Comparison of perioperative outcomes following hybrid minimally invasive versus open Ivor Lewis esophagectomy for esophageal cancer
Introduction
When considering locoregional control and long-term survival, surgical resection is the preferred method of treatment for esophageal cancer. However, the usefulness of this modality is still debated owing to patients’ high morbidities and mortalities. Despite continuous advances in perioperative management and surgical techniques, postoperative morbidity and mortality rates range from 30–50% and 2–10%, respectively (1). Thoracoscopic mobilization of the thoracic esophagus was introduced by Cuschieri et al. in 1992 to help overcome these limitations; since then, additional advances have led to minimally invasive esophagectomy (MIE), which has become increasingly popular (2). Several variations of this surgical procedure, such as total or hybrid MIE performed via thoracoscopy and/or laparoscopy, laparoscopic-assisted transhiatal esophagectomy, and robot-assisted MIE, have been reported (3). These updated MIE modalities reportedly produce equivalent oncologic outcomes with several added benefits, such as reduced morbidity and/or mortality rates and shorter hospital stays (4,5). However, only a handful of randomized controlled trials exist (6,7), and although several meta-analyses have been performed, the safety and efficacy of MIE remain unclear (8-10).
Because conclusive results that confirm the theoretical advantages of MIE compared with open surgery are lacking, we performed this study under the hypothesis that hybrid MIE that utilizes the advantages of both open and laparoscopic approaches may improve perioperative outcomes. Thus, we investigated patients who underwent Ivor Lewis esophagectomy for middle or lower thoracic esophageal cancer to compare the perioperative outcomes of those who received laparoscopic gastric mobilization and open right thoracotomy (the hybrid approach) and those who were treated via the conventional open approach.
Methods
Patients
This retrospective study was reviewed and approved by the Institutional Review Board of the Chonnam National University Hwasun Hospital (IRB approved No. CNUHH-2017-096). Informed consent was waived by the board. We enrolled 153 consecutive patients with middle or lower thoracic esophageal squamous cell cancer who underwent Ivor Lewis esophagectomy at our institution between January 2008 and December 2016. A single surgeon performed all the surgeries. The surgical strategies for esophageal cancer at our hospital changed over time: from late 2004 (when MIE was first introduced) to 2007, “three-phase” McKeown-type esophagectomy was mostly performed irrespective of the location of the esophageal cancer, and if possible, the MIE method suggested by Luketich et al. (11) was preferentially considered. Since 2008, upper thoracic esophageal cancer has been treated using the same technique, while middle or lower thoracic esophageal cancer has been treated via Ivor Lewis esophagectomy. The duration of our study was divided into three subperiods; hybrid minimally invasive Ivor Lewis esophagectomy (HIL) has been preferentially performed over the open approach during subperiod 3, i.e., since 2014 (Table 1). Sixteen patients who underwent complete MIE and 22 who received neoadjuvant treatment (4 in the hybrid group and 18 in the open group) were excluded. As a result, a total of 115 patients were divided into the HIL group and the OIL group; their clinical characteristics (age, sex, preoperative pulmonary function, location of the tumor, and results of preoperative laboratory tests) and perioperative outcomes (results of postoperative laboratory tests, surgery-related factors, and postoperative morbidity and mortality) were compared.
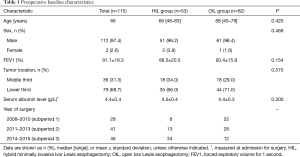

Full table
Preoperative assessment of resectability and workup for clinical staging were performed identically for all patients. Physical examination, standard laboratory tests, pulmonary function tests, computed tomography of the thorax and abdomen, upper gastrointestinal endoscopy including endoscopic ultrasound, and positron emission tomography were performed routinely.
Pathologic staging was based on the American Joint Committee on Cancer seventh edition TNM staging definitions (12). Serum albumin levels were compared between measurements taken preoperatively and those obtained immediately postoperatively. Preoperative white blood cell (WBC) counts and serum C-reactive protein (CRP) levels were mostly in the normal range; CRP measurements were obtained immediately postoperatively, and WBCs were measured on postoperative day 1. Overall postoperative complications were classified according to the Clavien-Dindo classification (13), and patients with two or more complications were classified based on their worst complication. Pulmonary complications included acute lung injury (respiratory insufficiency), pneumonia, pleural effusion, and atelectasis. The 30-day and in-hospital mortalities were analyzed.
