Report of the 2016–2017 ESTS-AME visiting fellow to the First Affiliated Hospital of Guangzhou University, China
I started my visiting fellowship at the First Affiliated Hospital of Guangzhou University in China by arriving at Guangzhou airport on a cool crisp December evening. After meeting Lucille, a liaison from AME publishing company who became my guide and close friend throughout the trip, we made our way to the heart of the city that night which was vibrant and bustling. After an authentic Chinese meal overlooking the Pearl River that runs through the city center it was time to rest up for a busy week at the hospital.
The next morning, after meeting Lucille, we made our way to the thoracic surgery ward which spans three floors. We were greeted with a warm reception from Dr. He (Chief of thoracic surgery) and were introduced to his large team of co-attendings, residents, fellows and nursing staff after which ward rounds were started (Figures 1,2). The hospital rooms offer patients with stunning views of the city and I was fortunate to be provided with constant translation to understand the interaction which was switching between Cantonese and Mandarin. We discussed each patient’s case in addition to North American management styles around issues such as chest tube management, enhanced recovery protocols and discharge patterns.

The late morning was spent reviewing imaging and planning surgical management for several cases with a multi-disciplinary team. Interesting discussions revolved around complex cases including large mediastinal masses and difficult superior sulcus tumors.
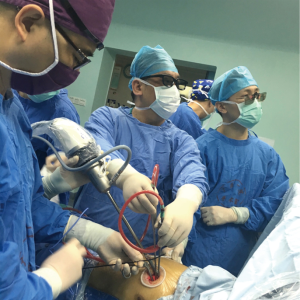
I spent the afternoon in the operating room where thoracic surgery runs around four operating theaters everyday with almost all cases approached in a minimally invasive manner. The institution is most reputed for mediastinal and lung cases with esophageal cases being concentrated at another hospital. Interestingly, Dr. He and the group almost exclusively prefer uniportal approaches for their cases and employ the 3D laparoscopic vision which does not require the surgeon to wear glasses but instead a comfortable headband (Figure 3). In their experience, the 3D view greatly facilitates dissection through a uniportal approach and the division has embraced this technology for several years now (1).
By the end of my first day which was busy and productive I was well integrated into thoracic surgery team with great insight into the thoracic surgery department. As I walked back with Lucille I learnt more about the Chinese health system, health policy and access to services for the people.
My next few days continued with morning ward rounds, thought provoking discussion of interesting cases with significant time spent in the operating room. I was impressed with the efficiency of the operative room (OR) staff (including prompt turnover times) and of course the proficiency of the surgeons with uniportal procedures even for challenging lung resections. One of the highlights of my trip was an excellent talk by Dr. He over delicious Chinese tea on cases such as uniportal double sleeve (bronchial and pulmonary artery plasty) and video-assisted thoracoscopic surgery (VATS) tracheal resection and reconstruction (2) (Figure 4). Of particular interest was Dr. He’s achievement with VATS resection of tracheal masses under spontaneous breathing and airway management with only a laryngeal mask (3). In their experience the team has found, spontaneous breathing surgery to be safe, feasible and efficient with possibly faster recovery times and better postoperative lung function for airway and lung operations (4,5).
Towards the end of my visit, I had the privilege of presenting grand rounds on the evolving paradigm of cardiothoracic surgery training in North America (Figure 5). During my time at Guangzhou I had the opportunity to interact with several residents in various stages of training and it was interesting to note the similarities in the challenges of surgical training including longer training times (due to the need for multiple fellowships). The presentation provided a platform to discuss strategies to overcome these issues including the growth of simulation training, competency-based education and novel models of instruction and assessment. I enjoyed interacting with the keen medical students, bright residents and accomplished attendings. After spending the morning in the OR, the discussion continued over an elaborate lunch hosted by Dr. He on the ward (Figure 6).
No trip to Guangzhou or Flower city as it is called (due to literally endless arrangements of perfectly manicured flowers flooding the city) without experiencing its rich history, culture and culinary delights. I spent my last day touring the city with Lucille who planned our itinerary to experience Guangzhou in its most authentic way. We visited ancient Buddhist temples that house 300-year-old Banyan trees and then made our way to Lychee park using the bike share which is ubiquitous throughout the city. We ended the day by watching a truly moving opera performance in the park, a routine cultural activity for the people of Guangzhou (Figure 7).

Before leaving Guangzhou, I thanked the AME staff, Dr. He and the entire team at the hospital for their warm hospitality and a truly enjoyable learning experience (Figure 8). I have made good friends and great colleagues over this trip and we hope to continue this experience with ongoing research collaborations.
Acknowledgements
Dr. Cassivi (Mayo Clinic) was our team leader and I thank him for this exciting opportunity in addition to my excellent team mates during the competition Dr. John Agzarian (Thoracic Surgery, McMaster University, Canada) and Dr. Simon Turner (Thoracic Surgery, Edmonton, Canada).
Organizing such as trip during a busy cardiothoracic surgery fellowship would not have been possible without my program director’s (Dr. Robert Shen, Mayo Clinic) and program coordinator’s (Ms. Carla Maclean) incredible support.
The entire group at AME Publishing in particular Lucille and Grace who arranged this travelling fellowship with meticulous detail ensuring the trip was enjoyable and academically rewarding.
Footnote
Conflicts of Interest: The author has no conflicts of interest to declare.
References
- He J, Ang KL, Hao Z, et al. The comparison between novel and traditional three-dimensional image system in thoracoscopy: glasses-less vs. glass. J Thorac Dis 2016;8:3075-80. [Crossref] [PubMed]
- He J, Wang W, Li J, et al. Video-assisted thoracoscopic surgery tracheal resection and carinal reconstruction for tracheal adenoid cystic carcinoma. J Thorac Dis 2016;8:198-203. [PubMed]
- Li S, Liu J, He J, et al. Video-assisted transthoracic surgery resection of a tracheal mass and reconstruction of trachea under non-intubated anesthesia with spontaneous breathing. J Thorac Dis 2016;8:575-85. [Crossref] [PubMed]
- Li J, Liu H, Liu J, et al. Challenges in complex video-assisted thoracoscopic surgery and spontaneous respiration video-assisted thoracoscopic surgery procedures. J Vis Surg 2017;3:31. [Crossref] [PubMed]
- Zheng H, Hu XF, Jiang GN, et al. Nonintubated-Awake Anesthesia for Uniportal Video-Assisted Thoracic Surgery Procedures. Thorac Surg Clin 2017;27:399-406. [Crossref] [PubMed]