Low grade myxofibrosarcoma in the right ventricle presenting as pulmonary thromboembolism
Introduction
Primary malignant cardiac neoplasms are uncommon, with more than 75% of primary malignant cardiac tumors being sarcomas. Myxofibrosarcoma is a rare primary cardiac sarcoma that commonly arises in the left atrium.
Here, we describe a patient with myxofibrosarcoma in the right ventricle and pulmonary arteries that initially presented as pulmonary thromboembolism.
Case report
A 78-year-old male with a history of chronic thromboembolic pulmonary hypertension 6 months previously presented with aggravated dyspnea. Chest computed tomography performed 6 months previously showed a large low-density lesion from the right main pulmonary artery to the lobar pulmonary arteries, and echocardiography revealed mild pulmonary hypertension (systolic pulmonary artery pressure =50 mmHg) with no evidence of an intracardiac lesion. Despite applying anticoagulation, repeated chest computed tomography revealed that the low-density lesion in pulmonary arteries progressed and that another low-density lesion had newly developed in the right ventricle. The patient refused surgical management.
The patient was admitted 6 months later with aggravated dyspnea. His blood pressure, pulse rate, respiratory rate, and body temperature on presentation were 100/70 mmHg, 107 min−1, 20 min−1, and 36.7 °C. Laboratory findings showed a white blood cell count of 19,600/L, hemoglobin at 13.1 g/dL, a platelet count of 42,000/µL, D-dimer at 1.47 µg/mL, and pro-BNP at 11,793 pg/mL.
Echocardiography showed dilated right atrium and right ventricle and severe right ventricular dysfunction with severe tricuspid regurgitation, and the systolic pulmonary artery pressure exceeded 80 mmHg. A round mass with a size of about 2 cm in the right ventricular outflow tract was impeded blood flow to the pulmonary artery (Figure 1).
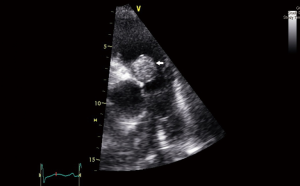
The low-density lesion was again noted in the right ventricle, and other low-density lesions in the pulmonary artery had progressed to extend into both pulmonary arteries and the right descending interlobar and lobar pulmonary arteries in chest computed tomography (Figure 2). Multifocal pulmonary infarctions were noted in both upper lobes, especially in the right upper lobe, and a perfusion scan demonstrated progression of a large perfusion defect area in the right lung and a subsegmental perfusion defect in the anterior segment of the left upper lobe.
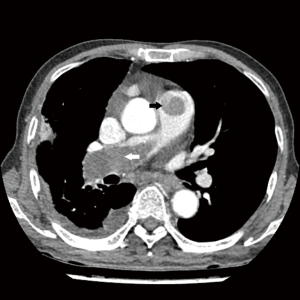
Venoarterial extracorporeal membrane oxygenation (ECMO) was applied due to the progression of right-side heart failure with severe pulmonary hypertension, which resulted in improvement of the right-side heart failure.
After median sternotomy, ascending aorta and superior vena cava were prepared for cannulations. Previous femoral venous cannula for ECMO was used for inferior vena cava cannulation. The aorta is clamped and cold crystalloid cardioplegia was infused through an aortic root cannula. Main pulmonary artery and both pulmonary arteries were opened in a T shape longitudinally and incision was extended to right ventricular outflow tract.
Exploration of the cardiac and pulmonary arteries revealed a yellow and glistening mass with a size of about 3 cm in the right ventricular outflow tract just below the pulmonary valves and which infiltrated the endocardium (Figure 3). Other separate lobulated masses obstructed and invaded the right and left main pulmonary arteries. The right ventricular outflow tract and pulmonary arterial obstructions were relieved with the removal of masses.
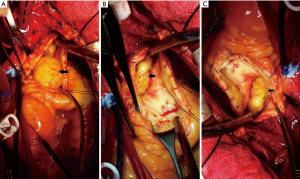
Histologically, the tumor was predominantly myxoid and had elongated, curvilinear capillaries. The nuclei were hyperchromatic and mildly pleomorphic, with only rare mitotic figures (Figure 4). The tumor cells were immunonegative for CD31, S-100, desmin, epithelial membrane antigen, and CD34, and focally positive for actin. The right ventricular mass was demonstrated to be a low-grade myxofibrosarcoma and was consistent with the pulmonary artery masses.
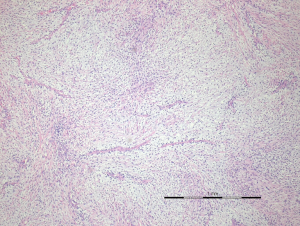
The pulmonary artery pressure decreased immediately after the operation, but the patient died at postoperative day 5 due to progression of the right-side heart failure.
Discussion
Primary cardiac tumors are uncommon, with 75% being benign and 25% being malignant. Among primary malignant cardiac neoplasms, approximately 75% are sarcomas that present with various clinical manifestations, including obstructing blood flow, embolism, pericardial effusion, arrhythmias, and generation of substances that result in constitutional systemic symptoms (1).
The most common primary malignant cardiac neoplasms are sarcomas with myofibroblastic differentiation, which mostly arise in the left atrium. Angiosarcomas are the most common, followed by rhabdomyosarcomas, malignant mesotheliomas, and fibrosarcomas (2).
