Major morbidity after video-assisted thoracic surgery lung resections: a comparison between the European Society of Thoracic Surgeons definition and the Thoracic Morbidity and Mortality system
Introduction
Complication rates following video assisted thoracoscopic surgery (VATS) lobectomy for lung cancer range between 6% and 34.2% and the mortality rate ranges between 0.6% and 1.3% (1-3). To date, there is no standardization for their classification. Postoperative complications are directly related to treatment effectiveness, prognosis, hospitalization costs and patients’ quality of life. The objective of this study was to verify whether those complications, traditionally classified as major cardiopulmonary complications according to the European Society of Thoracic Surgeons (ESTS) definition (4) and used as such in outcome analyses, were also classified as major according to the thoracic morbidity and mortality (TM&M) grading system (5,6).
Materials and methods
We retrospectively retrieved clinical and surgical information of 227 consecutive patients submitted to VATS lobectomies for lung cancer in our Institution, in the period comprised between August 2012 and October 2014. Patients’ baseline and surgical characteristics are shown in Table 1. Within this cohort, the analysis was performed on those patients who faced at least one postoperative complication.
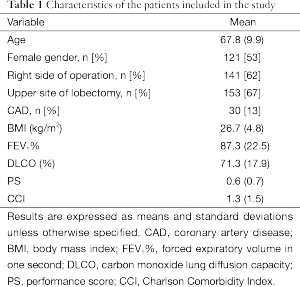

Full table
Board qualified thoracic surgeon performed all the procedures through a 2-3 ports VATS access. As a rule, all patients were extubated in the operating room and were transferred to a high dependency unit (HDU) where they spent the first night after the operation and from which were then moved to a dedicated thoracic ward bed. Inoperability criteria were a predicted postoperative forced expiratory volume in one second (ppo-FEV1) and predicted postoperative carbon monoxide lung diffusion capacity (ppo-DLCO) <30% in association with a VO2max <10 mL/kg/min, according to existing guidelines (7).
All patients were managed according to standardized pathways of care, including as early as possible mobilization, chest physiotherapy and rehabilitation, and venous thromboembolism (VTE) prophylaxis.
Pain control was achieved with a combination of a paravertebral catheter and intravenous patient controlled analgesia, with the aim of maintaining the numeric pain score consistently below 4 in a visual analogic scale (VAS).
In 18 cases the VATS procedure was converted into an open one due to complications that arose during the intervention (e.g., bleeding, major air leak) or for safety reasons (e.g., difficult dissection of vessels/fissure due to big lymph nodes or tumor), and were not excluded from the study according to the intention to treat model of the analysis.
Definitions of complications
TM&M classification system
Seely and colleagues developed the TM&M system in 2010 (5,6), based on the Clavien-Dindo classification (8). Regardless the type of complication, this system proportionally grades each postsurgical complication in the I to V scale according to the complexity of its management. Grades I and II include minor complications requiring no therapy or pharmacologic intervention only. Grades III and IV are major complications that require surgical intervention or life support. Grade V complications result in patient death as illustrated in Table 2.

Full table
European Society of Thoracic Surgery (ESTS) definitions of major cardiopulmonary complications
The ESTS Database Committee definitions of major cardiopulmonary complications, as published in the ESTS Silver Book (4), include “pneumonia”, “atelectasis requiring bronchoscopy”, “adult respiratory distress syndrome (ARDS)”, “mechanical ventilation >24 h”, “pulmonary oedema”, “pulmonary embolism”, “myocardial infarct”, “cardiac failure”, “arrhythmia”, “neurological complications (stroke)”, “acute renal insufficiency” and “deep vein thrombosis (DVT)”.
Design of the study
Firstly, all the identified postoperative complications of the cohort were classified according to the definitions proposed by the ESTS Database Committee. Subsequently, all the postoperative complications recorded were graded according to the TM&M classification system. In case a patient had multiple concurrent complications, only the most severe one was considered. A comparison of complications’ severity distribution between the two groups was then performed.
