
Disseminated adenoviral disease in immunocompetent adults supported with extracorporeal membrane oxygenation
Introduction
Adenovirus is a frequent cause of mild self-limiting upper respiratory tract infection, gastroenteritis, and conjunctivitis in infants and young children. There are currently 69 known serotypes of human adenoviruses (1), of which serotypes 3, 4, 7 and 21 account for most of the severe infections. Infections in immunocompetent adults first gained attention during the epidemics of the 1960s and early 1970s in military trainees (especially serotype 4), when no vaccine was available (1-3). In immunocompetent adults, serious adenovirus infections usually occur in the form of adenoviral pneumonia (4) with life-threatening sequelae such as acute respiratory failure, septic shock and encephalopathy (2). Disseminated adenovirus disease (DAD) is an entity that involves two or more organs from systemic adenoviral infection (5). Adenovirus serotypes 3 and 7 has been shown to cause disseminated fatal adenovirus disease in healthy children with predominant neurological complications (6). DAD needing extracorporeal membrane oxygenation (ECMO) has been rarely reported in adult immunocompetent patients.
Cidofovir has been found to be useful in the treatment of adenoviral pneumonia, though it is not FDA-approved for this indication. Due to its nephrotoxicity, it is contraindicated in patients with renal impairment. There is minimal published experience with cidofovir use in severe adenoviral pneumonia complicated by multi-organ failure and clear dosing information is not available.
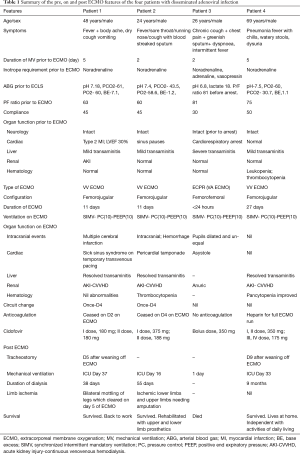
After Institutional Review Board approval for retrospective data collection, we report a case series of disseminated adenoviral disease in four previously healthy immunocompetent males who presented to us with rapidly developing respiratory failure and refractory hypoxemia needing cidofovir treatment and ECMO support. We also summarize the clinical features, management and outcome of severe adenovirus pneumonia in immunocompetent adults who needed ECMO as well as the rationale for cidofovir use for treatment of DAD (Table 1).
Full table
Case presentation
Case 1
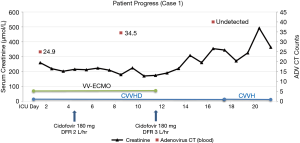
A 46-year-old morbidly obese [calculated body mass index (BMI) 44.3 kg/m2] gentleman, with history of hypertension and trigeminal neuralgia presented with features of community acquired pneumonia (CAP) and type I respiratory failure. Over a few days he had progressive respiratory symptoms necessitating intubation on fifth day of hospital admission. Despite optimal ventilation he developed refractory hypoxemia and needed veno-venous (VV) ECMO as rescue therapy. Antimicrobial therapy in the ICU was escalated to meropenam, azithromycin, vancomycin, amikacin and oseltamivir. The patient became oliguric due to acute kidney injury and he was commenced on continuous veno-venous hemodialysis (CVVHD). He had features of severe septic shock requiring high vasopressor support. Adenovirus serotype 7 was detected in blood and respiratory secretions by polymerase chain reaction (PCR). He was commenced on cidofovir. In lieu of anuric kidney failure on renal replacement therapy (RRT) and morbid obesity, cidofovir 180 mg (2 mg/kg based on adjusted body weight of 91 kg) was administered. He developed anisocoria on day 2 of ECMO and his CT revealed multiple areas of hemorrhagic infarcts in both cerebral hemispheres prompting us to temporarily stop anticoagulation. He also developed sick sinus syndrome for which he needed temporary trans venous pacing on day 10. On day 11, the second dose of cidofovir 180 mg was administered with oral probenecid. Adenoviral burden was quantified with serial cycle threshold (CT) counts. Details of cidofovir dosing, adenoviral CT counts, ECMO and CRRT support can be found in Figure 1. He was weaned off VV ECMO on day eleven. Subsequent doses of cidofovir were held off due to rising adenoviral CT counts, clinical and radiological improvement. The patient had tracheostomy on day 15 and weaned off completely on day 37. RRT was required till day 38, after which renal function recovered and remained stable at discharge. Aside from mild exposure keratopathy treated with artificial tears, ophthalmologic examination found no uveitis, iritis or other eye complications associated with cidofovir administration. The patient was transferred to a community hospital for further rehabilitation and has since gone home.
