
How to prepare for academic leadership: scientific training curriculum
Introduction
Thoracic surgery has evolved into an independent discipline out of general surgery practice over the past decades. In discrimination from other surgical subspecializations, thoracic surgery covers a large field of different physiological questions (ventilation, perfusion, intrathoracic volumes, and pressures), many different pathologies—the field of oncology being a topic as stand-alone—as well as different anatomical units (lungs, airways, chest wall, hilar vessels, mediastinum, etc.). Furthermore, different technical approaches are involved from minimal invasive [robotic-assisted thoracoscopic surgery (RATS), video-assisted thoracoscopic surgery (VATS)] to maximal invasive procedures (transplantation, chest wall reconstruction, extended resection). The development of the field of thoracic surgery in these various aspects is attributed to the innovation driven by representatives of the community of thoracic surgeons being motivated to move this field forward by constant analysis and critical appraisal and review of current practice, and identification of new research approaches as the pool and generator of innovation. Besides the generation of new ideas, it is crucial to be able to realize and execute these research ideas. For this purpose, scientific skills are needed and currently not covered during the surgical training, and in contrast to the well-established syllabus of training for patient care and surgery, a definition of this curriculum is missing.
In the present overview, we will try to summarize important factors for an academic career, however, none of these recommendations are validated and to our opinion also not realistically to be applied uniquely in the whole world of thoracic surgery in terms of relevant geographical and institutional differences. We will not differentiate between clinical and basic or translational research, as to our opinion research evolves from one research field to another—as it is said “from bench to bedside” and “from bedside to bench”, and it is beautifully the role of the surgeon scientist to accompany new ideas throughout the different phases of development or go back for proof of concept.
Why academia
Medical research is important and is directed to improve health and benefit of the public and has the goal to make a change in your patient care.
Clinically active physician/surgeon scientists are in the optimal position to bring up relevant questions from clinical practice: “from bedside to bench”, because they have a clear understanding of important clinical issues, including being able to identify the need to answer a certain question but also to judge the practicability to perform a research project. Furthermore, the other way arounds surgeons can introduce new research insights deriving from the lab into clinical practice: “from bench to bedside”.
Another argument for an academic career is that leadership positions in hospitals are related to academic productivity, as are membership and leadership in many academic surgical societies. It has been demonstrated that residents who completed 2 years of research training were more likely to pursue an academic career than those who did not complete 2 years (53% vs. 22%) (1), and none of the residents who did not have research experience went on to pursue an academic surgical career. Furthermore, research and science offer an alternative aspect of continued education throughout the entire career.
How to get started
The first and very important step of academic training is the choice of institution for training. Select a program that has a clear and successful track record in training and positioning future surgeons for a successful academic career. This selection process considers as well the choice of a mentor, who is an important key factor for a successful academic career, and it might need more than one mentor throughout a career. It is well established that the relationship between academic success and mentorship is obvious, but still some young surgeons remain hesitant to seek mentorship (2-5). This should indeed not be the case and is needed and extremely helpful in an academic career. Once started in a program, identify interesting research questions and start looking for potential projects. Academia does not necessarily mean laboratory work. Basic research is important to better understand the clinical basis. There are plenty of opportunities in outcome research, quality and safety, education, engineering of health care delivery, and other fields. If not basic science research, clinical [setting up or contributing to a clinical database (local, national, international) or participate/design in a clinical trial] or translational research (setting up or contributing to a tumor and blood bank; “tissue is the issue”—surgeons are uniquely positioned to collaborate here with basic scientists) are very interesting approaches (Table 1). For the latter ones it is not mandatory to be positioned in a university environment. However, although pure bench science research is uncommon in the community setting, it is not impossible if there is a collaborative effort with university scientists.

