Percutaneous trans-jugular vein closure of atrial septal defect with steerable introducer under echocardiographic guidance
Introduction
Percutaneous transcatheter closure of atrial septal defect (ASD) is one of the main ASD closure approaches (1-3). The percutaneous transcatheter method of ASD closure is performed under X-ray with the potential radial damage. It can be avoided using only the echocardiographic guidance (4,5), but in this method, the patient’s age and the size of the defect were still restricted (6). Transthoracic ASD closure (2,3,7) is a modified method with no radial involvement, no age limit, but wider indications in this decade. However, the transthoracic closure procedure still needs 1-2 cm chest wall incision and operates in the thoracic. So its minimally invasion has been questioned. Since January 2015, the authors have adopted a new method of percutaneous trans-jugular vein closure of ASD with steerable introducer under echocardiographic guidance, which is a good solution to the limitations for above methods and achieved good clinical results.
Materials and methods
General data
From January 2015 to May 2015, 10 patients had been operated with percutaneous trans-jugular vein closure of ASD with steerable introducer under echocardiographic guidance, including three males and seven females, aged 0.8-9 (3.3±3.2) years old, weight 6.0-29.5 (12.3±7.6) kg, with ASD diameter of 6-23 mm.
Inclusion criteria (7,8): single secundum ASD with diameter exceeds or equals to 5 mm and the distance of the edge of the defect to inferior vena cava, pulmonary vein and mitral valve is more than or equals to 5 mm. Atrial septal stretch diameter is greater than or equals to the diameter of the left side of the occluder.
The electrocardiogram, chest X-ray, transthoracic echocardiography (TTE) were examined routinely before the operation. The diameter of right internal jugular vein and right femoral vein were measured then evaluated by paired samples t-test.
This study have applied for the hospital new technology project, and obtained the approval of Medical Ethic Committee. The patients or their guardians have also signed the informed consent.
Surgical techniques
Under endotracheal intubation and general anesthesia, transesophageal echocardiography (TEE, Philips IE33) was done at the beginning of the procedure to choose the appropriate occluder. The patients took supine and trendelenburg position, shoulders being padded up and heading to the left and as back as possible. Touched the inner edge of the sternocleidomastoid and the carotid pulsation. Inserted needle at the position of 0.5 cm to the outer edge of the pulse point. The needle formed a 30-degree angle against the skin pointing to the homolateral nipple. The right internal jugular vein puncture for vascular access was underwent and the steerable introducer (made by Lifetech Scientific, Shenzhen) with 20 cm in length, 0-160 degree steerable angle in the tip of the introducer (as shown in Figure 1), was inserted into the vessel through the guide-wire. The depth equaled to the distance from the puncture point to the right nipple, then withdrew the guide-wire and dilator. The sheath can be clearly visualized by TEE. Adjust the angle and depth of the tip of sheath to make it perpendicular to the middle of ASD plane and pass through ASD about 1 cm, Chose an appropriate size of occluder (made by Lifetech Scientific, Shenzhen). Delivered the occluder by the sheath, and released the left disk then the right disk. Gentlely pushed and pulled the delivery cable to ensure the stability of the occluder. The occluder would be released only if the echocardiography demonstrated a correct position without evidence of significant residual shunt, atrioventricular valve malfunction, or venous obstruction. At the end, pressed the puncture point for 10-20 minutes to stop bleeding (see Figure 2).

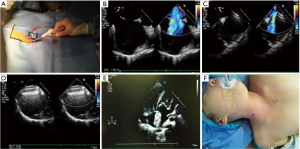
In this research, the procedure time is defined as the time from the internal jugular vein puncture to the removal of the sheath, and intracardiac operation time refers to the time from operating the introducer into the right atrium to the occluder released.
After the operation, the antibiotic drugs were given for 24 hours and 3-4 mg/kg of aspirin was taken orally for 6 months.
All patients were examined by echocardiography in our hospital for post-operation follow up after one month of the operation.
Results
All ASD cases were occluded successfully without any thoracotomy converting. The procedure time was 27.4±5.6 mins and the intracardiac operation time was 6.7±5.2 mins. There was no blood loss, no blood transfusion during the operation; there was no death, no serious arrhythmia, no hemolysis, no intracardiac infection and no injury or embolization of internal jugular vein in patients’ hospitalization. All cases were free from residual shunt after the operation examined by TEE.
Ultrasound examination showed that the diameter of right internal jugular vein was 6.98±1.15 mm, and right femoral vein was 5.01±0.76 mm. The paired samples t-test showed that the diameter of right internal jugular vein was larger than the right femoral vein in the same patient and P<0.01.
There was no residual shunt, no occluder detachment or displacement and other complications in post-operation follow-up after one month of the operation.
