Video-assisted thoracic surgery right sleeve lobectomy
Introduction
In recent years, lung cancer has become the leading malignant tumor in terms of morbidity and mortality in many countries around the world (1). The pneumonectomy plus systemic mediastinal lymph nodes dissection is one of the major lung cancer treatments which contribute to survival benefit for many lung cancer patients (2). In selective patients, either intentional or compromised sleeve lobectomy, instead of pneumonectomy, could obtain better quality of life and adjuvant treatment compliance after radical tumor dissection, which has been widely recognized by thoracic surgeon (3). Many multiple-institutional trials have already reported that video-assisted thoracic surgery (VATS) pulmonary lobectomy plus systemic mediastinal lymph nodes dissection could obtain comparable and even more satisfactory immediate and long-term therapeutic results than traditional thoracotomy. Therefore, VATS has already been accepted by National Comprehensive Cancer Network (NCCN) as one of surgery candidates for lung cancer since 2006. With increasing and improving experience, more VATS lung-sparing lobotomy with bronchoplasty and/or angioplasty has be performed in selected patients, but there is still no standard and widely accepted surgical procedure.
Operative techniques (Figure 1)

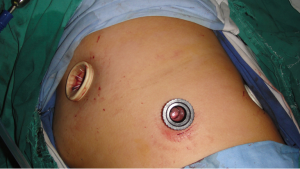
Patient and trocar position (Figure 2)
The patient was set in the lateral position with the arm hanging down. The surgeon stood at the abdominal of the patient. After single lung ventilation, three trocars were inserted:
- Ten mm trocar in the 7th intercostal space in the mid-axillary line for the scope camera (Storz, 30 degree);
- A total of 15 mm trocar in the 8th intercostal space in the scapula line, for the endostaple (Covidien, Mansfield, MA, USA) and other instruments such as grasping forceps, Harmonic scalpel and suction;
- Four cm length trocar was inserted in the 4th intercostal space in the anterior axillary line, and this port for the main operation, such as grasping, dissection, suction, specimen extraction, and suturing.
Mobilization and dissection of the upper lobe branch of the right superior pulmonary vein
The upper lobe branch of the right superior pulmonary vein was dissected after dividing of the parietal pleura anterior to the phrenic nerve; the adjacent middle lobe vein must be carefully preserved. When the upper, lower, and anterior borders were dissected out, the vein was encircled with a right-angled clamp and transected with an endoscopic vascular stapler (Covidien, 2.5 mm). The ongoing pulmonary artery that lies directly posterior to the vein must be carefully avoided.
Mobilization and dissection of the truncus anterior branch of the right pulmonary artery
Grasping the divided vein end, the ongoing pulmonary artery was dissected out. Dividing the pulmonary artery adventitial, the superior and inferior border of the truncus anterior branch was dissected. The plane between the right upper bronchus and the truncus anterior branch artery was then carefully developed. This is a difficult area to repair if injured. Once the plane developed, the artery was encircled with a right-angled clamp and transected with an endoscopic vascular staple (Covidien, 2.5 mm) through the 8th intercostal space trocar in the scapula line.
Dissection of the horizontal fissure with harmonic scalpel
We divided the minor fissure between the right upper and middle lobe that were almost complete with harmonic scalpel.
Mobilization and dissection of the superior segmental anterior of the right lower lobe
After dividing the minor fissure, the posterior ascending branch arising from the superior segmental artery of the right lower lobe was dissected. The posterior ascending branch could not be freely mobilized because the take-off of the artery was entirely invaded by the tumor. Then the superior segmental artery of the right lower lobe was carefully dissected out. Being retracted with 1-0 silk, the artery was then divided with an endoscopic vascular stapler (Covidien, 2.5 mm) through the 8th intercostal space trocar in the scapula line.
