
Inter-tumor heterogeneity of PD-L1 status: is it important in clinical decision making?
Introduction
Clinical applications for precision medicine with molecular-targeted drugs and immune checkpoint inhibitors have dramatically improved treatment outcomes for non-small cell lung cancer (NSCLC) patients. However, because precision medicine is precise, small genetic or transcriptional differences between cancer cells may affect the efficacies of these drugs. Therefore, studies on intra- and inter-tumor heterogeneity are important in the era of precision medicine (1), especially when spatial heterogeneity can bias the biomarker test results (2).
Programmed death-ligand 1 (PD-L1) protein expression, assessed via immunohistochemistry (IHC), is the only Food and Drug Administration (FDA)-approved biomarker for anti-PD-1 and anti-PD-L1 immune checkpoint inhibitor monotherapies for NSCLC. An IHC assay using the 22C3 antibody was approved as a companion diagnostic test for front-line pembrolizumab, and an assay using the 28-8 antibody was approved as a complementary diagnostic test for nivolumab. However, no solid evidence exists regarding which tumor tissues should be used (e.g., primary lung tumors, lymph node metastases, or distant lesions) for PD-L1 IHC testing to predict anti-PD-1 and anti-PD-L1 blockade efficacy. Current clinical practice allows use of any of these tissue specimens for PD-L1 IHC testing, which is reasonable because previous “practice-changing” phase III trials of anti-PD-1 and anti-PD-L1 agents did not restrict tissues for PD-L1 testing. For example, an analysis of the prevalence of PD-L1 expression in NSCLC patients screened for enrollment in the KEYNOTE-001, -010, and -024 trials found that 1,727 patients had their primary tumor tissues tested, and 1,281 had their metastatic samples tested. Of these patients, 437 (25%) who provided primary lung tumor tissues and 369 (29%) who provided metastatic samples had high PD-L1 expression, which is defined as a tumor proportion score (TPS) of ≥50% (3).
Non-negligible inter-tumor heterogeneity of PD-L1 expression status
In a study published in the Journal of Thoracic Disease in December 2019 (4), Saito and colleagues compared PD-L1 expression statuses detected via the 22C3 and 28-8 PharmDx assays between primary lung tumors and paired metastatic lymph nodes in 35 patients with surgically resected NSCLCs. The authors observed that the TPS categories (<1%, 1–49%, and ≥50%) were similarly distributed between the 22C3 and 28-8 antibodies in both primary lung tumors (concordance rate: 74%) and metastatic lymph nodes (concordance rate: 71%). This was expected because several harmonization studies for PD-L1 testing have shown that the 22C3 and 28-8 antibodies are interchangeable (5). The authors also found lower concordances of PD-L1 expression statuses between primary lung tumors and paired metastatic lymph nodes, at only 29% and 31% using the 22C3 and 28-8 PharmDx assays, respectively. Among samples with discordant results, PD-L1 status was higher in primary tumors in 51% (22C3) and 46% (28-8) of the cases, while it was higher in lymph node metastases in 20% (22C3) and 23% (28-8) of the cases. How should inter-tumor heterogeneity data on PD-L1 expression status be incorporated in daily clinical practice? Here, we discuss this point, referring to recent publications.
Molecular mechanisms regulating PD-L1 expression in tumor cells
Before discussing the inter-tumor heterogeneity of PD-L1 expression, we briefly summarize the molecular mechanisms that regulate PD-L1 expression in tumor cells. Tumor cells can express PD-L1 via three general mechanisms: constitutive PD-L1 expression, constitutive PD-L1 degradation, and adaptive PD-L1 expression.
Constitutive PD-L1 expression results from aberrant activation of oncogenic signaling pathway(s), such as the epidermal growth factor receptor (EGFR) (6), MYC (7), and ZEB1 (8) signaling pathway(s) or from PD-L1 gene amplification (9). Constitutive PD-L1 degradation was recently reported, with glycogen synthase kinase 3β (GSK3β) (10) and cyclin D-CDK4 (11) promoting proteasome-mediated PD-L1 degradation in tumor cells.