Full table
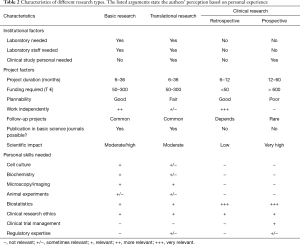
In any case, your research question stands at the beginning of the project. With support of your mentor who has eventually a wider overview, identify a “niche” or “knowledge gap” to address your research project. Another important factor at the beginning of your project is to assess your own skillset honestly, including as well your eventual deficiencies in order to identify areas where you need training, or collaboration with other research partners might be necessary. Scientific skills have to be learned to perform either type of research (Table 2). Specific research infrastructures are required to perform basic and translational research and multicentric clinical research, which in general are provided only by university hospitals. Many institutions offer methodology courses for research (statistics or good clinical practice courses) or attend courses offered by different societies, or even spend some time abroad to learn a special research technique (fellowships). To help, scientific societies like the European Society of Thoracic Surgeons (ESTS) have established several training modules to convey scientific key skills (8).
Full table
Protected research time
It might be necessary to have protected time for your research. It has been demonstrated, that 35% of residents who performed protected research time during their training successfully received independent research funding (9,10). In addition, protected research time has also a relevant impact on the publication track record which is the translation of your research outcome: Residents with research time get a mean of 7.4 original scientific publications and 4.0 first-author publications (9). Residents destined for academic surgery are also more productive publishing clinical papers than those who go into private practice (6.7 vs. 3.8, P=0.0035) (1) and last but not least, the number of publications correlates positively with the number of years spent in research (10,11). Institutional/departmental/divisional commitment exists in form of programs for early-career surgeon-scientists, at least 50% of the time, preferably for 2 years. Ask at your home university whether there are any programs for protected research time.
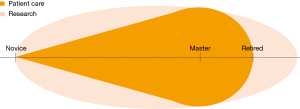
However, this extra time needs to be justified and organized in parallel to your at least equally if not more important surgical training. Even more important, at later stages, when you are establishing your career as a surgeon—always be available for your patient, your referring doctors and partners, always under motto: PATIENT First! (Figure 1). Depending on the structure of your department, there may be barriers to overcome for protected research time and therefore, obtaining funding is a central part, not only for the financial part of your research project.
Research funding
Overall, the general climate for obtaining successfully funding became very tight and frustrating over the past years. However, competing for research funding is a necessary part of a research career (5) and becomes an important criterion for your curriculum vitae (CV) later (Table 2). It might be discouraging how difficult it is nowadays to obtain funding, and also here your mentor will play a crucial role in advising which funding sources are realistic and available for you. It is helpful to diversify your efforts by applying for small and large grants simultaneously (5).
In general, you can differentiate between intra- and extramural funding. You can request to the hospital board for intramural funding, when you use your internal database of surgical patients for quality review and quality improvement purposes. Here, you can write a petition for support of the basic setup and data entry for your database, including technological considerations. Internal funding can also support the data manager and perhaps other research assistants (10). Also, some universities provide matching funds if there is a starter grant from extramural sources, which is not sufficient for financing a project.
Extramural funding can be obtained from government sources [Swiss National Science foundation (http://www.snf.ch/), Deutsche Forschungsgemeinschaft (https://www.dfg.de/); National Institutes of Health (NIH) (http://www.nih.gov/) and the Agency for Healthcare Research and Quality (http://www.ahrq.gov/)], supranational organizations like the European Union (European Research Council, https://erc.europa.eu/), or private foundations in your country. Furthermore, many organizations and societies have grants available for clinical research. Philanthropic donations from patients and their families are an additional potential funding source; however, the philanthropic spirit is not as developed in European countries as in the US. And last but not least, industry support, in particular for pharmacological trials are another option. To attract industry support, the performance and documentation of your program is very helpful.
Another strategy is to share research project costs across several specialties [so called full-time equivalents (FTEs) associated with the research effort], here it can be very helpful to collaborate with medical oncologists, radiation oncologists, general surgical oncologists, urologic oncologists to share service.
The whole writing process demands for many—partly in parallel-performed activities: besides the careful planning, solid data as a basis and budgeting is needed before you can submit the grant. Depending on the type of research and the experience of the applicant, grant applications can be prepared in collaboration of several professionals. Some societies offer courses for preparation: The American Association for Thoracic Surgery (AATS) sponsors a biennial Grant Writing Workshop in which the grant submission and review process of the NIH are discussed in detail. Strategies for optimizing each section of the grant (Hypothesis and Specific Aims, Significance, Innovation, Approach) as well as response to critique and rebuttal are discussed. Mock study sessions also provide the thoracic surgeon with insight into the actual discussion and grant review (10).
