Laser resection of pulmonary nodule via uniportal thoracoscopic surgery
Introduction
Uniportal video-assisted thoracic surgery (VATS) is increasing in popularity (1,2). Operating through a single incision may reduce postoperative pain and discomfort. Uniportal VATS wedge resection was first described by Rocco in 2004 (3). During uniportal VATS wedge lung resections, usually three instruments including a thoracoscope, lung retraction instrument as well as an endostapler are required and placed through the surgical incision. The endostapler is the largest by diameter of these instruments that occupy the uniportal incision. Although there have been substantial advances in development of smaller and variable angulated thoracoscopes (4), as well as narrower double-hinged VATS graspers and retractors over the years (5), thus allowing ever smaller uniportal incisions and reduced instrument fencing (6), the “Achilles Heel” remain the size of the endostapler. We describe our technique for uniportal VATS lung wedge resection by diode laser that allows further miniaturization of the uniportal VATS wound.
Operative technique
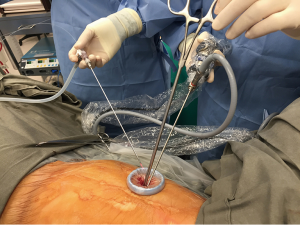
A 53-year-old non-smoking gentleman with a peripheral 1.2 cm left lower lobe lesion was scheduled for uniportal VATS lung wedge resection and frozen section. Standard general anesthesia with double lumen tube endobronchial intubation was performed, the patient was placed in lateral decubitus position and left lung was collapsed. A 1.5-cm incision was made over the left anterior axillary line at 5th intercostal space. An O-silk was tied to the inner rubber ring of a small size Alexis-type wound protector (SurgiSleeveTM, Covidien, Minneapolis, US) before it was placed into the wound. Using the 30-degree 3-mm thoracoscope (Karl-Storz GmbH & Co., Tuttlingen, Germany) and a VATS double-hinged 5-mm shaft diameter node grasper (Scanlan International Inc., US) for lung retraction, the pleural cavity was inspected and the lesion identified. An 1,350-nm wavelength diode laser (Biolitec, Jena, Germany) conducted through a 0.6-mm diameter catheter was fed through the lumen of a rigid 2-mm endosuction tube, which was also connected to suction via a three way tap (Figure 1) and inserted into the chest. Minor adhesions were divided by the laser, followed by laser lung wedge resection of the lesion (Figure 2) (7). The lesion was removed using a protective bag, and the frozen section was benign. Underwater test for airleak was negative. Retrieval of the Alexis retractor was facilitated by pulling on the pre-tied O-silk (Figure 3) (8). A 24 Fr chest drain was placed through the same wound towards the apex, secured, and the incision was closed routinely. The chest drain was removed the following day and discharge on the same day without complications. Follow-up 2 weeks after the procedure was unremarkable with the final pathology showing benign granulomatous inflammatory nodule.


Comments
Recently, advances in the development of smaller endostapler-cutters for pulmonary hilar vessels have allowed improved maneuverability, less instrument fencing, and smaller surgical incision during uniportal VATS. However, endostapler-cutters used for lung parenchyma division are larger and their sizes have not changed significantly in recent years. During uniportal VATS wedge lung resections, when small diameter thoracoscope and endoscopic or double hinged VATS instruments are used, the endostapler-cutter becomes the largest instrument by diameter that occupies the incision. Thus, a narrower instrument that can mimic the cutting, pneumostatic and haemostatic properties of the endostapler-cutter may permit a smaller uniportal incision to be made for lung wedge resection. Uniportal VATS lung wedge resection using laser conducted by a narrow catheter may provide such solution. The use of lasers in thoracic, in particular airway surgery is well established. Different properties of tissue determine the ideal laser wavelength absorption that produces the desired local effects of cutting, coagulation and hemostasis, tissue vaporization, and for lung parenchyma pneumostasis. The 1,350-nm wavelength diode laser is highly absorbed by lung parenchymal tissue producing an excellent balance between cutting, hemostasis, and pneumostasis making it ideal for limited lung resections. The laser catheter in our case was fed through a 3-mm narrow bore suction catheter to provide control of the direction of the laser tip as well as for suctioning of the smoke generated during laser resection. In our experience, the immediate disadvantages of using the laser for lung resection is first of all the relatively slow speed of cutting compared with endostapler, and secondly, the large amount of smoke generated within the pleural space that sometimes needed to be evacuated prior to further use of the laser, therefore the procedural time is longer. In this particular patient, the time required to complete the lung resection with the laser was 5 minutes 20 seconds. Nevertheless, the hemostasis and pneumostasis from the laser resected surface is excellent. Also during these uniportal procedures with incision size of 1 to 1.5 cm, we found that with such a small wound, placing a finger in to pull out and remove the inner ring of the Alexis retractor is a challenge, and many a times not physically possible. Therefore, we have adopted tying a thick silk tie to the inner rubber ring to facilitate easy removal at the end of the procedure. Although the manufacturer’s data suggest the 1,350-nm diode laser can satisfactorily seal airway and vessels up to 2 mm in diameter, questions about how deep or large a wedge can be safely performed in the clinical setting will need further investigation. In the future, laser surgery for limited lung resection may potentially have a role in select patients within the family of diverse approaches to uniportal VATS (9). More experience and prospective studies will be needed to better define its application.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
References
- Ng CSH. Uniportal VATS in Asia. J Thorac Dis 2013;5:S221-5. [PubMed]
- Rocco G, Martucci N, La Manna C, et al. Ten-year experience on 644 patients undergoing single-port (uniportal) video-assisted thoracoscopic surgery. Ann Thorac Surg 2013;96:434-8. [Crossref] [PubMed]
- Rocco G, Martin-Ucar A, Passera E. Uniportal VATS wedge pulmonary resections. Ann Thorac Surg 2004;77:726-8. [Crossref] [PubMed]
- Ng CS, Wong RH, Lau RW, et al. Single port video-assisted thoracic surgery: advancing scope technology. Eur J Cardiothorac Surg 2015;47:751. [Crossref] [PubMed]
- Ng CS, Rocco G, Wong RH, et al. Uniportal and single-incision video-assisted thoracic surgery: the state of the art. Interact Cardiovasc Thorac Surg 2014;19:661-6. [Crossref] [PubMed]
- Ng CS, Wong RH, Lau RW, et al. Minimizing chest wall trauma in single-port video-assisted thoracic surgery. J Thorac Cardiovasc Surg 2014;147:1095-6. [Crossref] [PubMed]
- Ng CS, Capili F, Zhao ZR, et al. Laser resection of pulmonary nodule via uniportal thoracoscopic surgery. Asvide 2017;4:114. Available online: http://www.asvide.com/ articles/1424
- Ng CS, Capili F, Zhao ZR, et al. Laser resection of pulmonary nodule via uniportal thoracoscopic surgery. Asvide 2017;4:115. Available online: http://www.asvide.com/ articles/1425
- Ng CS. Uniportal video-assisted thoracic surgery: a look into the future. Eur J Cardiothorac Surg 2016;49 Suppl 1:i1-2. [PubMed]