Discussion
With the advantages of no incision and cardiopulmonary bypass (CPB), percutaneous ASD closure has become the main treatment for ASD (9,10) as Amplatzer occluder was adopted since 1997 (11). However, there are some disadvantages, such as (8): (I) large radial equipments are needed, with radial injury. And age limit for it can commonly be applied in patients over two years old; (II) long delivery system, poor handling; (III) the sheath is nearly parallel to ASD, so it is difficult to position the occluder especially for a larger ASD because the occluder is easy to detach or displace.
Trans femoral vein ASD closure under echocardiographic guidance avoids the radial injury, but defects still exist for X-ray will perform as mediation in percutaneous closure.
Transthoracic ASD closure is a new method in recent 10 years with no radial contact, no age limit, but wider indications, shorter delivery system, more flexible handling, with sheath perpendicular to the plane of ASD. However, the procedure still needs 1.5-2 cm incision on the chest.
Percutaneous trans-jugular vein closure of ASD with steerable introducer under echocardiographic guidance is a novel surgical method with the following advantages: (I) free from large radial equipment and radial damage; (II) the anatomical structure of heart and the delivery sheath can be visualized clearly by TEE (12); (III) the diameter of internal jugular vein is larger than femoral vein which can accept larger sheath, even the infant younger than 1-year-old is suitable for ASD closure; (IV) the tip of the sheath can be adjusted from 0-160 degree to accurately make the occluder perpendicular to the plane of ASD; (V) shorter delivery system and flexible handling; (VI) the sheath can reach into ASD directly without guide-wire and dilator into the heart, so it will reduce the damage of the heart; (VII) for larger ASD, since the sheath is perpendicular to ASD, it has the same closure effect as the transthoracic ASD closure dose; (VIII) the operation was done in the routine operating room which can be immediately converted to a CPB operation in case the percutaneous trans-jugular vein closure of ASD fails.
In conclusion, percutaneous trans-jugular vein closure of ASD with steerable introducer under echocardiographic guidance is a novel approach with simple operation, mild damage, but wider indications and less complications which has obtained satisfactory clinical effect. It has obvious advantages compared to the traditional percutaneous intervention and transthoracic ASD closure. This procedure not requiring special equipment and being operating in the routine operating room makes it easy to be promoted with promising applications.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Jones TK, Latson LA, Zahn E, et al. Results of the U.S. multicenter pivotal study of the HELEX septal occluder for percutaneous closure of secundum atrial septal defects. J Am Coll Cardiol 2007;49:2215-21. [PubMed]
- Kardon RE, Sokoloski MC, Levi DS, et al. Transthoracic echocardiographic guidance of transcatheter atrial septal defect closure. Am J Cardiol 2004;94:256-60. [PubMed]
- Zaqout M, Suys B, De Wilde H, et al. Transthoracic echocardiography guidance of transcatheter atrial septal defect closure in children. Pediatr Cardiol 2009;30:992-4. [PubMed]
- Petit CJ, Justino H, Pignatelli RH, et al. Percutaneous atrial septal defect closure in infants and toddlers: predictors of success. Pediatr Cardiol 2013;34:220-5. [PubMed]
- Pan XB, Ou-Yang WB, Pang KJ, et al. Percutaneous Closure of Atrial Septal Defects Under Transthoracic Echocardiography Guidance Without Fluoroscopy or Intubation in Children. J Interv Cardiol 2015;28:390-5. [PubMed]
- Papa M, Gaspardone A, Fragasso G, et al. Feasibility and safety of transcatheter closure of atrial septal defects with deficient posterior rim. Catheter Cardiovasc Interv 2013;81:1180-7. [PubMed]
- Wan L, Yu BT, Wu QC, et al. Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass. Genet Mol Res 2015;14:3760-6. [PubMed]
- Vasquez AF, Lasala JM. Atrial septal defect closure. Cardiol Clin 2013;31:385-400. [PubMed]
- Takaya Y, Akagi T, Kijima Y, et al. Long-term outcome after transcatheter closure of atrial septal defect in older patients: impact of age at procedure. JACC Cardiovasc Interv 2015;8:600-6. [PubMed]
- Meier B. Percutaneous Closure of Atrial Septal Defects: Contraindications Are Hard to Find These Days. JACC Cardiovasc Interv 2015;8:607-8. [PubMed]
- Yew G, Wilson NJ. Transcatheter atrial septal defect closure with the Amplatzer septal occluder: five-year follow-up. Catheter Cardiovasc Interv 2005;64:193-6. [PubMed]
- Aubry P, Brochet E, Verdonk C, et al. 3-D transoesophageal echocardiography guidance in percutaneous closure of three distant atrial septal defects. Eur Heart J Cardiovasc Imaging 2015. [Epub ahead of print]. [PubMed]