Left-heart sarcomas are solid and exhibit less infiltration than right-heart sarcomas, and tend to metastasize later during the disease course. Right-heart sarcomas tend to metastasize early, present as larger masses, occupy the right atrium as bulky mass, and heart failure is the latest presentation.
Myxofibrosarcomas are tumors of mesenchymal origin that commonly affect the extremities of elderly patients and occur frequently in dermal or subcutaneous tissues (3). They have high rates of local recurrence and distant metastasis. Their histologic features include a nodular growth pattern, a myxoid matrix containing elongated capillaries, fusiform, round, or spindle cells with indistinct cell margins, a slightly eosinophilic cytoplasm, and a hyperchromatic atypical nuclei. These lesions are categorized from low-grade neoplasms with a hypocellular, mainly myxoid, and spindle-cell appearance, to high-grade neoplasms with pleomorphic lesions with multinucleated giant cells, high mitotic activity, and areas of necrosis. A low-grade myxofibrosarcoma tends to metastasize locally, requiring wide surgical resection, while high-grade myxofibrosarcomas invade local and adjacent tissues and are associated with distant metastasis to the lung, bone, brain, and lymph nodes.
A cardiac myxofibrosarcoma occurs in the endocardium and can arise in any one of the four chambers of the heart and also occur in valvular and vascular structures. The left atrium is the most common location (4), followed by the right atrium, right ventricle, and ventricular septum. A rare case of primary myxofibrosarcoma in the aorta has also been reported (5). Myxofibrosarcomas are considered to originate from myofibroblasts. Microscopically, the tumor cells represent fibroblastic differentiation with secretory activity within a myxoid matrix, and they are composed of spindle or rounded cells within a myxoid matrix, without significant pleomorphism.
In our patient, the right ventricular mass was confined to the endocardial surface of the right ventricular outflow tract and it was clearly separated with the masses of pulmonary arteries. The initial clinical presentation as pulmonary thromboembolism rather than the mass effect in the right ventricle reflects the distinct features of early local metastasis of low-grade myxofibrosarcoma. Pulmonary artery sarcomas often present with pulmonary artery obstruction and can be mistaken for chronic pulmonary embolism, as in our case for both the clinically and imaging findings. Dang et al. (5) reported the aortic myxofibrosarcoma that mimicked a thrombus. A myxofibrosarcoma is a hypovascular neoplasm that does not exhibit contrast enhancement, and it could be confused with a thrombus.
Initially the patient was treated with anticoagulation under diagnosis of pulmonary thromboembolism. Despite anticoagulation, pulmonary lesions were progressed. Surgical treatment was recommended for the differentiation of pulmonary artery sarcoma and pulmonary embolism, but patient refused.
Complete surgical resection is important for prolongation of survival. But, complete resection is very difficult and it occurs in only about one third of cases. Shiga et al. (6) reported a large myxofibrosarcoma of the right ventricle in a 56-year-old male which obstructed the right ventricular outflow tract. Though the mass was extended into right pulmonary artery, they did not show the local or distant metastasis and the mass was resected successfully. However, the local metastasis and diffuse infiltration into endocardial surface and both pulmonary arteries in our case made complete resection impossible. Radiotherapy and chemotherapy can be considered in case of residual lesions or high-grade tumors, but, the role of radiotherapy and chemotherapy is uncertain. The exact prognosis of cardiac myxofibrosarcoma has not been elucidated; the outcomes of cardiac myxofibrosarcomas are usually disappointing.
Our patient had a rare case of cardiac myxofibrosarcoma which arising from the endocardial surface of right ventricle and it initially presented with pulmonary thromboembolism. Myxofibrosarcoma of the heart is very uncommon and has regional and distant metastatic potential. Therefore, it should be considered in the differential diagnosis of pulmonary thromboembolism.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
References
- Selke F, del Nido P, Swanson S. Sabiston and Spencer Surgery of the Chest. 9th edition. Amsterdam: Elsevier 2015;2:1845.
- Silverman NA. Primary cardiac tumors. Ann Surg 1980;191:127-38. [Crossref] [PubMed]
- Mentzel T, Calonje E, Wadden C, et al. Myxofibrosarcoma. Clinicopathologic analysis of 75 cases with emphasis on the low-grade variant. Am J Surg Pathol 1996;20:391-405. [Crossref] [PubMed]
- Sanchez-Uribe M, Retamero JA, Gomez Leon J, et al. Primary intermediate-grade cardiac myxofibrosarcoma with osseous metaplasia: an extremely rare occurrence with a previously unreported feature. Cardiovasc Pathol 2014;23:376-8. [Crossref] [PubMed]
- Dang D, Rosado-de-Christenson ML, Suster SM. Primary aortic myxofibrosarcoma mimicking thrombus: findings on CT, MRI, and angiography. J Thorac Imaging 2009;24:125-8. [Crossref] [PubMed]
- Shiga Y, Miura S, Nishikawa H, et al. Very rare case of large obstructive myxofibrosarcoma of the right ventricle assessed with multi-diagnostic imaging techniques. Intern Med 2014;53:739-42. [Crossref] [PubMed]


