Acetazolamide use in severe COPD exacerbations requiring invasive mechanical ventilation: impact on duration of mechanical ventilation
We read with interest the article titled “Effect of Acetazolamide vs. Placebo on Duration of Invasive Mechanical Ventilation Among Patients With Chronic Obstructive Pulmonary Disease: A Randomized Clinical Trial” by Faisy et al. (1) where the authors have and colleagues randomly assigned patients with chronic obstructive pulmonary disease (COPD) who required invasive mechanical ventilation to receive either acetazolamide 500 mg intravenously twice daily (1,000 mg if loop diuretics were also prescribed) or matching placebo up to 28 days. A total of 382 patients with COPD who were expected to receive mechanical ventilation for more than 24 hours to acetazolamide (500–1,000 mg, twice daily) or placebo, administered intravenously in cases of pure or mixed metabolic alkalosis. The main results were: among 382 randomized patients, 380 [mean age, 69 years; 272 men (71.6%); 379 (99.7%) with endotracheal intubation] completed the study. For the acetazolamide group (n=187), compared with the placebo group (n=193), no significant between-group differences were found for median duration of mechanical ventilation (–16.0 hours; 95% CI, –36.5 to 4.0 hours; P=0.17). For secondary outcomes, there is no difference in duration of weaning off mechanical ventilation (–0.9 hours; 95% CI, –4.3 to 1.3 hours; P=0.36), in changes of minute-ventilation (–0.0 L/min; 95% CI, –0.2 to 0.2 L/min; P=0.72), or partial carbon-dioxide pressure in arterial blood (–0.3 mmHg; 95% CI, –0.8 to 0.2 mmHg; P=0.25). However, the authors observed a significant daily changes of serum bicarbonate (between-group difference, –0.8 mEq/L; 95% CI, –1.2 to –0.5 mEq/L; P<0.001), in the number of days with metabolic alkalosis (between-group difference, –1 days; 95% CI, –2 to –1 days; P<0.001) and significantly increased in the PaO2:FIO2 ratio in the acetazolamide group’s. Other secondary outcomes also did not differ significantly between groups.
The authors concluded that among patients with COPD receiving invasive mechanical ventilation, the use of acetazolamide, compared with placebo, did not result in a statistically significant reduction in the duration of invasive mechanical ventilation.
Several hypotheses can be advanced to explain the inefficacy of acetazolamide to shorten the duration of mechanical ventilation in this study.
First, this inefficacy may be related to pharmacokinetic reasons. In fact, there are several isoforms of human carbonic anhydrase, and some may be more inhibited than others by ACET, which may complicate the reversal of metabolic alkalosis (2-4).
Second, several factors as serum chloride level and co-administration of furosemide or systemic steroid can interfere with ACET pharmacokinetics (5). Despite that in the study performed by Faisy et al. (1), co-treatments with loop diuretics, glucocorticoids, β2-agonists or catecholamines, were used in the same proportion in the two groups, theses therapeutics can interfere with ACET pharmacokinetics and decrease ACET effectiveness.
Third, the optimal dosage of acetazolamide to be administered to alkalotic COPD patients is unclear. The results of a recent study (6) suggest that higher doses of acetazolamide (>1,000 mg daily) are necessary to induce a substantial increase in minute ventilation and hence a decrease in PaCO2 in alkalotic mechanically ventilated COPD patients. Moreover, this last study (6) suggests that the increase in minute ventilation following the administration of acetazolamide is obtained at the price of an increase in respiratory rate rather than tidal volume, whatever the ventilatory mode.
Fourth, a limitation of Faisy et al. (1) study is the presence of mixed metabolic alkalosis in most patients. In fact, the lack of acetazolamide respiratory effect may be due to the fact that many of the patients had a degree of metabolic alkalosis too mild for the intervention.
Fifth, although the two groups included in this study (1) have the same respiratory characteristics with the same forced expiratory volume in the first second of expiration (FEV1) and the same forced vital capacity (FVC), the poor mechanic capacities in severely flow-limited COPD patients may explain why the reversal of the depressive metabolic stimulus of the respiratory drive did not induce an increase in minute ventilation and thus, did not make weaning from ventilator support easier (4).
Sixth, the ACET induces a metabolic acidosis which stimulates the respiratory neural-driving leading to a hyperventilation with polypnea. This polypnea will significantly increase the workload of respiratory muscles and shortens the time of the respiratory cycle with its two components inspiratory and expiratory. As consequence, respiratory and/or limb muscle dysfunction, which are frequently observed in COPD patients will be increased by ACET prescription.
Seventh, as detailed by authors (1) the study may have identified a clinically important benefit of acetazolamide for the primary end point that did not demonstrate statistical significance because of a possible lack of power. In fact, the lack of statistical significance may be due to an underpowered study because of fewer-than-expected patients who received the treatment (more than 20% of patients in each group did not receive the assigned treatment because of lack of metabolic alkalosis or temporary contraindications. Moreover, despite it did not the reach statistical significance, the difference between-group in median durations of invasive mechanical ventilation was clinically considerable (16 hours). In fact, this last trial was prospectively powered to detect a 15% difference in the invasive ventilation duration, considered clinically relevant in light of the usual duration of intubation in these patients. However, the observed median durations of invasive mechanical ventilation in the placebo and acetazolamide groups were lower than anticipated for statistical power, complicating the study interpretation. This means that the 10% reduction of invasive mechanical ventilation by acetazolamide could have reached statistical significance if the study was designed to detect such a difference.
