Chest wall stabilization with rib plating after cardiopulmonary resuscitation
Introduction
Rib fractures are common injuries sustained after chest compressions during cardiopulmonary resuscitation (CPR) for cardiac arrest (1). Chest wall instability secondary to these fractures can complicate management, especially in an already physiologically fragile patient. It is well known that rib fractures can significantly impair respiratory mechanics, alter cardiopulmonary physiology, and hinder mechanical ventilation weaning strategies (2). Chest wall instability can negatively impact the overall clinical outcomes and rehabilitation trajectories of patients with rib fractures after CPR.
Historically, rib fractures and chest wall instability have been managed conservatively with analgesia, pulmonary toilet and supplemental oxygen delivery. With the advent of surgical stabilization of rib fractures (SSRF) as a viable treatment strategy, the rib fracture management paradigm is shifting. Rib fractures and chest wall instability secondary to thoracic trauma are now being managed more aggressively with chest wall stabilization and rib fixation with promising results (3,4) and it is arguable that a recovery benefit may exist if SSRF were applied to the subset of post-CPR chest injury patients. No standardized guidelines have been developed for management of fractures that occur secondary to CPR, and to the author’s knowledge, only one other reported case details the application of SSRF as a management method (5). We report the case of rib fractures after CPR and discuss the utility of chest wall stabilization with rib plating following cardiopulmonary arrest and associated chest wall instability.
Case presentation
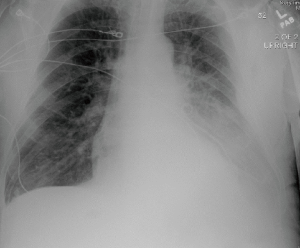
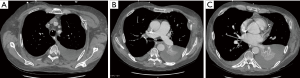
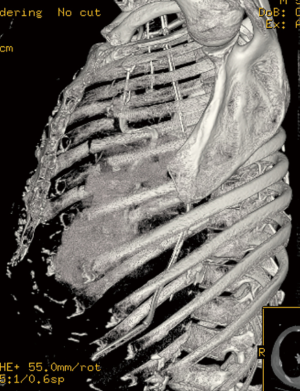
A 59-year-old male suffered a witnessed cardiac arrest by Emergency Medical Services after demonstrating altered mental status and seizure like activity. The patient was intubated and underwent CPR including chest compressions and return of spontaneous circulation was achieved. The patient was admitted to our facility, managed by the medical intensive care unit team and was unable to be weaned from the ventilator. On hospital day number 17, consideration was given to the patient’s notably displaced left sided rib fractures as a contributing factor to the patient’s ventilator weaning difficulties. Surgical consultation was obtained and the patient’s chest radiograph and computed tomography scan of the chest were reviewed (Figures 1,2). 3D reconstructions of the CT chest were obtained to assist with operative planning (Figure 3). The patient was taken to the operating room for chest wall stabilization and rib fixation.
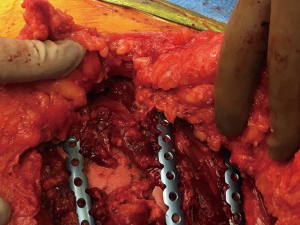
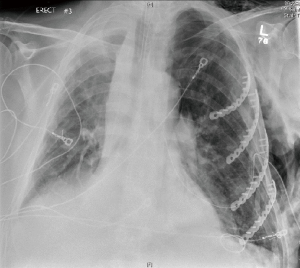
In the operating room, the patient was positioned in the right lateral decubitus position. A vertical incision at the anterior axillary line of the left chest was made over the palpable fractures. The pectoralis major muscle was split in a muscle sparing fashion to allow access to the more cephalad fractures. The chest wall was inspected and a disruption of the intercostal space at the level of the 5th and 6 ribs was noted. The defect was accessed to evacuate a small, retained hemothorax. The left sided fractured ribs 3, 4, 5, and 6th were reduced and fixated using the Synthes MatrixRIB® Fixation System (DePuy Synthes, West Chest, PA 19380, USA). Left sided, pre-contoured plates were applied to all four ribs with 10-mm locking screws for bicortical fixation (Figure 4). The intercostal defect was closed primarily with intercostal muscle approximation using 2-0 Vicryl sutures. A 19 Fr Blake Drain was positioned into the pleural space and placed to continuous suction. The pectoralis major was re-approximated with 2-0 Vicryl suture to cover the plates. An additional 2-0 Vicryl was used to close the dermis and skin was closed with staples. A post-operative chest radiograph revealed clearing of the left lung field and improved left lung expansion (Figure 5).
Post-operatively the patient underwent percutaneous tracheostomy on post arrest day #23 (POD #7). The patient was weaned to aerosolized tracheostomy collar and transferred to a rehabilitation center on post arrest day #32 (POD #16). The patient was seen one month after discharge from the hospital. He had been cleared from his rehabilitation facility with no need for supplemental respiratory support and was functioning near his baseline status.
Discussion
Rib fractures, sternal fractures, and flail chest occur commonly as a result of chest compressions during CPR. CPR associated chest wall Injuries have increased in frequency over the last several decades, a trend potentially attributable to a change in CPR guidelines which now recommends an increase in the depth and rate of chest compression for the resuscitation of an arresting patient. In a forensic autopsy study of patients who underwent CPR before death, it was found that rib fractures occurred in 77% of males and 85% of females (1).
Patients who suffer cardiopulmonary arrest usually have preexisting cardiac and respiratory deficiencies that are exacerbated by cardiac arrest and further strained by their newly acquired chest wall instability. It is arguable that the CPR patient’s newly acquired chest wall injury, now coupled with their pre-existing medical comorbidities and their compromised cardiopulmonary performance, further disadvantages these patients’ recovery potential. The application of chest wall stabilization with rib fixation could help improve the already oppressed respiratory system performance in the post cardiac arrest patient. Chest wall stabilization has been shown to reduce pain, improve pulmonary mechanics, reduce mechanical ventilatory needs, and decrease known morbidities of rib fractures that include pneumonia and pleural effusions. By providing chest wall stabilization to an already fragile patient, we believe this intervention could help improve overall outcomes, weaning from mechanical ventilation, and rehabilitation disposition.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
References
- Kralj E, Podbregar M, Kejzar N, et al. Frequency and number of resuscitation related rib and sternal fractures are higher than generally considered. Resuscitation 2015;93:136-41. [Crossref] [PubMed]
- Ziegler DW, Agarwal NN. The morbidity and mortality of rib fractures. J Trauma 1994;37:975-79. [Crossref] [PubMed]
- Marasco SF, Davies AR, Cooper J, et al. Prospective Randomized Controlled Trial of Operative Rib Fixation in Traumatic Flail Chest. J Am Coll Surg 2013;216:924-32. [Crossref] [PubMed]
- Pieracci FM, Lin Y, Rodil M, et al. A Prospective, Controlled Clinical Evaluation of Surgical Stabilization of Severe Rib Fractures. J Trauma Acute Care Surg 2016;80:187-94. [Crossref] [PubMed]
- Ananiadou O, Karaiskos T, Givissi P, et al. Operative Stabilization of skeletal chest injuries secondary to cardiopulmonary resuscitation in cardiac surgical patient. Interact Cardiovasc Thorac Surg 2010;10:478-80. [Crossref] [PubMed]