Surgical procedures
A laparoscopic surgical technique using five trocars has been previously described in detail (14). Briefly, gastric mobilization was performed using an energy-based device with en bloc lymph node dissection in the celiac region. The lesser curvature of the stomach was divided with an Endo GIA linear stapler to create a gastric tube. Except during subperiod 1, pyloroplasty or pyloromyotomy using an electrocautery device was performed in almost all patients.
As in the laparoscopic approach, the open abdominal approach involved gastric mobilization and tubularization with lymphadenectomy. Except for a few cases of pyloroplasty, pyloric digital fracture was performed in almost all patients. We performed feeding jejunostomy only in patients who were likely to require delayed enteral feeding via the oral route among the patients who underwent the open approach.
A posterolateral thoracotomy in the fourth intercostal space of approximately 15 cm was performed. After esophageal mobilization and mediastinal lymph node dissection, esophagogastric anastomosis using a 28-mm end-to-end anastomosis circular stapler was performed high above the azygos vein; a safety margin of at least 5 cm was required. Lymphadenectomy was performed using the concept of “extended two-field lymph node dissection,” according to the lymph node map of the Japanese Society for Esophageal Diseases (15), including upper thoracic paraesophageal (#105), recurrent nerve (#106rec), and tracheobronchial (#106tb) lymph nodes. The redundant portion of the fundus was excised with an Endo GIA reticulating stapler. All patients were extubated in the operating room and transferred to the intensive care unit.
Statistical analysis
All data were presented as either mean ± standard deviation or median and range where indicated. Categorical variables were compared using the Pearson chi-square test or two-tailed Fisher’s exact test. The t-test was used to compare independent continuous variables. A P value less than 0.05 was considered statistically significant. Statistical analyses were performed using SPSS for Windows, version 19 (IBM, Chicago, IL).
Results
Among 115 patients who underwent Ivor Lewis esophagectomy, 53 were in the HIL group and 62 were in the OIL group. Preoperative baseline characteristics are shown in Table 1. The median patient age was 66 years (range, 45–83 years); the vast majority of patients were male (n=112, 97.4%). The proportion of the HIL group has increased over the subperiods; the hybrid approach was performed in about 75% of the cases in subperiod 3. The two groups were comparable with respect to age, sex, pulmonary function (percentage of forced expiratory volume for 1 second), tumor location, and preoperative serum albumin level. Furthermore, preoperative WBC counts and serum CRP levels were mostly in the normal range. In terms of surgical data (Table 2), there were no significant differences in the durations of surgery, method of anastomosis, and additional procedures performed between the groups; however, the two groups significantly differed in pyloric management (P<0.001). In the OIL group, pyloroplasty was only performed in eight patients (12.9%); the majority (n=52, 83.9%) underwent pyloric digital fracture. In the HIL group, the pyloric procedure was not performed in subperiod 1, and pyloromyotomy (n=18, 34%) or pyloroplasty (n=21, 39.6%) was chosen intermittently in the later periods. The mean number of harvested lymph nodes was 25.5; the difference between the groups was not significant. However, pathologic stage significantly differed between the two groups; the proportion of advanced-stage tumors was significantly higher in the OIL group (P=0.003).
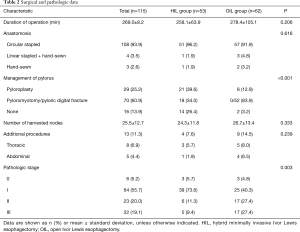
Full table
Postoperative data are shown in Table 3. Laboratory tests showed no significant differences in WBC counts; however, the HIL group had a higher serum albumin level (means: 3.4 vs. 2.9 g/dL in the HIL and OIL groups, respectively; P<0.001). Moreover, the mean serum CRP level in the HIL group (6.4 mg/L) was significantly lower than in the OIL group (8.1 mg/L; P=0.001).
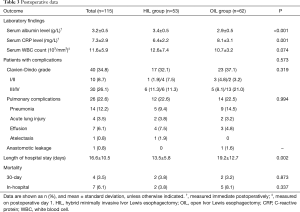
Full table
Postoperative complications occurred in 40 patients (34.8%). According to the Clavien-Dindo classification, 36 patients had complications that were grade II or higher (31.3%). Overall morbidity was higher in the OIL group (37.1%) than in the HIL group (32.1%) but not significantly. Pulmonary complications occurred in 26 patients (22.6%), although no significant differences between the two groups were observed. Anastomotic leakage only occurred in one patient in the open group (1.6%) and was resolved by thoracotomic reoperation. Other major complications were hoarseness with transient vocal cord palsy (n=7), acute renal failure (n=3), atrial fibrillation (n=3), and chyle leakage (n=2).