In general, medical writing is an important pillar for a young scientist’s career and here in particular also how to publish your research results. How to write a paper needs education and a learning process as well, a process, which will never end in your career lifetime.
Scientific medical writing
Publication of research results is the global measure used by all scientific disciplines to gauge a scientist’s level of success. Different fields have different conventions for writing style, and individual journals within a field usually have their own style guides (12). Original research articles are typically structured in the following order (13):
- Introduction—why was the study undertaken? What was the research question, the tested hypothesis or the purpose of the research?
- Methods—when, where, and how was the study done? What materials were used or who was included in the study groups (patients, etc.)?
- Results—what answer was found to the research question; what did the study find? Was the tested hypothesis true?
- Discussion—what might the answer imply and why does it matter? How does it fit in with what other researchers have found? What are the perspectives for future research?
The ESTS offers for several years already a successful course on medical writing (http://www.ests.org/education/medical_writing_course__hamburg_germany.aspx), and also some Universities offer locally courses on “How to write a paper”.
Research fellowships in training
Trainees in basic science and translational laboratories have to learn specific laboratory techniques; similarly, trainees in clinical research need to be educated in statistical analysis, clinical trial design and methodology, and database management. This fellowship time in early residency years provides the additional advantage of exposure in depth to the field of interest and might influence the direction of the future career. A survey of academic surgeons reported that 72% of those engaged in basic science research during their residency training selected their surgical specialty based on this experience (10,14). The ESTS Biology Club was introduced in 2011 and presents at the annual meeting since then a new scientific session format to bring together clinically relevant research questions and basic science. Since its introduction, 6 fellows were selected during the annual conference to spend a fellowship abroad from their home institution to bring back a research technique learnt at the host institution. Furthermore, the European Society of Medical Oncology (ESMO) Fellowship Program is a successful program since 30 years and also accepts surgeons for fellowships. In the US, there is a 2-year specific National Cancer Institute’s (NCI’s) Surgical Oncology Fellowship Program (15) for 6 months of clinical rotation followed by 18 months basic science and translational research (10). There are additional graduate education options for Clinical Research in form of master’s and even doctorate programs in clinical research, epidemiology, or public health; some degrees can even be completed online, either part time or full time. The syllabus usually comprises clinical trials and methodology, data management, biostatistics, ethics/research compliance, decision and cost-effectiveness analysis, grant writing, and epidemiology (10).
Clinical research opportunities
Clinical research is an optimal field for surgeons to participate in many roles. This can be by participation in multicenter (randomized) trials, as a role in designing a trial, or enrolling patients, or being involved in the analysis and evaluation of the trial. Participation in multicenter, national, or international registries can be another alternative to perform clinical research, such as submission of clinical data to the registries/databases of the ESTS or European Organization for Research and Treatment of Cancer (EORTC), or European Thoracic Oncology Platform (ETOP). The ESTS database comprises datasets from 243 contributing units throughout Europe for more than 10 years. It is the most current appraisal of the thoracic surgical activity in Europe, in the framework of a comprehensive, European-wide, population dataset; in particular for thymoma (1,344 registered cases from 75 centers), mesothelioma (2,216 registered cases from 63 centers) and data from the Neuroendocrine Thoracic Tumor (NETT) registry (1,450 registered cases). Last but not least, maintenance of an institutional database serving not only for quality control but also to generate research questions, is a very straightforward way of conducting clinical research. Out of this database, interesting research questions can be generated by retrospective studies, being equally interesting and definitively less expensive than prospective randomized trials (10,16).
Such a database project can be very easy to conduct by simply using spreadsheet programs or database management such as Microsoft Access (www.microsoft.com) or File-Maker Pro (www.filemaker.com). These desktop database management programs are relatively inexpensive and user friendly. With a minimal amount of training, these programs allow the creation of forms to input, edit, and display data. Queries can be performed to choose data to be displayed, and then, importantly, data stored in database management programs can be imported into most statistical analysis programs (10). Other options are SecuTrial® (https://www.secutrial.com/) or REDCapTM (https://www.project-redcap.org/), online data management systems with the advantage to define several roles for several readers (data submission, analysis, read only, etc.).