Dissection of the #7 and #8 stations of mediastinal lymph nodes
Grasping upwards the right lower lobe gently, the right inferior pulmonary ligament up to the inferior pulmonary vein and parietal pleura anterior to the esophagus was divided with electrocautery. When the esophagus was kept retracted posteriorly and the lung anteriorly, the #7 and #8 stations of mediastinal lymph nodes were entirely dissected with Harmonic. The dissection was carried out along the border of the left and right main stem bronchus, pericardium, and esophagus, which should be carefully reserved to avoid inadvertent injury. Bronchial and esophageal arterial branches were carefully clipped with Harmonic. The posterior aspect of the major fissure were thick and incomplete, it was divided with endoscopic stapler (Covidien, 4.8 mm) through the 4th intercostal space trocar in the anterior axillary line.
Extraction of the specimen
The 11th lymph nodes adjacent to the intermediate bronchus were dissected with Harmonic. When all the lymph nodes was swept off the bronchus or up into the specimen, the right main bronchus and intermediate bronchus was mobilized and cut off respectively with scissor. The specimen was packed into a 7.5 size glove and then extracted through the 4th intercostal space incision in the anterior axillary line. The proximal and distal bronchus resection margins were checked to be pathology negative in the intraoperative frozen section analysis.
Anastomosis of the bronchus ends
The anastomosis between the right main bronchus and intermediate bronchus ends (end-to-end anastomosis) were performed carefully by running and circumferential suture technique with one 3-0 non-absorbable prolene suture (BRAUN). The first suture was begun at the membranous and cartilaginous junction portion. The suture was tightened by nerve hook when the posterior wall of the anastomosis was completed. Then the suture of the anterior wall was performed. When the whole anastomosis was completed, we tightened and tied the suture. Finally, the right middle and lower lobes were inflated to ensure that the anastomosis and airway were air leaks free.
Dissection of the #2 and #4 stations of mediastinal lymph nodes
After dividing the parietal pleura posterior to the superior vena cava and superior to the azygos vein with electrocautery, the #2 and #4 stations of mediastinal lymph nodes were entirely dissected with Harmonic. The right recurrent nerve should be carefully preserved to avoid injury and the small venous branches off the superior vena cava were carefully clipped with harmonic.
Completion of the procedure
When the sleeve lobectomy and radical lymphadenectomy were completed, the right middle lobe and lower lobe received reventilation. The chest tube (24F) was administrated through the camera port in the 7th intercostal space and the tip of the tube was kept in the cavity of the removed right upper lobe (RUL).
Comments
Compared to pneumonectomy, sleeve lobectomy (more technically demanding) can obtained lower associated morbidity and mortality together with more satisfactory cardiopulmonary function and comparable long-term outcome (1,5). VATS sleeve lobectomy developed in recent years for lung cancer in selected patients is proven technically feasible and safe. Various suture material and technique for the bronchus anastomosis are proven feasible. The running and circumferential suture technique for end-to-end bronchus anastomosis with the material of one 3-0 non-absorbable prolene suture which could be easily tightened by nerve hook is proven to be ease, feasible, safe and time-saving, and the kinking of the suture which should be especially carefully avoided in VATS is the main pitfall of the procedure. We do not consider the encirclement of the anastomosis in sleeve lobectomy is necessary even after the skeletonizing of the bronchus. The suture technique performed in the video could simplify the procedure. With increasing experiences, more VATS lung-sparing surgeries should be encouraged to be performed in selected patients in high volume lung cancer centers.
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- Siegel R, Ma J, Zou Z, et al. Cancer statistics, 2014. CA Cancer J Clin 2014;64:9-29. [PubMed]
- Ginsberg RJ, Rubinstein LV. Randomized trial of lobectomy versus limited resection for T1 N0 non-small cell lung cancer. Lung Cancer Study Group. Ann Thorac Surg 1995;60:615-22. [PubMed]
- Parissis H, Leotsinidis M, Hughes A, et al. Comparative analysis and outcomes of sleeve resection versus pneumonectomy. Asian Cardiovasc Thorac Ann 2009;17:175-82. [PubMed]
- Xiong F, Wang S, Kai J. Video-assisted thoracic surgery right sleeve lobectomy. Asvide 2014;1:365. Available online: http://www.asvide.com/articles/399
- Stallard J, Loberg A, Dunning J, et al. Is a sleeve lobectomy significantly better than a pneumonectomy? Interact Cardiovasc Thorac Surg 2010;11:660-6. [PubMed]