The postoperative length of stay (LOS) was also analyzed. Descriptive statistics was utilized. Results are reported as means and standard deviation for numeric variables or frequency of occurrence for categorical variables. The statistical analysis was performed on STATA 12.0 statistical software (STATA Corp. College Station, TX).
Results
The total number of postoperative complications among the 227 patients included in this study was 34 (15%). Twenty patients (8.8% of the total population) were affected by major cardiopulmonary complications according to the ESTS definitions, such as: “atrial fibrillation (AF)”: #10 (50%); “ARDS”: #1 (5%); “pulmonary embolism:” #2 (10%); “mechanical ventilation >24 h”: #1 (5%); “pneumonia”: #3 (15%); “myocardial infarct”: #1 (5%); “atelectasis requiring bronchoscopy”: #2 (10%) (Table 3). This incidence accounts for 59% of the total complications recorded in this series.
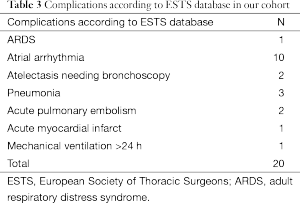
Full table
According to the TM&M system, 10 patients had minor complications (grades I and II), while 24 patients (11% of the total population) developed major complications, including 3 deaths (grade V). This group of major complications represents 71% of all complications (Table 4).

Full table
Nine postoperative complications considered as major according to the ESTS DB classification were reclassified as minor complications (grade II) by the TM&M system. They represent 45% of all major cardiopulmonary complications, which were recoded as minor by the TM&M system. These patients’ characteristics, including the in-hospital median LOS, are evidenced in Table 5.

Full table
A total of 14 other complications, including surgical ones, occurred. Thirteen were considered as major complications and one minor according to the TM&M system.
Of the 18 VATS lobectomies converted to an open procedure, three patients faced postoperative complications and were classified as such by the TM&M classification: 1 minor complication (grade II), 1 major complication (grade IVb) and 1 death (grade V).
The analysis of the postoperative LOS between the two groups evidenced a 12-day difference in the LOS between the patients who remained classified in the ESTS major complication group after the TM&M recoding and the patients reclassified in the minor complication group according to it (21.6 vs. 9.6 days; Mann Whitney Test P=0.08).
Discussion
Clinical background and rationale for the study
Postoperative complications are often used as primary endpoint for outcome analyses. In fact, as they are directly related to prognosis and treatment efficacy, at the same time they may be utilized as indirect indicators of the quality of surgical treatment given to the patient, hospitalization cost and patients’ quality of life following surgery (9,10). In a time in which minimally invasive surgical procedures (VATS) are increasingly adopted worldwide, along with the aim of decreasing patients’ hospitalization, an appropriate, accurate and standardized measurement and monitoring of adverse events following surgery becomes of utmost importance.
It is of evidence that VATS lung resections for lung cancer reduces overall postoperative complications, acute and chronic pain and loss of pulmonary function when compared to standard open technique (11). For this reason, the American College of Chest Physicians (ACCP) recommends VATS lobectomy as the procedure of choice for clinical stage I non-small cell lung carcinoma (12). Perioperative complications and mortality in patients submitted to VATS lobectomy for lung cancer is low, yet not negligible (1-3).
The ESTS classification system identified a series of frequent and potentially life threatening complications while TM&M classification system does not discriminate between the types of complication occurred, but weighs each complication through a grading system that takes into account the effort required to treat them.
Main findings
Through this study we aimed to evaluate potential inconsistencies between the coding of postsurgical complications following minimally-invasive lung resections for cancer according to the ESTS definitions and the TM&M classification.
Nearly 60% of the complications occurred in our cohort of patients submitted to VATS lobectomy for lung cancers were classified as major cardiopulmonary complications according to the ESTS definitions, which are the ones most commonly used as outcome indicators for quality of care evaluation. In our series these were mostly represented by atrial arrhythmias. Although potentially cause of morbidity and mortality, 45% of them was reclassified as minor complications according to the TM&M classification, since required just a pharmacological treatment and had a minimal impact on patients postoperative course.