Inflammatory factors secreted in the tumor microenvironment induce adaptive PD-L1 expression during antitumoral immune responses. Interferon (IFN)-γ, an inflammatory cytokine secreted by cytotoxic T lymphocytes and natural killer cells, induces PD-L1 expression in tumor cells. An in vitro study reported that brief exposure to IFN-γ significantly enhanced PD-L1 expression in all 32 tumor cell lines tested (derived from NSCLCs, melanomas, renal-cell carcinomas, and head-and-neck squamous cell carcinomas) regardless of baseline constitutive PD-L1 expression (12). The same study also found that cytokines IL-1α and IL-27 independently enhanced or induced PD-L1 expression in some tumor cell lines, and further increased IFN-γ-induced PD-L1 expression in some cases, suggesting the complexity of adaptive PD-L1 expression mechanisms (12). These polyphyletic mechanisms of PD-L1 expression/degradation can cause a discrepancy in the PD-L1 expression status between tumor cells in primary lung tumors and those in metastatic lymph nodes.
Inter-tumor heterogeneity of PD-L1 status in previous studies
In addition to the current study (4), several research groups have evaluated inter-tumor heterogeneity in PD-L1 expression statuses between primary lung tumors and lymph node metastases (13-18). Notably, these studies used specimens from patients who underwent surgical resection, because both the primary tumor tissues and lymph node samples were available. Table 1 summarizes the major findings of these publications. Some results were inconsistent between studies, likely owing to differences in patients’ clinical backgrounds, differences in PD-L1 antibodies, cut-off values, conditions of the archived tissues, PD-L1 staining and evaluation qualities, and small sample sizes; however, a summary of these studies revealed some general trends.
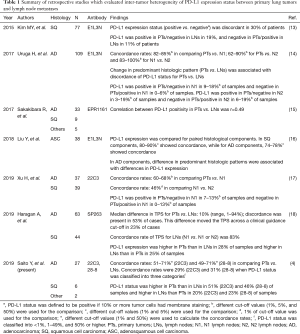
Full table
First, inter-tumor heterogeneity of PD-L1 expression status between primary lung tumors and lymph node metastases exists at frequencies of approximately 15–40%. In cases with positive inter-tumor heterogeneity, more patients showed negative conversion (i.e., the primary lung tumors were PD-L1-positive, but the lymph node metastases were PD-L1-negative), and fewer patients showed positive conversion (i.e., the primary lung tumors were PD-L1-negative, but the lymph node metastases were PD-L1-positive). Some studies also evaluated inter-tumor heterogeneity between lymph node metastases from different locations (e.g., N1 vs. N2) (14,17,18), suggesting higher concordance rates between different lymph nodes than between primary lung tumors and lymph node metastases.
Second, histology may affect the concordance rates of PD-L1 status between primary lung tumors and lymph node metastases. Squamous cell carcinomas may have higher concordances than those of adenocarcinomas, partially owing to discrepancies among predominant histologic subtypes of lung adenocarcinomas (19), which affect PD-L1 expression statuses (20) between primary lung tumors and lymph node metastases.
Inter-tumor heterogeneity between primary lung tumors and lymph node metastases has also been reported for other immune checkpoints. One study assessed the inter-tumor heterogeneity of PD-L2 expression status (13). The concordance rate of PD-L2 expression between primary lung tumors and lymph node metastases was 62%. PD-L2 expression was upregulated in 31% and downregulated in 7% of lymph node metastases compared with primary lung tumors. A subgroup analysis of 142 NSCLC patients with surgically resected lymph node metastases compared cytotoxic T-lymphocyte-associated antigen-4 (CTLA-4) expression statuses of tumor cells between primary lung tumors and lymph node metastases (21) and found that they were not significantly correlated. In 56% of the cases, IHC scores were concordantly high or low in both samples. In 23% of the cases, primary tumors scores were high, and lymph node scores were low, whereas 21% of the cases showed the opposite trend.