The mean length of hospital stay was 16.6 days, and there was a significant difference between the groups (means: 13.5 vs. 19.2 days in the HIL and OIL groups, respectively; P=0.002). The overall 30-day mortality rate was 3.5%, while the in-hospital mortality rate was 6.1%. The OIL group showed a higher in-hospital mortality rate than the HIL group, but not to a significant degree.
Discussion
Surgical resection is the most effective treatment modality for esophageal cancer in terms of locoregional control and long-term survival. Surgical approaches vary with respect to transthoracic vs. transhiatal esophagectomy, intrathoracic vs. cervical anastomosis, and the degree of lymphadenectomy; the choice and sequence of these modalities depend on the preference of the surgeon and the institution (16). Although optimal surgical strategies are still debated, the Ivor Lewis procedure with two-field lymph node dissection remains the most preferred technique for middle and lower esophageal cancer (17). Our institution experimented with the change in surgical strategies but now preferentially performs this technique for middle or lower thoracic esophageal cancer.
High postoperative morbidity and mortality remain a point of concern in the surgical treatment of esophageal cancer. Although Wright et al. recently reported improved outcomes in the major morbidity rate (24%) and hospital mortality rate (2.7%) based on 2,315 esophagectomy cases (18), morbidity and mortality remain high in most institutions, reaching 30–50% and 2–10%, respectively (1). MIE addresses some of these drawbacks; its advantages include less blood loss, lower respiratory-related and total morbidity, and shorter hospital stay. As mentioned previously, the short- and long-term outcomes of MIE vs. those of conventional open surgery are comparable; however, the efficacy of MIE has remained controversial (8-10). Randomized controlled trials have been few (6,7,19) and include the MIRO trial published by Mariette et al. in 2015. Notably, however, the MIRO trial compared laparoscopic gastric mobilization with the open abdominal approach in patients who underwent transthoracic esophagectomy with two-field lymphadenectomy; i.e., the study essentially compared hybrid MIE with the conventional open approach. They found that the hybrid group had a significantly lower prevalence of major pulmonary complications and postoperative morbidities (20).
Although several reports that described the outcomes of MIE included the hybrid technique, few reports focused only on the hybrid technique. Briez et al. reported that the prevalence of major pulmonary complications was significantly lower in the laparoscopic hybrid MIE group than in the open group (15.7% vs. 42.9%, respectively); the same was true for overall morbidity (35.7% vs. 59.3%, respectively) and in-hospital mortality (1.4% vs. 7.1%, respectively), with similar 2-year survival rates between the two groups (21). In a French nationwide study of approximately 3,000 patients, Messager et al. compared laparoscopic gastric mobilization with open surgery; they found that the 30-day postoperative mortality was significantly lower in the hybrid (laparoscopic) group even after propensity score matching (3.3% vs. 5.9%), although they did not mention morbidity (22). More recently, Bjelovic et al. confirmed some benefits of hybrid MIE as previously described and also reported that a greater number of lymph nodes were harvested from patients who underwent hybrid MIE using laparoscopy than from those who underwent open surgery (31.9 vs. 26.3, respectively) (23). In our study, there was no significant difference in overall morbidity between the two groups; however, this is not too meaningful since both groups had relatively low incidences of grade II or higher complications on the Clavien-Dindo grade (30.1% in the HIL group vs. 32.3% in the OIL group). We thought that several factors such as a single experienced surgeon and a consistent setting for esophagectomies likely contributed to the lower morbidity, including the lower incidence of anastomotic leakage (0.8% of all patients). This corroborates our expectation that one of the benefits of hybrid MIE ought to be meticulous lymph node dissection and sound anastomosis via an open thoracotomy.
Previous studies have expounded on the advantages of laparoscopy. First, a laparoscopic approach may lower the level of inflammatory response to surgical trauma by reducing muscular stress and pain and may lower fluid and consequent albumin loss by avoiding the opening of the abdomen (24). Various factors such as interleukin, procalcitonin, liver enzyme (e.g., aspartate transaminase), and lactate levels have been used to assess inflammatory responses induced by surgical stress, which in turn are reported to be associated with postoperative complications such as pneumonia and sepsis (25,26). As this study was retrospective in nature, we chose the WBC count and CRP level as inflammatory markers because these two parameters were easily measured and were available for most patients. Preoperative measurements of these two parameters were generally in the normal range; however, despite the use of the same antibiotics and perioperative management protocol, serum CRP levels on postoperative day 1 were significantly lower in the HIL group.