This finding confirms a previous comparative study performed in a population of patients operated by thoracotomy and showing that almost 62% of those complications defined as major by the ESTS definitions were reclassified as minor complications using the TM&M system (9).
The absolute incidence of major complications according to the TM&M system found in our study (11%) is also in line with the one previously reported after open lobectomies and using this classification system (9.3%) (9).
An interesting finding is the large discrepancy in the proportion of major complications found in the present study compared to the one published by Salati and colleagues (9) and including open lobectomies. They found that more than 70% of the complications occurring after open lobectomy were graded as minor complications using the TM&M system, while in our series almost 70% of complications were graded as major. This discrepancy may be explained by the lower absolute incidence of complications observed in our series (15% vs. 34%), which is consistent with the one observed in most of the publications after VATS lobectomy. In particular, several studies have shown a consistent reduction of AF after VATS compared to open lobectomies (13-15) and this may account for a lower proportion of minor complications after VATS.
Due to its nature, the ESTS major cardiopulmonary complication list does not account for the so called surgical morbidity (redo surgery, bleeding, bronco-pleural fistula, surgical emphysema etc.), as omitting the occurrence of a considerable set of complications relatively frequent in our specialty, thus being less accurate. In fact, in our study, 14 complications could not be assessed according to the ESTS classification, but were graded according to the TM&M.
More than half of the complications (55%) considered as major complications according to the ESTS were confirmed so in the TM&M system since they required a complex management.
Limitations
The major potential limitations of this study are its retrospective nature, and the analyses conducted on a small cohort of patients. Its retrospective nature may impact on the data collection affecting its accuracy, especially in identifying the pharmacological treatment used, particularly in those in the case of Grade I and II of the TM&M classification system. On the other hand, the short period of analysis ensured standardization of indication for surgery, treatment of complications and data collection.
The possible inter-observer discrepancy in the classification of the post-surgical complications is reduced due to a prior agreement between surgeons, working in the same centre, as described in the paper by Varela and colleagues (16).
Clinical implications
The classification of the most frequently occurring postoperative complications in thoracic surgery, like the one proposed by the ESTS, is important to standardize the type of treatment of the occurred adverse event, as well as serving the purpose of collecting data for statistical analysis. In particular, major cardiopulmonary complications are frequently selected as endpoint of outcome analyses. For instance, risk adjusted morbidity is one of the parameter compounding the Composite Performance Score used for evaluating the institutional quality of care during the European accreditation process (17,18). Therefore, it appears of critical importance to find a standardized system capable of reliably grade the complications, overcoming one of the most important limitations when dealing with morbidity analysis. The use of TM&M in this regard may be complementary to the traditional classification, or even replace it, if future analyses will confirm its inter-observer stability.
One critical aspect that would warrant further investigation is the correlation between the TM&M grade of complication and other parameters associated with quality of care, such as the postoperative LOS. In fact, we found a 12-day LOS difference between patients who remained classified in the ESTS major complication group after the TM&M recoding and the patients reclassified in the minor complication group according to it.
Finally, a more aggressive attitude toward management of complications (reflected in a higher TM&M grade) would not necessarily mean a poor practice and may in fact lead to a better outcome (reduced failure to rescue).
Conclusions
Postoperative complications are an indicator of quality of care and an important primary endpoint in outcome analysis. The distribution of postoperative major complications between the two classification systems differs. The TM&M system questions the traditional classification of major cardiopulmonary complications following VATS lobectomy, which is currently used for risk-modeling and quality of care analyses. In fact, only 55% of the traditionally defined major cardiopulmonary complications were classified as major by the TM&M grading system due to the complexity of their management. In this regards the TM&M scoring system should be used as an additional instrument for risk-modeling. Only those complications graded greater than II should be selected as endpoints for any future outcome analysis.