These studies used tissue specimens from NSCLC patients who underwent surgical resection. However, data on inter-tumor heterogeneity are especially important in patients with advanced-stage disease because these patients are candidates for immune checkpoint inhibitors. Because multiple biopsy samples are difficult to obtain from advanced-stage NSCLC patients, few data are available regarding inter-tumor heterogeneity of the PD-L1 expression status in advanced-stage NSCLC patients. Our previous study, which analyzed five autopsied patients with treatment-naïve lung cancer, showed that inter-tumor heterogeneity of PD-L1 and the tumor mutation burden (1) as well as other immune checkpoint molecules (22) also existed in advanced-stage NSCLC. We also found that immune-related pathways were downregulated in metastatic lesions (including lymph node metastases) compared with primary lesions (1).
Is inter-tumor heterogeneity of PD-L1 status clinically relevant?
The studies summarized in Table 1 show that inter-tumor heterogeneity of PD-L1 status occurs frequently between primary lung tumors and lymph node metastases. Thus, should inter-tumor heterogeneity be considered when treating NSCLC patients? Currently, as described above, both primary lung tumors and metastatic lesions are used for PD-L1 testing in clinical practice.
First, whether PD-L1 status in both primary lung tumors and metastatic lesions can predict the efficacy of anti-PD-1 and anti-PD-L1 blockade must be determined. A recent retrospective study by Schoenfeld and colleagues may answer this (23). Their analysis of progression-free survival (PFS) among patients receiving anti-PD-1 and anti-PD-L1 inhibitors compared high-PD-L1 patients (≥50%) and PD-L1-negative patients (<1%) by anatomic site where the biopsy was taken for testing. When PD-L1 testing was performed using tissue samples from primary lung tumors [hazard ratio (HR): 0.56, 95% confidential interval (CI): 0.43–0.74, P<0.01, n=190] or distant metastases (HR: 0.48, 95% CI: 0.31–0.73, P<0.01, n=110), high PD-L1 status was significantly correlated with longer PFS. The difference in PFS was marginally significant when PD-L1 expression status of lymph node metastasis was used (HR: 0.63, 95% CI: 0.38–1.04, P=0.05, n=61). These results support the current clinical practice of using both primary lung tumors and metastatic lesions for PD-L1 testing. However, it is unclear whether anti-PD-1 and anti-PD-L1 blockade will be effective when the first biopsy is PD-L1-negative and the second biopsy from a different tumor location has high PD-L1 expression.
Second, whether the PD-L1 status of each metastatic site is correlated with anti-PD-1 and anti-PD-L1 blockade response in each metastatic lesion must be determined. Although this is difficult to determine, the study by Schoenfeld and colleagues (23) may also help answer this. The authors summarized PD-L1 expression status by anatomic site of the biopsy. The frequencies of high PD-L1 expression were higher in liver (23%, n=61) and pleural (18%, n=72) metastases than in lung tumors (13%, n=1,124). Conversely, several retrospective studies found that liver (24-26) and pleural (27,28) metastases were significantly correlated with poorer patient outcomes after anti-PD-1 and anti-PD-L1 blockade. These results suggest that PD-L1 status at each metastatic site is not strongly correlated with clinical response to anti-PD-1 and anti-PD-L1 blockade in each metastatic lesion.
Future perspectives and conclusions
PD-L1 expression is an imperfect predictive biomarker of anti-PD-1 and anti-PD-L1 blockade for treating NSCLCs. As discussed herein, the inter-tumor heterogeneity of PD-L1 expression makes evaluating the predictive roles of PD-L1 IHC testing difficult. The inter-tumor heterogeneity of PD-L1 expression also highlights the complexity of immuno-oncology. Identifying a clonal expression biomarker (2) or liquid-based biomarker that can represent an NSCLC patient’s entire immuno-oncological status will help predict anti-PD-1 and anti-PD-L1 blockade efficacy.
Acknowledgments
We thank Traci Raley, MS, ELS, from Edanz Group (www.edanzediting.com/ac) for editing a draft of this manuscript.