Case 2
A 21-year-old male with history of coryzal illness presented to the emergency department for persistent fever, cough with blood-streaked sputum, abdominal cramps and loose stools. There was no significant travel or contact history. Empirical treatment with amoxicillin-clavulanate and clarithromycin was started and escalated to meropenem, vancomycin and oseltamivir. He developed progressive respiratory failure needing intubation and ventilation on day five of hospital admission which progressed to ARDS with refractory hypoxemia and was started on VV-ECMO the same day. On day 2 of ECMO, the patient underwent percutaneous drainage for a pericardial effusion with tamponade. PCR of the pericardial fluid was positive for adenovirus. On day 3 left gaze deviation was noted on physical examination, prompting a CT scan of the brain which showed multiple foci of acute, small hemorrhages. Blood and ETT cultures remained negative for bacteria and fungi but a repeat Multiplex Viral PCR on BAL sample confirmed adenovirus serotype 7. Cidofovir 5mg/kg was administered together with probenecid and hydration. However, the patient developed acute kidney injury needing CRRT and this prompted us to reduce the next dose of cidofovir (2.5 mg/kg) on day 10. Adenoviral burden was quantified with serial CT counts performed before and after cidofovir. The patient also developed thrombocytopenia and progressive mottling of the skin on both upper and lower limbs, which subsequently turned gangrenous. A low A Disintegrin and Metalloproteinase with ThromboSpondin-1 motifs (ADAMST13) activity test raised suspicion of thrombocytopenia-associated multiple organ failure (TAMOF) and five sessions of plasma exchange were performed from day 8–12 with good results.
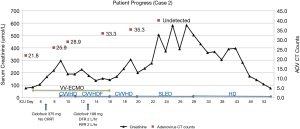
He was decannulated on Day 11. Surgical tracheostomy was performed to wean off ventilator support. He underwent multiple amputations of the lower limb and the digits. He was shifted to the general ward where he was rehabilitated and needed intermittent dialysis and was discharged three weeks later. Subsequent cidofovir doses were not administered given the clinical improvement and rising adenoviral CT counts. He was weaned off dialysis completely on day 55. He was discharged to a community hospital for rehabilitation on day 61. Details of cidofovir dosing, adenovirus PCR CT counts, ECMO and CRRT support can be found in Figure 2.
Case 3
A 26-year-old male with history of allergic rhinitis developed fever with features of lower respiratory tract infection. He was admitted to the hospital and was initially treated with antibiotics for CAP. As his respiratory failure worsened and progressed to ARDS, he was intubated and ventilated on day four of hospital admission. He progressed to septic shock requiring high inotropic and vasopressor support. On day five of ventilator support, he had refractory hypoxemia and was referred for ECMO retrieval. However, when the ECMO team arrived, he developed cardiac arrest; ECMO was initiated within 40 minutes with ongoing CPR and patient was retrieved on VA ECMO. He later developed severe shock liver (elevated transaminases) and acute kidney injury. He had no intrinsic cardiac activity despite active resuscitation. His bronchoalveolar lavage as well as his blood PCR later showed adenovirus type 7 from Multiplex PCR. He was initially loaded with cidofovir 5 mg/kg. However, he developed progressive multiorgan failure and ultimately treatment was withdrawn.
Case 4
A 67-year-old male with no significant past medical history was admitted with features of acute gastroenteritis. Laboratory investigations revealed leukopenia and thrombocytopenia. He had progressive cough and dyspnea leading to isolation for viral pneumonia. Upon admission, he was initially treated for suspected bacterial dysentery with ceftriaxone and later switched to levofloxacin. He developed respiratory distress on day 3 of hospitalization requiring intubation and was transferred to the medical ICU. Antibiotics were escalated to azithromycin, meropenem and oseltamivir. Blood and urine cultures at admission were negative for bacteria, however the Multiplex viral respiratory PCR at admission returned positive for adenovirus serotype 7. A diagnosis of adenoviral pneumonia with ARDS was made.