Summary and conclusions
- Enjoy being a surgeon—it’s a tremendous personal and professional satisfaction and only a few careers provide the opportunity to have such a profound effect on the lives of others and to derive meaning from work;
- Research can add a very attractive dimension to your practice;
- Research can be performed in many ways from basic science, to translational to clinical research, in an academic or community-based setting;
- Identify your niche and research question and search for support by one or several mentors to get started;
- Obtain funding for your project, and if feasible for protected research time or short-term research fellowships.
Acknowledgments
We thank Dr. Chloe Spichiger for administrative support and Prof. Ilhan Inci for critical reading.
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Gilbert Massard) for the series “Training in Pulmonary Medicine and Surgery” published in Journal of Thoracic Disease. The article has undergone external peer review.
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jtd.2019.06.49). The series “Training in Pulmonary Medicine and Surgery” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Thakur A, Thakur V, Fonkalsrud EW, et al. The outcome of research training during surgical residency. J Surg Res 2000;90:10-2. [Crossref] [PubMed]
- Rudnicki PA, Liang F, Prince NH, et al. What Made Them Successful: An Introspective Survey of AAPS Members. Plast Reconstr Surg Glob Open 2015;3:e327 [Crossref] [PubMed]
- Lou X, Enter D, Sheen L, et al. Sustained supervised practice on a coronary anastomosis simulator increases medical student interest in surgery, unsupervised practice does not. Ann Thorac Surg 2013;95:2057-63. [Crossref] [PubMed]
- Upchurch GR Jr, Freischlag JA, Novicoff W, et al. Survey of the American College of Surgeons scholarship recipients: a story of generating academic leaders. J Am Coll Surg 2015;220:1122-7.e3. [Crossref] [PubMed]
- David EA, Nasir BS. Transition to practice, lessons learned: Academic general thoracic surgery. J Thorac Cardiovasc Surg 2016;151:920-4. [Crossref] [PubMed]
- What is basic research? In: National Science Foundation. Available online: https://www.nsf.gov/pubs/1953/annualreports/ar_1953_sec6.pdf. Accessed 3 January 2019.
- Clinical research. In: Wikipedia. Available online: https://en.wikipedia.org/wiki/Clinical_research. Accessed 3 January 2019.
- ESTS School. In: ESTS European Society of Thoracic Surgeons. http://www.ests.org/education/ests_school.aspx Accessed 3 January 2019.
- Robertson CM, Klingensmith ME, Coopersmith CM. Long-term outcomes of performing a postdoctoral research fellowship during general surgery residency. Ann Surg 2007;245:516-23. [Crossref] [PubMed]
- D'Amico TA, Tong BC, Berry MF, et al. Incorporating research into thoracic surgery practice. Thorac Surg Clin 2011;21:369-77. [Crossref] [PubMed]
- Robertson CM, Klingensmith ME, Coopersmith CM. Prevalence and cost of full-time research fellowships during general surgery residency. Ann Surg 2009;250:352-author reply 352. [Crossref] [PubMed]
- Scientific writing. In: Wikipedia. Available online: https://en.wikipedia.org/wiki/Scientific_writing. Accessed 3 January 2019.
- IMRAD. In: Wikipedia. Available online: https://en.wikipedia.org/wiki/IMRAD. Accessed 3 January 2019.
- Ko CY, Whang EE, Longmire WP Jr, et al. Improving the Surgeon's participation in research: is It a problem of training or priority? J Surg Res 2000;91:5-8. [Crossref] [PubMed]
- S. R. Graduate Medical Education (GME): surgical oncology. 2010. Available online: http://www.cc.nih.gov/training/gme/programs/surgical_oncology.html. Accessed 17 January 2011.
- Concato J, Shah N, Horwitz RI. Randomized, controlled trials, observational studies, and the hierarchy of research designs. N Engl J Med 2000;342:1887-92. [Crossref] [PubMed]