Acknowledgements
Paper presented at the Joint Annual Meeting of the Society for Cardiothoracic Surgery in Great Britain & Ireland and the Association of Cardiothoracic Anaesthetists, held in March 2015 in Manchester, UK.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Solaini L, Prusciano F, Bagioni P, et al. Video-assisted thoracic surgery (VATS) of the lung: analysis of intraoperative and postoperative complications over 15 years and review of the literature. Surg Endosc 2008;22:298-310. [PubMed]
- McKenna RJ Jr, Houck W, Fuller CB. Video-assisted thoracic surgery lobectomy: experience with 1,100 cases. Ann Thorac Surg 2006;81:421-5; discussion 425-6. [PubMed]
- Whitson BA, Groth SS, Duval SJ, et al. Surgery for early-stage non-small cell lung cancer: a systematic review of the video-assisted thoracoscopic surgery versus thoracotomy approaches to lobectomy. Ann Thorac Surg 2008;86:2008-16; discussion 2016-8.
- DDatabase report silver book 2011. Available online: http//www.ests.org/documents/PDF/Database_silver_book_2011.pdf. Accessed November 9,2011.
- Seely AJ, Ivanovic J, Threader J, et al. Systematic classification of morbidity and mortality after thoracic surgery. Ann Thorac Surg 2010;90:936-42; discussion 942. [PubMed]
- Ivanovic J, Al-Hussaini A, Al-Shehab D, et al. Evaluating the reliability and reproducibility of the Ottawa Thoracic Morbidity and Mortality classification system. Ann Thorac Surg 2011;91:387-93. [PubMed]
- Brunelli A, Kim AW, Berger KI, et al. Physiologic evaluation of the patient with lung cancer being considered for resectional surgery: Diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 2013;143:e166S-90S.
- Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 2004;240:205-13. [PubMed]
- Salati M, Refai M, Pompili C, et al. Major morbidity after lung resection: a comparison between the European Society of Thoracic Surgeons Database system and the Thoracic Morbidity and Mortality system. J Thorac Dis 2013;5:217-22. [PubMed]
- Bruce J, Russell EM, Mollison J, et al. The measurement and monitoring of surgical adverse events. Health Technol Assess 2001;5:1-194. [PubMed]
- Downey RJ, Cheng D, Kernstine K, et al. Video-Assisted Thoracic Surgery for Lung Cancer Resection: A Consensus Statement of the International Society of Minimally Invasive Cardiothoracic Surgery (ISMICS) 2007. Innovations (Phila) 2007;2:293-302. [PubMed]
- Detterbeck FC, Lewis SZ, Diekemper R, et al. Executive Summary: Diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 2013;143:7S-37S.
- Paul S, Altorki NK, Sheng S, et al. Thoracoscopic lobectomy is associated with lower morbidity than open lobectomy: a propensity-matched analysis from the STS database. J Thorac Cardiovasc Surg 2010;139:366-78. [PubMed]
- Cao C, Manganas C, Ang SC, et al. Video-assisted thoracic surgery versus open thoracotomy for non-small cell lung cancer: a meta-analysis of propensity score-matched patients. Interact Cardiovasc Thorac Surg 2013;16:244-9. [PubMed]
- Burt BM, Kosinski AS, Shrager JB, et al. Thoracoscopic lobectomy is associated with acceptable morbidity and mortality in patients with predicted postoperative forced expiratory volume in 1 second or diffusing capacity for carbon monoxide less than 40% of normal. J Thorac Cardiovasc Surg 2014;148:19-28, dicussion 28-29.e1.
- Varela G, Novoa NM. Evaluation of the interobserver variability in the systematic classification of operative morbidity in lung resection. Arch Bronconeumol 2011;47:581-3. [PubMed]
- Brunelli A, Berrisford RG, Rocco G, et al. The European Thoracic Database project: composite performance score to measure quality of care after major lung resection. Eur J Cardiothorac Surg 2009;35:769-74. [PubMed]
- Brunelli A, Rocco G, Van Raemdonck D, et al. Lessons learned from the European thoracic surgery database: the Composite Performance Score. Eur J Surg Oncol 2010;36:S93-9. [PubMed]