Funding: This work was supported by a grant from the Uehara Memorial Foundation to K Suda.
Footnote
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jtd-20-1661). KS reports grants and personal fees from Boehringer Ingelheim, personal fees from AstraZeneca, grants from Rain Therapeutics, outside the submitted work; TM reports grants and personal fees from Boehringer Ingelheim, personal fees from AstraZeneca, grants and personal fees from Pfizer Japan Inc., grants and personal fees from Chugai Pharmaceutical Co. Ltd., personal fees from MSD K. K., grants and personal fees from Ono Pharmaceutical Co. Ltd., personal fees from Bristol Myers Squibb, personal fees from Eli Lilly Japan K. K., grants and personal fees from Taiho Pharmaceutical Co. Ltd., outside the submitted work.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Suda K, Kim J, Murakami I, et al. Innate Genetic Evolution of Lung Cancers and Spatial Heterogeneity: Analysis of Treatment-Naive Lesions. J Thorac Oncol 2018;13:1496-507. [Crossref] [PubMed]
- Biswas D, Birkbak NJ, Rosenthal R, et al. A clonal expression biomarker associates with lung cancer mortality. Nat Med 2019;25:1540-8. [Crossref] [PubMed]
- Aggarwal C, Rodriguez Abreu D, Felip E, et al. 1060P – Prevalence of PD-L1 expression in patients with non-small cell lung cancer screened for enrollment in KEYNOTE-001, -010, and -024. Presented at ESMO 2016, 2016.
- Saito Y, Horiuchi S, Morooka H, et al. Inter-tumor heterogeneity of PD-L1 expression in non-small cell lung cancer. J Thorac Dis 2019;11:4982-91. [Crossref] [PubMed]
- Tsao MS, Kerr KM, Kockx M, et al. PD-L1 Immunohistochemistry Comparability Study in Real-Life Clinical Samples: Results of Blueprint Phase 2 Project. J Thorac Oncol 2018;13:1302-11. [Crossref] [PubMed]
- Suda K, Rozeboom L, Furugaki K, et al. Increased EGFR Phosphorylation Correlates with Higher Programmed Death Ligand-1 Expression: Analysis of TKI-Resistant Lung Cancer Cell Lines. Biomed Res Int 2017;2017:7694202.
- Casey SC, Tong L, Li Y, et al. MYC regulates the antitumor immune response through CD47 and PD-L1. Science 2016;352:227-31. [Crossref] [PubMed]
- Chen L, Gibbons DL, Goswami S, et al. Metastasis is regulated via microRNA-200/ZEB1 axis control of tumour cell PD-L1 expression and intratumoral immunosuppression. Nat Commun 2014;5:5241. [Crossref] [PubMed]
- Ikeda S, Okamoto T, Okano S, et al. PD-L1 Is Upregulated by Simultaneous Amplification of the PD-L1 and JAK2 Genes in Non-Small Cell Lung Cancer. J Thorac Oncol 2016;11:62-71. [Crossref] [PubMed]
- Li CW, Lim SO, Xia W, et al. Glycosylation and stabilization of programmed death ligand-1 suppresses T-cell activity. Nat Commun 2016;7:12632. [Crossref] [PubMed]
- Zhang J, Bu X, Wang H, et al. Cyclin D-CDK4 kinase destabilizes PD-L1 via cullin 3-SPOP to control cancer immune surveillance. Nature 2018;553:91-5. [Crossref] [PubMed]
- Chen S, Crabill GA, Pritchard TS, et al. Mechanisms regulating PD-L1 expression on tumor and immune cells. J Immunother Cancer 2019;7:305. [Crossref] [PubMed]
- Kim MY, Koh J, Kim S, et al. Clinicopathological analysis of PD-L1 and PD-L2 expression in pulmonary squamous cell carcinoma: Comparison with tumor-infiltrating T cells and the status of oncogenic drivers. Lung Cancer 2015;88:24-33. [Crossref] [PubMed]
