before inclusion in this study.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin 2019;69:7-34. [Crossref] [PubMed]
- Borghaei H, Paz-Ares L, Horn L, et al. Nivolumab versus Docetaxel in Advanced Nonsquamous Non-Small-Cell Lung Cancer. N Engl J Med 2015;373:1627-39. [Crossref] [PubMed]
- Garon EB, Rizvi NA, Hui R, et al. Pembrolizumab for the treatment of non-small-cell lung cancer. N Engl J Med 2015;372:2018-28. [Crossref] [PubMed]
- Rittmeyer A, Barlesi F, Waterkamp D, et al. Atezolizumab versus docetaxel in patients with previously treated non-small-cell lung cancer (OAK): a phase 3, open-label, multicentre randomised controlled trial. Lancet 2017;389:255-65. [Crossref] [PubMed]
- Socinski MA, Jotte RM, Cappuzzo F, et al. Atezolizumab for First-Line Treatment of Metastatic Nonsquamous NSCLC. N Engl J Med 2018;378:2288-301. [Crossref] [PubMed]
- West H, McCleod M, Hussein M, et al. Atezolizumab in combination with carboplatin plus nab-paclitaxel chemotherapy compared with chemotherapy alone as first-line treatment for metastatic non-squamous non-small-cell lung cancer (IMpower130): a multicentre, randomised, open-label, phase 3 trial. Lancet Oncol 2019;20:924-37. [Crossref] [PubMed]
- Reck M, Rodriguez-Abreu D, Robinson AG, et al. Pembrolizumab versus Chemotherapy for PD-L1-Positive Non-Small-Cell Lung Cancer. N Engl J Med 2016;375:1823-33. [Crossref] [PubMed]
- Sacher AG, Gandhi L. Biomarkers for the Clinical Use of PD-1/PD-L1 Inhibitors in Non-Small-Cell Lung Cancer: A Review. JAMA Oncol 2016;2:1217-22. [Crossref] [PubMed]
- Lu S, Stein JE, Rimm DL, et al. Comparison of Biomarker Modalities for Predicting Response to PD-1/PD-L1 Checkpoint Blockade: A Systematic Review and Meta-analysis. JAMA Oncol 2019. [Epub ahead of print]. [Crossref] [PubMed]
- Nicholson AG, Chansky K, Crowley J, et al. The International Association for the Study of Lung Cancer Lung Cancer Staging Project: Proposals for the Revision of the Clinical and Pathologic Staging of Small Cell Lung Cancer in the Forthcoming Eighth Edition of the TNM Classification for Lung Cancer. J Thorac Oncol 2016;11:300-11.
- Eisenhauer EA, Therasse P, Bogaerts J, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 2009;45:228-47. [Crossref] [PubMed]
- Jin J, Hu K, Zhou Y, et al. Clinical utility of the modified Glasgow prognostic score in lung cancer: A meta-analysis. PLoS One 2017;12:e0184412. [Crossref] [PubMed]
- Kunizaki M, Tominaga T, Wakata K, et al. Clinical significance of the C-reactive protein-to-albumin ratio for the prognosis of patients with esophageal squamous cell carcinoma. Mol Clin Oncol 2018;8:370-4. [PubMed]
- Okada S, Shimada J, Kato D, et al. Clinical Significance of Prognostic Nutritional Index After Surgical Treatment in Lung Cancer. Ann Thorac Surg 2017;104:296-302. [Crossref] [PubMed]
- Bence C, Hofman V, Chamorey E, et al. Association of combined PD-L1 expression and tumour-infiltrating lymphocyte features with survival and treatment outcomes in patients with metastatic melanoma. J Eur Acad Dermatol Venereol 2019. [Epub ahead of print]. [Crossref] [PubMed]
- Murata M. Inflammation and cancer. Environ Health Prev Med 2018;23:50. [Crossref] [PubMed]
- Li Z, Xu Z, Huang Y, et al. Prognostic values of preoperative platelet-to-lymphocyte ratio, albumin and hemoglobin in patients with non-metastatic colon cancer. Cancer Manag Res 2019;11:3265-74. [Crossref] [PubMed]
- Pirozzolo G, Gisbertz SS, Castoro C, et al. Neutrophil-to-lymphocyte ratio as prognostic marker in esophageal cancer: a systematic review and meta-analysis. J Thorac Dis 2019;11:3136-45. [Crossref] [PubMed]
- Ogata T, Satake H, Ogata M, et al. Neutrophil-to-lymphocyte ratio as a predictive or prognostic factor for gastric cancer treated with nivolumab: a multicenter retrospective study. Oncotarget 2018;9:34520-7. [Crossref] [PubMed]
- Shoji F, Takeoka H, Kozuma Y, et al. Pretreatment prognostic nutritional index as a novel biomarker in non-small cell lung cancer patients treated with immune checkpoint inhibitors. Lung Cancer 2019;136:45-51. [Crossref] [PubMed]
- Ohba T, Takamori S, Toyozawa R, et al. Prognostic impact of the Controlling Nutritional Status score in patients with non-small cell lung cancer treated with pembrolizumab. J Thorac Dis 2019;11:3757-68. [Crossref] [PubMed]
- Leung EY, Scott HR, McMillan DC. Clinical utility of the pretreatment glasgow prognostic score in patients with advanced inoperable non-small cell lung cancer. J Thorac Oncol 2012;7:655-62. [Crossref] [PubMed]
- Jiang AG, Chen HL, Lu HY. The relationship between Glasgow Prognostic Score and serum tumor markers in patients with advanced non-small cell lung cancer. BMC Cancer 2015;15:386. [Crossref] [PubMed]
- Fujio T, Nakashima K, Naito T, et al. Platinum Combination Chemotherapy Is Poorly Tolerated in Malnourished Advanced Lung Cancer Patients with Poor Performance Status. Nutr Cancer 2019;71:767-71. [Crossref] [PubMed]