Serum albumin levels are another important indicator of postoperative recovery. Ryan et al. reported that hypoalbuminemia on the first postoperative day is closely associated with morbidity, including pulmonary complications (27), and several studies have noted that serum albumin levels are associated with anastomotic leaks, in-hospital deaths, and prolonged hospital stays (28). In our study, the HIL group had a significantly higher serum albumin level immediately postoperatively. We posit that the fact that the HIL group had less inflammatory response and better nutritional status may have had beneficial effects on postoperative recovery, thereby shortening the hospital stay. Although Scarpa et al. reported findings that were consistent with ours, they had a relatively small sample size, and patients who underwent the two-phase and three-phase (cervical anastomosis) techniques were enrolled together (29).
Patients who underwent neoadjuvant chemoradiation experienced difficulties at the time of surgery due to postradiation changes, which in turn may have affected the complication rates and durations of hospital stay. However, hybrid MIE using laparoscopy is predicted to be easy to apply even to such patients, as the irradiated thoracic field can easily be accessed via thoracotomy. Although we excluded patients who received neoadjuvant treatment to ensure homogeneity between the two groups, Woodard et al. reported that performing HIL in patients who underwent neoadjuvant chemoradiation led to minimal morbidity and excellent long-term survival outcomes (30).
This study has a few limitations. First, the initially devised case-control study was replaced with a retrospective analysis. To compensate for this, we limited esophageal cancer to squamous cell carcinoma and the surgical technique to Ivor Lewis esophagectomy to minimize heterogeneity among the subjects. Second, WBC and CRP are not typically used to represent inflammatory status. As previously mentioned, we chose these parameters for their ease of measurement and likely availability in patients’ records. Finally, this study did not include an analysis of postoperative survival; we determined that such an analysis would be meaningless due to the differences in the pathologic stages between the two groups. Analysis of postoperative survival remains a task for future studies after more data on the hybrid technique are accumulated.
In conclusion, we found that HIL has the advantage of better postoperative nutritional and inflammatory status, resulting in shorter hospital stays. Hybrid MIE could be considered a transition stage from conventional open surgery to total MIE, but our findings suggest that it is an excellent surgical option at this point when concrete evidence on the efficacy of total MIE is lacking.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: This study was approved by the Institutional Review Board of the Chonnam National University Hwasun Hospital (IRB approved No. CNUHH-2017-096) and informed consent was waived by the board.
References
- Mariette C, Piessen G, Triboulet JP. Therapeutic strategies in oesophageal carcinoma: role of surgery and other modalities. Lancet Oncol 2007;8:545-53. [Crossref] [PubMed]
- Cuschieri A, Shimi S, Banting S. Endoscopic oesophagectomy through a right thoracoscopic approach. J R Coll Surg Edinb 1992;37:7-11. [PubMed]
- Watanabe M, Baba Y, Nagai Y, et al. Minimally invasive esophagectomy for esophageal cancer: an updated review. Surg Today 2013;43:237-44. [Crossref] [PubMed]
- Dantoc MM, Cox MR, Eslick GD. Does minimally invasive esophagectomy (MIE) provide for comparable oncologic outcomes to open techniques? A systematic review. J Gastrointest Surg 2012;16:486-94. [Crossref] [PubMed]
- Schoppmann SF, Prager G, Langer FB, et al. Open versus minimally invasive esophagectomy: a single-center case controlled study. Surg Endosc 2010;24:3044-53. [Crossref] [PubMed]
- Biere SS, van Berge Henegouwen MI, Maas KW, et al. Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet 2012;379:1887-92. [Crossref] [PubMed]
- Briez N, Piessen G, Bonnetain F, et al. Open versus laparoscopically-assisted oesophagectomy for cancer: a multicentre randomised controlled phase III trial - the MIRO trial. BMC Cancer 2011;11:310. [Crossref] [PubMed]
- Guo W, Ma X, Yang S, et al. Combined thoracoscopic-laparoscopic esophagectomy versus open esophagectomy: a meta-analysis of outcomes. Surg Endosc 2016;30:3873-81. [Crossref] [PubMed]
- Biere SS, Cuesta MA, van der Peet DL. Minimally invasive versus open esophagectomy for cancer: a systematic review and meta-analysis. Minerva Chir 2009;64:121-33. [PubMed]
- Sgourakis G, Gockel I, Radtke A, et al. Minimally invasive versus open esophagectomy: meta-analysis of outcomes. Dig Dis Sci 2010;55:3031-40. [Crossref] [PubMed]
- Luketich JD, Alvelo-Rivera M, Buenaventura PO, et al. Minimally invasive esophagectomy: outcomes in 222 patients. Ann Surg 2003;238:486-94. [PubMed]
- Rice TW, Blackstone EH, Rusch VW. 7th edition of the AJCC cancer staging manual: esophagus and esophagogastric junction. Ann Surg Oncol 2010;17:1721–4.
- Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 2004;240:205-13. [Crossref] [PubMed]
- Song SY, Na KJ, Oh SG, et al. Learning curves of minimally invasive esophageal cancer surgery. Eur J Cardiothorac Surg 2009;35:689-93. [Crossref] [PubMed]
- Japan Esophageal Society. Japanese classification of esophageal cancer, tenth edition: part I. Esophagus 2009;6:1-25.
- Pennathur A, Luketich JD. Resection for esophageal cancer: strategies for optimal management. Ann Thorac Surg 2008;85:S751-6. [Crossref] [PubMed]
- Pennathur A, Zhang J, Chen H, et al. The “best operation” for esophageal cancer? Ann Thorac Surg 2010;89:S2163-7. [Crossref] [PubMed]
- Wright CD, Kucharczuk JC, O'Brien SM, et al. Predictors of major morbidity and mortality after esophagectomy for esophageal cancer: a society of thoracic surgeons general thoracic surgery database risk adjustment model. J Thorac Cardiovasc Surg 2009;137:587-95. [Crossref] [PubMed]
- Biere SS, Maas KW, Bonavina L, et al. Traditional invasive vs. minimally invasive esophagectomy: a multi-center, randomized trial (TIME-trial). BMC Surg 2011;11:2. [Crossref] [PubMed]
- Mariette C, Meunier B, Pezet D, et al. Hybrid minimally invasive vs open oesophagectomy for patients with oesophageal cancer: a multicenter, open-label, randomized phase III controlled trial, the MIRO trial. J Clin Oncol 2015.33. abstract 5.
- Briez N, Piessen G, Torres F, et al. Effects of hybrid minimally invasive oesophagectomy on major postoperative pulmonary complications. Br J Surg 2012;99:1547-53. [Crossref] [PubMed]
- Messager M, Pasquer A, Duhamel A, et al. Laparoscopic gastric mobilization reduces postoperative mortality after esophageal cancer surgery: a French Nationwide Study. Ann Surg 2015;262:817-22. [Crossref] [PubMed]
- Bjelovic M, Babic T, Spica B, et al. Could hybrid minimally invasive esophagectomy improve the treatment results of esophageal cancer? Eur J Surg Oncol 2016;42:1196-201. [Crossref] [PubMed]
- Lee JH, Han HS, Lee JH. A prospective randomized study comparing open vs. laparoscopy-assisted distal gastrectomy in early gastric cancer. Surg Endosc 2005;19:168-73. [Crossref] [PubMed]
- Durila M, Bronský J, Haruštiak T, et al. Early diagnostic markers of sepsis after oesophagectomy (including thromboelastography). BMC Anesthesiol 2012;12:12. [Crossref] [PubMed]
- Maas KW, Biere SS, van Hoogstraten IM, et al. Immunological changes after minimally invasive or conventional esophageal resection for cancer: a randomized trial. World J Surg 2014;38:131-7. [Crossref] [PubMed]
- Ryan AM, Hearty A, Prichard RS, et al. Association of hypoalbuminemia on the first postoperative day and complications following esophagectomy. J Gastrointest Surg 2007;11:1355-60. [Crossref] [PubMed]
- Goh SL, De Silva RP, Dhital K, et al. Is low serum albumin associated with postoperative complications in patients undergoing oesophagectomy for oesophageal malignancies? Interact Cardiovasc Thorac Surg 2015;20:107-13. [Crossref] [PubMed]
- Scarpa M, Cavallin F, Saadeh LM, et al. Hybrid minimally invasive esophagectomy for cancer: impact on postoperative inflammatory and nutritional status. Dis Esophagus 2016;29:1064-70. [Crossref] [PubMed]
- Woodard GA, Crockard JC, Clary-Macy C, et al. Hybrid minimally invasive Ivor Lewis esophagectomy after neoadjuvant chemoradiation yields excellent long-term survival outcomes with minimal morbidity. J Surg Oncol 2016;114:838-47. [Crossref] [PubMed]