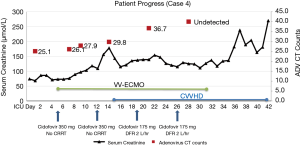
Oxygenation remained suboptimal despite maximum ventilator settings, sedation and paralysis. On day 5 of ICU admission, VV ECMO was commenced. Cidofovir was started at 5 mg/kg with probenecid after adequate hydration. Multiplex viral PCR and adenovirus PCR CT counts were monitored. After two weeks and two induction doses of cidofovir at 5mg/kg, the patient remained dependent on ECMO and adenoviral PCR CT count remained largely unchanged. However, the patient was weaned off vasopressors within 24 hours of initiating cidofovir therapy. The patient developed AKI on day 15 of ICU admission requiring CVVHD support. Subsequently, 2 more doses of cidofovir were given at a reduced dose of 2.5 mg/kg administered 1 week apart. He was successfully decannulated 27 days after ECMO support. Surgical tracheostomy was performed nine days following decannulation. Details of cidofovir dosing, adenovirus PCR CT counts, and its impact on ECMO can be found in Figure 3. His hospital stay was further complicated by Klebsiella pneumonia and Enterobacter bacteremia, both of which were appropriately treated with antibiotics. He was eventually transferred to a local hospital for further rehabilitation and renal support.
Discussion
In our series, we report four patients with DAD, who were immunocompetent community dwelling healthy adults. They had brief upper respiratory infections followed by rapidly progressive respiratory failure with multi-organ dysfunction needing ECMO within 24 hours of intubation. All of them had clinical evidence of cardiac involvement presenting with pericardial effusion, cardiac arrhythmias, or cardiac arrest in addition to severe shock. All of them had thrombocytopenia during the course of their treatment; two of them developed critical limb ischemia and gangrene. Three out of four patients were on VV ECMO; all of them had positive viral PCR serotyped as adenovirus serotype 7. Real Time PCR helped us monitor the viral load and response to cidofovir in three patients who survived. Two of them had clinical and radiological evidence of diffuse intracranial hemorrhage consistent with viral cerebritis, which required cessation of anticoagulation on ECMO. All 3 patients who were supported on veno-venous ECMO needed dialysis for acute kidney injury, survived to hospital discharge with minimal neurological sequelae.
Among the known 51 serotypes of human adenoviruses, serotypes 3 and 7 account for most of these severe infections. A review of the literature looking at patients with adenoviral pneumonia needing ECMO, including our cohort, revealed four case series and five case reports with 18 adult patients of which eight survived; 5 of these eight patients received cidofovir. Four patients from China went on VV ECMO for adenoviral pneumonia with serotype 55, but only one survived. All of them were immunocompetent young adults and they remained on ECMO for 8–11 days (7). Patients with severe adenovirus pneumonia (serotype 7) requiring ECMO support have been reported from Singapore in 2013. Of the three healthy adult patients who went on VV ECMO for severe respiratory failure, one survived. (4). Lee et al. reported two patients with adenoviral pneumonia who were treated with early cidofovir in addition to ECMO; one survived to hospital discharge by day 47 (8).
A review of the Extracorporeal Life Support Organization registry involving 163 children who needed ECMO support for adenoviral pneumonia reported a 62% overall mortality in this cohort. Neonates had a higher mortality than older infants or children (89% vs. 48%). Virulent strains of adenovirus (e.g., serotypes 3 and 7) in a genetically susceptible host impair cytokine, T-cell function, and expression of major histocompatibility complex expression (9). It is likely that the host’s immunological reaction to the infection leads to acute lung injury and multi organ dysfunction syndrome (10,11). Antiviral therapy administered late in the course of respiratory failure may not be effective. The use of cidofovir in adenoviral infection remains controversial, both in terms of dose and duration. Cidofovir use in ECMO or renal failure with or without CRRT is limited to two pharmacokinetic studies and 5 case reports, of these 3 patients were on both ECMO with CRRT and two on ECMO support only without renal impairment. An early study by Brody et al. suggested a theoretical dosing strategy to maintain adequate serum area-under-the curve in patients with varying degrees of renal impairment (12). Using this dosing strategy, Anglada Martínez et al. treated a previously healthy, immunocompetent female with community-acquired adenovirus pneumonia on continuous veno-venous haemodiafiltration (CVVHDF) with four doses of cidofovir at 2.5 mg/kg (half of the normal dose) (13). Vossen et al. recommended a regimen of 3–4 mg/kg weekly during continuous veno-venous hemofiltration (CVVH) based on a single-dose study (14). Refaat et al. reported a 54-year old male adult heart transplant recipient with adenoviral pneumonia on both ECMO and CVVHDF who was successfully treated with two doses of cidofovir at 3 mg/kg every 24 hours (15). Ha et al. reported 2 patients on ECMO and CRRT treated with cidofovir 5 mg/kg who recovered and were not dialysis-dependent, however details of CRRT mode and total cidofovir regimen were not available (16).