- Uruga H, Bozkurtlar E, Huynh TG, et al. Programmed Cell Death Ligand (PD-L1) Expression in Stage II and III Lung Adenocarcinomas and Nodal Metastases. J Thorac Oncol 2017;12:458-66. [Crossref] [PubMed]
- Sakakibara R, Inamura K, Tambo Y, et al. EBUS-TBNA as a Promising Method for the Evaluation of Tumor PD-L1 Expression in Lung Cancer. Clin Lung Cancer 2017;18:527-534.e1. [Crossref] [PubMed]
- Liu Y, Dong Z, Jiang T, et al. Heterogeneity of PD-L1 Expression Among the Different Histological Components and Metastatic Lymph Nodes in Patients With Resected Lung Adenosquamous Carcinoma. Clin Lung Cancer 2018;19:e421-e430. [Crossref] [PubMed]
- Xu H, Chen X, Lin D, et al. Conformance Assessment of PD-L1 Expression Between Primary Tumour and Nodal Metastases in Non-Small-Cell Lung Cancer. Onco Targets Ther 2019;12:11541-7. [Crossref] [PubMed]
- Haragan A, Field JK, Davies MPA, et al. Heterogeneity of PD-L1 expression in non-small cell lung cancer: Implications for specimen sampling in predicting treatment response. Lung Cancer 2019;134:79-84. [Crossref] [PubMed]
- Suda K, Sato K, Shimizu S, et al. Prognostic implication of predominant histologic subtypes of lymph node metastases in surgically resected lung adenocarcinoma. Biomed Res Int 2014;2014:645681.
- Miyazawa T, Marushima H, Saji H, et al. PD-L1 Expression in Non-Small-Cell Lung Cancer Including Various Adenocarcinoma Subtypes. Ann Thorac Cardiovasc Surg 2019;25:1-9. [Crossref] [PubMed]
- Paulsen EE, Kilvaer TK, Rakaee M, et al. CTLA-4 expression in the non-small cell lung cancer patient tumor microenvironment: diverging prognostic impact in primary tumors and lymph node metastases. Cancer Immunol Immunother 2017;66:1449-61. [Crossref] [PubMed]
- Suda K, Kim J, Murakami I, et al. P2.04-15 Heterogeneity and Correlation Between Immune Markers in Lung Cancers: Analysis of Treatment-Naïve Lesions. J Thorac Oncol 2018;13:S736. [Crossref]
- Schoenfeld AJ, Rizvi H, Bandlamudi C, et al. Clinical and molecular correlates of PD-L1 expression in patients with lung adenocarcinomas. Ann Oncol 2020;31:599-608. [Crossref] [PubMed]
- Funazo T, Nomizo T, Kim YH. Liver Metastasis Is Associated with Poor Progression-Free Survival in Patients with Non-Small Cell Lung Cancer Treated with Nivolumab. J Thorac Oncol 2017;12:e140-1. [Crossref] [PubMed]
- Schmid S, Diem S, Li Q, et al. Organ-specific response to nivolumab in patients with non-small cell lung cancer (NSCLC). Cancer Immunol Immunother 2018;67:1825-32. [Crossref] [PubMed]
- Tamiya M, Tamiya A, Inoue T, et al. Metastatic site as a predictor of nivolumab efficacy in patients with advanced non-small cell lung cancer: A retrospective multicenter trial. PLoS One 2018;13:e0192227. [Crossref] [PubMed]
- Shibaki R, Murakami S, Shinno Y, et al. Malignant pleural effusion as a predictor of the efficacy of anti-PD-1 antibody in patients with non-small cell lung cancer. Thorac Cancer 2019;10:815-22. [Crossref] [PubMed]
- Kawachi H, Tamiya M, Tamiya A, et al. Association between metastatic sites and first-line pembrolizumab treatment outcome for advanced non-small cell lung cancer with high PD-L1 expression: a retrospective multicenter cohort study. Invest New Drugs 2020;38:211-8. [Crossref] [PubMed]