Finally, we found that this recent study, confirms the results of two retrospective, case-control studies (4,7) published on the same subject. The first study was published on 2010 (7), in this study, 26 intubated COPD patients with mixed metabolic alkalosis were compared with a historical control group (n=26) matched for serum bicarbonate, arterial pH, age, and severity of illness at admission to ICU. ACET administration (500 mg intravenously) was monitored daily according to arterial blood gas analysis from readiness to wean until extubation. The main results of this study were Patients with ACET treatment significantly decreased their serum bicarbonate (P=0.01) and arterial blood pH (P<0.0001), increased their PaO2/FiO2 ratio (P=0.04), but did not change their PaCO2 (P=0.71). Compared with matched controls, administration of ACET did not improve arterial blood gas and respiratory parameters except PaO2/FiO2 ratio (P=0.03). The use of acetazolamide, compared with placebo, did not result in a statistically significant reduction in the duration of invasive mechanical ventilation. Moreover, extubation success rate was not significantly different between groups, and causes of reintubation were comparable.
The second study was more recently published (on 2015) (4). It is Retrospective pair-wise, case-control study with 1:1 matching. Patients were defined as cases when they had received acetazolamide (500 mg per day) and as controls when they did not received it. Patients were matched according to age, severity on admission (pH, PaO2/FiO2 ratio) and SAPSII score. This study included 72 patients equally distributed between the two studied groups. There were no differences between baseline characteristics of the two groups. Concomitant drugs used were also not significantly different between two groups.
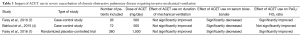
The main results of this study were mean duration of mechanical ventilation was not significantly different between ACET(+) and ACET(–) patients (10.6±7.8 and 9.6±7.6 days, respectively; P=0.61). The use of ACET was associated with a significantly decreased serum bicarbonate, arterial blood pH, and PaCO2 levels. Moreover, authors did not found any significant difference between the two studied groups in terms of ICU length of stay (LOS). ICU mortality was also comparable between ACET(+) and ACET(–) groups (38% and 52%, respectively; P=0.23). Table 1 summarizes the impact of ACET use in severe exacerbation of chronic obstructive pulmonary disease requiring invasive mechanical ventilation in all published studies (1,4,7).
Full table
In summary, we can conclude that in severe exacerbation of COPD requiring intensive care admission and invasive mechanical ventilation, metabolic alkalosis occurs frequently in this group of patients who frequently receive therapies for cardiac and respiratory failures (steroids, diuretics, etc.). This disorder may depress central respiratory drive leading to hypoventilation and thus, hampers the weaning process. Despite that Acetazolamide, is used to reverse metabolic alkalosis after proper fluid loading and potassium supplementation, all published results of ACET in this specific condition suggests that systemic ACET therapy in this specific condition is not helpful to reduce the duration of mechanical ventilation and to make the weaning process easier (1,4,7). However, it is possible that the use of ACET can be efficient in a subgroup of patients. Thus, further studies are needed to evaluate the effect of ACET on ventilator weaning process in critically ill COPD patients requiring mechanical ventilation.
Acknowledgements
None.
Footnote
Provenance: This is an invited Editorial commissioned by the Section Editor Zhongheng Zhang (Department of Critical Care Medicine, Jinhua Municipal Central Hospital, Jinhua Hospital of Zhejiang University, Jinhua, China).
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Faisy C, Meziani F, Planquette B, et al. Effect of Acetazolamide vs Placebo on Duration of Invasive Mechanical Ventilation Among Patients With Chronic Obstructive Pulmonary Disease: A Randomized Clinical Trial. JAMA 2016;315:480-8. [Crossref] [PubMed]
- Alp C, Özsoy Ş, Alp NA, et al. Sulfapyridine-like benzenesulfonamide derivatives as inhibitors of carbonic anhydrase isoenzymes I, II and VI. J Enzyme Inhib Med Chem 2012;27:818-24. [Crossref] [PubMed]
- Gomolin IH, Chapron DJ. Elucidating the relationship between acetazolamide plasma protein binding and renal clearance using an albumin infusion. J Clin Pharmacol 1992;32:1028-32. [Crossref] [PubMed]
- Bahloul M, Chaari A, Tounsi A, et al. Impact of acetazolamide use in severe exacerbation of chronic obstructive pulmonary disease requiring invasive mechanical ventilation. Int J Crit Illn Inj Sci 2015;5:3-8. [Crossref] [PubMed]
- Heming N, Faisy C, Urien S. Population pharmacodynamic model of bicarbonate response to acetazolamide in mechanically ventilated chronic obstructive pulmonary disease patients. Crit Care 2011;15:R213. [Crossref] [PubMed]
- Heming N, Urien S, Fulda V, et al. Population pharmacodynamic modeling and simulation of the respiratory effect of acetazolamide in decompensated COPD patients. PLoS One 2014;9:e86313. [Crossref] [PubMed]
- Faisy C, Mokline A, Sanchez O, et al. Effectiveness of acetazolamide for reversal of metabolic alkalosis in weaning COPD patients from mechanical ventilation. Intensive Care Med 2010;36:859-63. [Crossref] [PubMed]