We considered the pharmacokinetic properties of cidofovir to estimate drug disposition. Drugs with low protein binding, low molecular weight and low volume of distribution (Vd) are determined to be readily removed by CRRT. For ECMO, lipophilic drugs get adsorbed to the circuit. Drugs with low Vd may have lower concentrations due to haemodilution from extra volume within the circuit (17). From its low molecular weight of 279 g/mol, low volume of distribution (Vd) of 0.5 L/kg, low protein binding of less than 7% and dianionic state under physiologic conditions (18), we inferred that cidofovir concentrations may be compromised due to high removal through CRRT and ECMO-related haemodilution, whilst not highly adsorbed to the ECMO circuit. In pharmacokinetic studies, approximately 30% of a single dose of cidofovir was removed during CVVH (19) and 50% during high flux HD (12).
Although renal impairment is a relative contraindication to cidofovir use, our patients received treatment as we believed the benefits outweighed the risks and no alternative agents were readily available. In our first patient, obesity provided a dosing conundrum depending on the choice of dosing weight, a wide range of possible regimens existed given his actual, adjusted and ideal body weights of 128, 91 and 65 kg respectively. We ultimately selected the adjusted body weight because adipose tissue is comparatively poorly vascularized, and cidofovir is hydrophilic and likely to be confined intravascularly. The second and fourth patients received subsequent doses of 2.5 mg/kg after acute kidney injury as per the regimen of Anglada Martínez et al. and the recommendation by Brody et al. Cidofovir has been used in haemopoietic stem cell recipient at a lower dose of 1 mg/kg thrice weekly (19). However, we opted for a regimen with a higher once-weekly dose because cidofovir action is concentration-dependent.
This is the first clinical experience with cidofovir in this region, in patients with multi-organ failure requiring both ECMO and CRRT support. Although a few case reports are available, none of them analyzed the effect of cidofovir on viral load; efficacy was assumed based on clinical improvement and not all patients survived the episode. 3 out of 4 patients had documented clearance of adenovirus on both CT count and on viral swab and were successfully weaned off ECMO support. The first and second patient were dialysis-free at 2 months and three out of four patients did not suffer from long-term hematologic or ophthalmologic adverse effects. Therefore, in view of scarce information on cidofovir in patients with ECMO and CRRT, this regimen appears safe and efficacious and could be considered for future cases. Due to the rarity of adenovirus pneumonia requiring ECMO and CRRT support, more experience is needed to draw a firm conclusion on the efficacy and safety of this regimen.
Conclusions
Immunocompetent adults can be susceptible to DAD. Adenovirus serotype 7 can cause severe respiratory failure even in immunocompetent hosts and can sometimes be fatal. Persistent high fever, dyspnea and rapid progression to multi organ failure within a week with features of ARDS are the most frequent clinical manifestations that necessitate ECMO in these patients. Three out of our four patients survived with mild neurological and renal sequelae; however the survival rates of adult patients with severe adenovirus pneumonia on ECMO reported in the literature is much lower than the rates reported for CAP (20) or influenza A(H1N1) pneumonia (21). Monitoring the viral load by PCR may be helpful in predicting patients’ disease severity and outcomes as well as adjusting cidofovir dosing. Cidofovir remains a promising agent in the treatment of adenovirus disease with careful dosing adjustment and vigilant monitoring in patients with renal failure and RRT.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jtd-19-2096). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was approved by the NHG Domain Specific Review Board (No. 2018/00645). The NHG DSRB has approved the waiver of informed consent.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Tan D, Zhu H, Fu Y, et al. Severe Community-Acquired Pneumonia Caused by Human Adenovirus in Immunocompetent Adults: A Multicenter Case Series. PloS one 2016;11:e0151199. [Crossref] [PubMed]
- Hakim FA, Tleyjeh IM. Severe adenovirus pneumonia in immunocompetent adults: a case report and review of the literature. Eur J Clin Microbiol Infect Dis 2008;27:153-8. [Crossref] [PubMed]
- Gu L, Qu J, Sun B, et al. Sustained Viremia and High Viral Load in Respiratory Tract Secretions Are Predictors for Death in Immunocompetent Adults with Adenovirus Pneumonia. PloS one 2016;11:e0160777. [Crossref] [PubMed]
- Low SY, Tan TT, Lee CH, et al. Severe adenovirus pneumonia requiring extracorporeal membrane oxygenation support--Serotype 7 revisited. Respir Med 2013;107:1810-3. [Crossref] [PubMed]
- Prodhan P, Bhutta AT, Gossett JM, et al. Extracorporeal membrane oxygenation support among children with adenovirus infection: a review of the Extracorporeal Life Support Organization registry. ASAIO J 2014;60:49-56. [Crossref] [PubMed]
- Munoz FM, Piedra PA, Demmler GJ. Disseminated adenovirus disease in immunocompromised and immunocompetent children. Clin Infect Dis 1998;27:1194-200. [Crossref] [PubMed]
- Sun B, He H, Wang Z, et al. Emergent severe acute respiratory distress syndrome caused by adenovirus type 55 in immunocompetent adults in 2013: a prospective observational study. Critical care 2014;18:456. [Crossref] [PubMed]
- Lee M, Kim S, Kwon OJ, et al. Treatment of Adenoviral Acute Respiratory Distress Syndrome Using Cidofovir With Extracorporeal Membrane Oxygenation. J Intensive Care Med 2017;32:231-8. [Crossref] [PubMed]
- Smith CA, Woodruff LS, Kitchingman GR, et al. Adenovirus-pulsed dendritic cells stimulate human virus-specific T-cell responses in vitro. J Virol 1996;70:6733-40. [Crossref] [PubMed]
- Prince GA, Porter DD, Jenson AB, et al. Pathogenesis of adenovirus type 5 pneumonia in cotton rats (Sigmodon hispidus). J Virol 1993;67:101-11. [Crossref] [PubMed]
- Gregory SM, Nazir SA, Metcalf JP. Implications of the innate immune response to adenovirus and adenoviral vectors. Future Virol 2011;6:357-74. [Crossref] [PubMed]
- Brody SR, Humphreys MH, Gambertoglio JG, et al. Pharmacokinetics of cidofovir in renal insufficiency and in continuous ambulatory peritoneal dialysis or high-flux hemodialysis. Clin Pharmacol Ther 1999;65:21-8. [PubMed]
- Anglada Martínez H, Carcelero San Martín E, Castro Rebollo P, et al. Cidofovir dosage in a critically ill patient undergoing continuous veno-venous hemodiafiltration. Farm Hosp 2014;38:71-3. [PubMed]
- Vossen MG, Gattringer KB, Jager W, et al. Single-dose pharmacokinetics of cidofovir in continuous venovenous hemofiltration. Antimicrob Agents Chemother 2014;58:1952-5. [Crossref] [PubMed]
- Refaat M, McNamara D, Teuteberg J, et al. Successful cidofovir treatment in an adult heart transplant recipient with severe adenovirus pneumonia. J Heart Lung Transplant 2008;27:699-700. [Crossref] [PubMed]
- Ha SO, Kim HS, Park S, et al. Severe ARDS caused by adenovirus: early initiation of ECMO plus continuous renal replacement therapy. Springer plus 2016;5:1909. [Crossref] [PubMed]
- Sherwin J, Heath T, Watt K. Pharmacokinetics and Dosing of Anti-infective Drugs in Patients on Extracorporeal Membrane Oxygenation: A Review of the Current Literature. Clin Ther 2016;38:1976-94. [Crossref] [PubMed]
- Cundy KC. Clinical pharmacokinetics of the antiviral nucleotide analogues cidofovir and adefovir. Clin Pharmacokinet 1999;36:127-43. [Crossref] [PubMed]
- Nagafuji K, Aoki K, Henzan H, et al. Cidofovir for treating adenoviral hemorrhagic cystitis in hematopoietic stem cell transplant recipients. Bone Marrow Transplant 2004;34:909-14. [Crossref] [PubMed]
- Ramanathan K, Tan CS, Rycus P, et al. Extracorporeal Membrane Oxygenation for Adult Community-Acquired Pneumonia: Outcomes and Predictors of Mortality. Crit Care Med 2017;45:814-21. [Crossref] [PubMed]
- Australia and New Zealand Extracorporeal Membrane Oxygenation (ANZ ECMO) Influenza Investigators, Davies A, Jones D, et al. Extracorporeal Membrane Oxygenation for 2009 Influenza A(H1N1) Acute Respiratory Distress Syndrome. JAMA 2009;302:1888-95. [Crossref] [PubMed]


